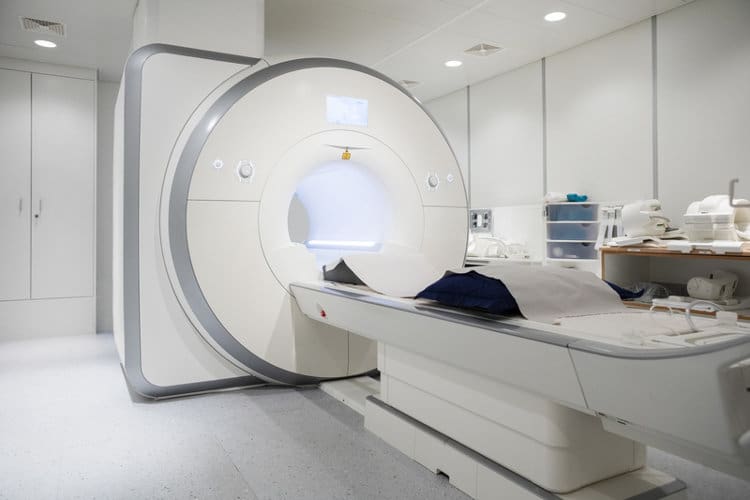
What is an MRI?
An MRI (magnetic resonance imaging) scan is an imaging test that can give very detailed images of the inside of the body. Instead of using X-rays, MRI uses strong magnets, low-energy radio waves and a computer to produce images.
When is an MRI done?
MRI scans can provide detailed pictures of any part of the body. MRI is used when it is considered to be the best test to help diagnose or assess your condition, or when simpler and less expensive tests have failed to give a diagnosis.
MRI is often recommended for imaging the brain and spine because of the detailed, high-quality images it provides. It is also useful in assessing knee injuries and other sports injuries as it is good at showing problems with soft tissues such as muscles, tendons and ligaments.
MRI is often used in addition to other tests, including other imaging tests such as ultrasound. MRI can sometimes show conditions or details that other imaging tests cannot provide.
How does an MRI work?
The strong magnets in the MRI scanner create a magnetic field, which causes the hydrogen atoms in your body to line up in the same direction. Radio waves are then passed into the part of your body being scanned, moving the hydrogen atoms out of alignment. When the radio waves are turned off, the atoms realign, and as they do so they produce radio signals. The signals are transmitted to radio antennae, or receivers, and the computer picks up this information and generates images.
Hydrogen atoms are found in water – H2O – and our bodies have a high composition of water, meaning hydrogen is found throughout the body. Because the hydrogen atoms in different types of body tissue realign at different speeds, they produce different signals. Diseased tissue also gives off a different signal from healthy tissue. This allows the scanner to tell the difference between different tissue types and detect damaged or diseased tissue.
What happens during an MRI scan?
You will be asked to change into a hospital gown and lie on a narrow table. The table will then slide you into the MRI scanner, which looks like an open-ended tunnel or tube. Depending on the part of your body that is being scanned, your head may remain inside or outside the tunnel.
The table doesn’t move during the test and nothing will touch you. Sometimes people report feeling warm during the scan.
When you are in the scanner, you can talk to the staff at any time through an intercom. There is usually a panic button that you can press if you feel very claustrophobic or unwell. Fans will circulate air through the tunnel.
The machine makes knocking noises, which are very loud. You will be provided with earplugs or headphones to protect your hearing. Music can often be played into the headphones to distract you, and some MRI facilities have CD or DVD players, so you can bring your own CDs or DVDs to listen to or watch.
You may be given an injection of a contrast medium or dye (called gadolinium contrast medium) that makes some scans easier to read; this will be discussed before the procedure. You may be asked to hold your breath while some images are being taken.
Once enough images have been obtained, the table will slide out of the tunnel, and you can go and get dressed.
How do I prepare for an MRI?
The magnetic field used in MRI scanning can affect some metal objects, which can be a safety hazard due to the metal heating up, moving, or electronic or mechanical devices malfunctioning. Metal objects can also affect the MRI images.
You should tell the doctor who arranges the test if you have any internal metal devices or implants in your body. Often there will be a form, or safety questionnaire, that you need to fill out before the test, asking specifically if you have any implanted metal devices or objects.
Metal objects may include:
- metal clips on blood vessels in your brain;
- a pacemaker or implanted defibrillator;
- a surgically implanted joint/pin;
- artificial heart valves;
- a deep brain stimulator;
- a cochlear implant;
- magnetic dental implants;
- drug infusion devices;
- an intrauterine contraceptive device (IUD); or
- any metal foreign bodies in your eyes or elsewhere, such as body modification implants and piercings, bullets or shrapnel.
Bear in mind there are implants that do not cause problems during MRI scanning – your doctor or radiographer will be able to work out whether or not it is safe for you to have an MRI.
