What is amniocentesis?
Amniocentesis is a test that involves inserting a thin needle into a pregnant woman’s belly to take a sample of the fluid around the baby (amniotic fluid). It is possible to tell from the fluid whether a fetus has certain birth defects, such as chromosome abnormalities.
The fluid contains cells from the fetus, which are grown in the laboratory. After careful processing, the chromosomes in the cells are examined and counted.
Chromosomes are the packages of all our genetic material, the blueprint for each of us. The correct number and arrangement of chromosomes are necessary for the development of a healthy individual.
What does amniocentesis show?
Amniotic fluid contains skin cells shed from the fetus and these cells can be used to diagnose chromosomal problems, such as Down syndrome (trisomy 21).
Amniotic fluid also contains alpha-fetoprotein, a substance produced by the fetus. Levels of alpha-fetoprotein may also indicate whether a fetus has problems affecting the spine or other areas of the body.
Is it the right test for you?
Amniocentesis is a prenatal test that helps determine whether a fetus has health problems. The test is usually done at about 15 weeks into the pregnancy. Not every pregnant woman needs this test. Discuss with your doctor or obstetrician whether amniocentesis is right for you.
Should you have amniocentesis?
If the fetus has a higher than normal chance of birth defects or other problems, you may want to have this test. The following risk factors can increase the chances of fetal health problems.
- You are aged 35 years or older.
- There is a history of inherited (genetic) problems in your family.
- Other tests have shown the fetus may have health problems.
Less invasive tests (such as a combined nuchal ultrasound and blood test) are commonly recommended before amniocentesis. If these tests show an elevated risk of Down syndrome or other abnormalities, amniocentesis may be recommended to confirm or exclude chromosomal abnormalities.
There is a risk of miscarriage associated with having an amniocentesis. The risk of miscarriage is generally considered to be less than one per cent.
Your doctor or obstetrician will help you compare the benefits and risks of this test.
How is amniocentesis done?
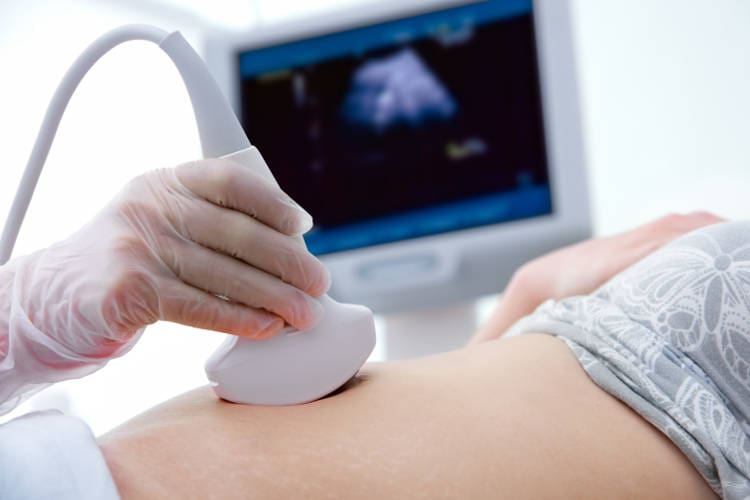
First, the fetus is located using ultrasound (sound waves that make an image on a screen). You may have an injection of local anaesthetic into your skin, and then a thin needle is inserted into your belly. The doctor keeps the needle from touching the fetus by watching the screen. The needle is used to remove a small amount of amniotic fluid from around the developing fetus. Your body will make more fluid to replace what is taken.
You may experience mild pain (like period pain) or a small amount of vaginal bleeding (spotting) straight after having an amniocentesis. You can go home right after the test but you may need to take it easy for a day or so.
After amniocentesis
Call your doctor immediately if you notice:
- severe pain or cramping;
- persistent back pain or abdominal pain (lasting more than a few hours);
- fever or chills;
- vaginal bleeding; or
- fluid leaking from your vagina.
Getting the test results
You will get your amniocentesis results in about 2 weeks.
In special circumstances, preliminary results can be obtained in 2 or 3 days by using a rapid testing method called the FISH technique. However, this tests for only the most common abnormalities, and incurs an extra cost.
Most women’s results are normal. If yours are not, an obstetrician or a geneticist can help you to understand the results and arrange any special care you may need.
It’s your choice
Ask your doctor or obstetrician any questions you have about amniocentesis. Having this test is up to you.