What is Lyme disease?
Lyme disease is a tick-borne illness caused by 4 main Borrelia species of bacteria. The type of black-legged tick that transmits Lyme disease is found in Asia, Europe and North America. Australians who have travelled to these regions and spent time in grassy or heavily wooded areas can be affected by Lyme disease.
There is a growing number of people who believe that Lyme disease occurs in Australia and that they have caught Lyme disease from ticks in Australia. But so far, there is no conclusive evidence that there are ticks in Australia infected with Lyme Disease-causing bacteria.
Lyme disease symptoms
Symptoms can vary depending on where you caught the infection.
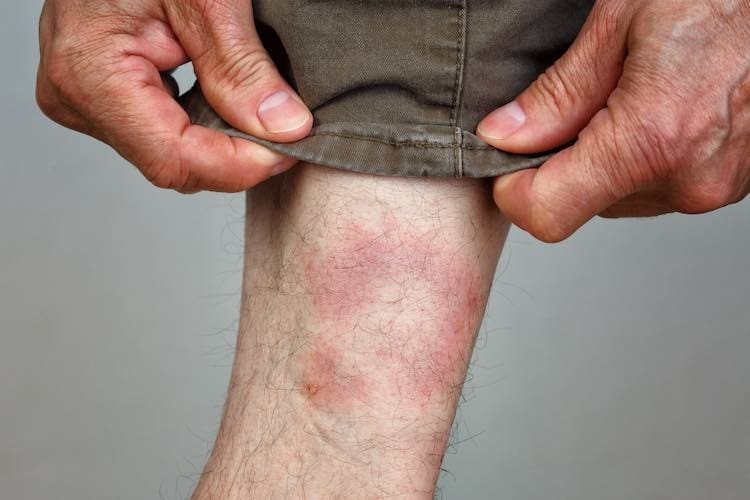
The first symptom in 70-80 per cent of people infected with Lyme disease is a rash called erythema migrans. The rash appears at the site of a tick bite, between 3 and 30 days after being bitten. It starts as a red dot around the bite, and then slowly expands to form a bull’s-eye pattern, with a red outer ring surrounding a clear area in the middle. The rash is not usually itchy or painful.
Sometimes the rash also appears elsewhere on the skin away from the tick bite, which is a sign that the bacteria are multiplying in the bloodstream.
Other Lyme disease symptoms can develop a couple of days to a few weeks after the rash first appears, and include:
- fever;
- headache;
- tiredness;
- joint pain; and
- muscle pain.
In the 20-30 per cent of people who do not develop the hallmark erythema migrans rash, these symptoms may be the only evidence of infection.
Complications
Untreated Lyme disease can be associated with other problems, including:
- ongoing episodes of severe joint pain and swelling;
- fatigue;
- meningitis (inflammation of the membrane surrounding the brain);
- inflammation of the eyes;
- hepatitis (inflammation of the liver);
- short-term memory problems;
- heart problems (such as inflammation of the heart or an irregular heartbeat); and
- nerve problems such as Bell’s palsy (temporary paralysis of one side of the face) or numbness, weakness and shooting pains in the limbs.
It’s possible for some complications to develop months to years after an untreated infection with Lyme disease.
What causes Lyme disease?
Ticks attach themselves to their hosts (humans and other warm-blooded animals) and feed on the host’s blood. As they are feeding, ticks can transmit bacteria to their host. You can catch Lyme disease if you are bitten by a tick that is infected with Borrelia bacteria. In many cases, bites from tiny, immature ticks (called nymphs) cause Lyme disease.
In North America, Borrelia burgdorferi is the main cause of Lyme disease. Borrelia mayonii is a new bacterial species also found to cause Lyme disease in the United States. Borrelia garinii is the main cause of Lyme disease in Asia, while in Europe Borrelia garinii and Borrelia afzelii are the main types of bacteria involved.
Lyme disease is the most common tick-borne illness in North America and Europe. The ticks that cause Lyme disease (black-legged ticks) are often found in grassy and heavily wooded areas, and infections are more common in summer than at other times of the year.
The risk of developing Lyme disease is low if a tick is removed within 24 hours. That’s because ticks need to be attached to your skin for at least 36 hours before the Borrelia bacteria can enter your bloodstream.
Lyme disease cannot be passed from person to person – you can’t catch Lyme disease from someone else.