You will be asked to remove all jewellery, watches, and hearing aids, and to take out any removable dental work. Some wigs contain traces of metal, so these also need to be removed. Some tattoos contain traces of metal, but it is usually still safe to have an MRI. Tattooed skin may feel slightly warm during the scan.
You will also be asked to not wear any makeup or hairspray on the day of the scan, as these products may contain tiny metallic particles that could lead to problems with the scan.
Can I eat or drink before an MRI?
For some scans, such as scans of the abdomen and pelvis, you may be asked to restrict food and drink for a few hours before the test. For others you may be asked to drink a certain amount of water before the test.
MRI scans of the brain or chest areas don’t usually require any special dietary preparation.
If you take regular medication, you should take your medicines as normal unless your doctor has told you not to.
Will it hurt?
MRI scans themselves are painless. However, depending on your condition, you may experience some discomfort or pain from lying in one position for the duration of the scan. The radiographer will work with you to get the most comfortable position possible.
Sometimes medicines or contrast (dye) need to be given through a vein for the test. If this is the case, you’ll need to have a cannula (small tube) inserted in your hand or arm using a small needle. Cannula insertion can be painful, but the pain only lasts a few seconds.
What if I am claustrophobic?
Having an MRI can be slightly uncomfortable for people who are claustrophobic (scared of small or enclosed spaces). You should discuss any concerns with your doctor, and if you think you could not lie still and relax, tell your doctor (and the radiology clinic) beforehand. They can arrange for you to have a sedative medicine before the test to help you stay calm.
You will need to have someone take you home after the test if you have a sedative.
Remember, there is an intercom through which you can communicate with the radiographer (healthcare imaging specialist who performs the test), as well as a button that you can press if you are feeling panicked or unwell.
What are the risks of MRI?
MRI scanning is generally considered to be safe – there is no exposure to radiation and the scan itself has no known harmful effects for most people.
Sometimes people who have had an injection of contrast dye may have an allergic reaction to the dye. In most cases allergic reactions are mild, and in the case of a more severe allergic reaction, you can be given medication to treat it.
People with kidney problems may be at risk of complications related to the gadolinium contrast medium (dye) that may be used during an MRI. Your doctor may recommend having a blood test before the MRI to assess your kidney function.
It has recently been found that a very small amount of some forms of gadolinium contrast medium sometimes remain in the body after the scan. The contrast medium is mainly retained in the bones and tiny amounts in the brain. There are currently no known side effects associated with retained contrast, but radiographers and radiologists are careful to only use contrast when it is needed to make a diagnosis.
If you have any metal objects in your body, this can be a safety hazard during MRI scanning due to the metal heating up, moving, or electronic or mechanical devices malfunctioning. It’s important that your doctor and radiographer are aware of any metal implants or devices that you have, to determine whether it is safe for you to have an MRI.
Can pregnant women have an MRI?
The effects of MRI scanning on a developing fetus are not completely known.
While there have been no reported birth defects resulting from MRI scanning during pregnancy, MRI scans are generally not recommended during pregnancy, especially during the first 12 weeks.
You should tell your doctor if you are pregnant, or think you may be pregnant.
Can children have an MRI?
Children can have MRIs, and MRI is often a good choice of imaging test as there is no exposure to X-ray radiation.
Children younger than about 6 or 7 years may need to have a general anaesthetic for an MRI, as they are generally not able to stay still during the procedure. If your child is having a general anaesthetic, they should not eat or drink anything for 6 hours before the test.
The doctor will discuss the procedure with you and answer any questions. You will be asked to sign a consent form allowing the test to be done.
Parents can often stay in the room with their children while they have an MRI. Parents will need to remove any metal jewellery and clothing containing metal (such as zippers), and will need to confirm that they have no implanted metal objects.
How long does the test take?
The MRI scan may take from 15 to 90 minutes, depending on the type of scan you are having and the number of images taken. You should be told beforehand approximately how long your scan will take.
If you are given a sedative medicine to keep you calm during the scan, you will need to spend extra time at the facility after the scan.
What happens after an MRI?
You can resume normal physical activity and return to work and your usual activities as soon as the test is finished.
The results will be sent to the doctor who referred you for the test, and a follow-up appointment will be made for you to discuss them.
How long does it take to get the results?
After the scans are taken, a radiologist (doctor who specialises in imaging) will review the images and write a report. The report is sent to your doctor, who will discuss the results with you.
Most people should get their results within a week, often sooner. Ask when you have the scan how long the results are likely to take – it can vary depending on the type of scan you are having and whether the scans need to be compared to previous scans.
Further information and support
Talk to your doctor if you are concerned about having an MRI. The hospital or radiology centre where you are having the MRI should also be able to answer any specific questions you have about the test.