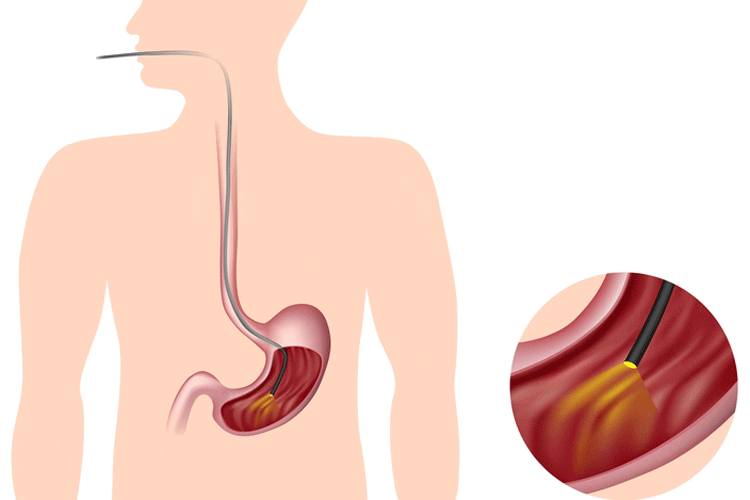
What is a gastroscopy?
Gastroscopy is an examination of the upper digestive tract (the oesophagus, stomach and duodenum) using an endoscope — a long, thin, flexible tube containing a camera and a light — to view the lining of these organs.
Why is a gastroscopy done?
A gastroscopy, also known as an upper gastrointestinal endoscopy or just upper endoscopy, is usually done to investigate the cause of symptoms such as heartburn, abdominal pain, difficulty swallowing, vomiting or bleeding from the digestive tract, and to make or confirm a diagnosis.
Conditions can also sometimes be treated during gastroscopy — for example:
- polyps can be removed;
- enlarged veins (varices) in the oesophagus (food pipe) can be treated to stop and prevent bleeding;
- a narrowed oesophagus can be widened; and
- foreign objects (such as objects accidently swallowed by children) can be removed.
How do I prepare for a gastroscopy?
You will be asked not to eat or drink anything for at least 6 hours before a gastroscopy.
If you are taking any medicines, check with your doctor if it is all right to continue taking them. You may be asked to stop taking medicines that can increase the risk of bleeding for a few days before the test; these include warfarin, aspirin and non-steroidal anti-inflammatory (NSAID) medicines. However, this depends on your individual circumstances, so you should check.
You should also inform the centre performing the gastroscopy if you have any condition that requires you to take antibiotics before dental procedures — you may need antibiotics before gastroscopy too.
Before your gastroscopy, the doctor will discuss the procedure with you and answer any questions, then you will be asked to sign a consent form allowing the test to be done.
What happens during a gastroscopy?
You will be asked to lie flat, usually on your left side. You are usually given a sedative and sometimes a pain-reliever medicine by injection into a vein. The sedative will help you to relax, and may put you to sleep. Generally, you will have little recollection of the procedure. In some cases, the procedure can be done without the sedative – you need to discuss this with the doctor before you sign the consent form.
The back of your throat may be sprayed with a local anaesthetic to make it numb and to help you not to gag. A small mouthguard will be put between your teeth to stop you from biting the endoscope and to protect your teeth. If you have false teeth (dentures) they will need to be removed.
The endoscope will be placed into your mouth and you will be instructed to swallow it down into your stomach. The doctor will direct air into your stomach via the gastroscope. This will make viewing easier.
Sometimes a special instrument can be inserted through the scope, and a small sample of tissue removed (a biopsy). This is not painful. The doctor may also take photos to refer to later.
Some treatments can be performed while the endoscope is in, such as:
- removing polyps;
- controlling blood loss from an ulcer; or
- controlling or preventing bleeding from enlarged veins — similar to varicose veins — in the oesophagus by injecting them with chemicals (sclerotherapy) or placing bands on them (band ligation).
What happens after a gastroscopy?
The procedure takes about 15 to 30 minutes. After the test you will be transferred to a recovery room and a nurse will care for you until you are awake. You can usually go home after about 2 hours.
Make sure you have someone to drive you home as you will still be drowsy after the test. You should not drive and should plan to rest for the remainder of the day.
Although the doctor may briefly run through the findings of the gastroscopy with you once the sedative has worn off, a follow-up appointment is usually made to discuss the test results in more detail.
What are the risks of a gastroscopy?
You may have a slightly sore throat after the procedure. Air may also be trapped in your stomach causing you to feel bloated.
There is a small chance of bleeding after the procedure, especially If a biopsy has been taken or treatment performed. Any bleeding is usually minor.
Very few people experience serious side effects from gastroscopy. Very rarely, the lining of the stomach, oesophagus or duodenum (first part of the small intestine) may be torn, and in such cases you would be admitted to hospital. Surgery may be needed to repair a tear (perforation).
Complications resulting from being sedated are also possible, but again rare.
Your doctor will discuss the risks of the procedure with you and make sure you understand them. They will also tell you what to do if you become unwell after the procedure.
Further information and support
Talk to your doctor or contact the hospital or clinic where you will be having the gastroscopy.