Diagnosis
If you are concerned about Lyme disease, see your general practitioner (GP). Your doctor will ask you about your symptoms, how long you’ve had them, and whether you have recently travelled anywhere overseas. They will also perform a physical examination, looking for signs of ticks and Lyme disease (such as the characteristic rash), as well as signs of other possible causes of your symptoms.
Diagnosing Lyme disease can be difficult because many of the symptoms and signs are non-specific and similar to those of other conditions, such as the flu and other viral illnesses. The rash is the only symptom that is unique to Lyme disease, but not everyone develops the rash. Also, ticks are very small and their bites are usually painless, so some people may not realise that they have been bitten.
If your doctor thinks Lyme disease is a possibility, they will recommend you have tests. They may also refer you to a specialist in infectious diseases.
Tests for Lyme disease
The following blood tests can help to confirm a diagnosis of Lyme disease. These tests are highly specialised and are not always readily available in all areas. Testing for Lyme disease should be performed by laboratories that have accreditation from the National Association of Testing Authorities (NATA) and Royal College of Pathologists of Australasia (RCPA).
- Enzyme immunoassay (EIA). This test detects antibodies produced by your immune system against the Borrelia bacteria. It is most reliable if performed within 4-6 weeks of suspected infection.
- Western blot test. A second test for antibodies, called a Western blot test, can be done if the EIA test is positive, to confirm the result.
- Polymerase chain reaction (PCR) is a test that can be used to detect DNA from the bacteria that cause Lyme disease.
Sometimes a small sample of skin taken from the skin rash can be sent for testing to see if there is evidence of infection with Borrelia bacteria.
Treatment of Lyme disease
Lyme disease can be treated with antibiotics. The type of antibiotics, how they are given and for how long depends on your symptoms.
People treated promptly in the early stages of the disease usually make a full recovery. When treatment is delayed, the response to treatment may be slower but most people still make a complete recovery.
Additional treatments may be needed if complications such as arthritis develop.
Post-treatment Lyme disease syndrome
Some people with Lyme disease continue to have symptoms after treatment with antibiotics. This is sometimes known as post-treatment Lyme disease syndrome (PTLDS) or post Lyme disease syndrome (PLDS).
Symptoms are usually non-specific and typically include:
- tiredness;
- sleep disturbance;
- problems with memory and concentration;
- joint pain; and
- muscle aches.
The cause of these ongoing symptoms is not known, but they should improve on their own over time. Using antibiotics for an extended period of time has not been shown to be of benefit for ongoing symptoms of Lyme disease, and may actually cause serious side effects. Extended antibiotic use is likely to do more harm than good.
Chronic Lyme disease (CLD) is another term sometimes used to describe persistent Lyme disease-like symptoms. However, some people said to have chronic Lyme disease have not travelled overseas or ever been formally diagnosed with Lyme disease. There is confusion around how the term ‘chronic Lyme disease’ is used and how it is defined, and the existence of this condition is disputed.
Treatment of chronic Lyme disease or Lyme disease-like illness with prolonged courses of antibiotics is not currently supported by evidence from clinical studies and is not recommended.
Lyme disease in Australia
There have been instances of Lyme disease confirmed in Australia, but in these cases the infection was found to have been acquired overseas.
There is currently no evidence that locally-acquired Lyme disease occurs in Australia. The bacteria that cause Lyme disease have so far not been found in Australian ticks. Also, the specific type of tick species that transmits Lyme disease overseas is not found in Australia. However, research and testing are ongoing.
It may be possible that other infections (including as-yet undiscovered types of bacteria) can be transmitted by Australian ticks and cause symptoms similar to those of Lyme disease. There are other illnesses known to be caused by Australian ticks, such as rickettsial infections, Q fever and mammalian meat allergy.
Preventing tick bites
The following precautions can help prevent you from being bitten by a tick. Follow these steps when going outdoors, especially in grassy or heavily wooded areas.
- Wear clothes that fully cover your arms and legs.
- Tuck your shirt into your trousers, and tuck your trousers into your socks.
- Wear a wide-brimmed hat.
- Apply insect repellent that contains DEET to clothes, hats and skin.
- Brush clothing before going back inside to remove ticks that may be on your clothes.
- Shower and check for ticks soon after being outdoors in areas known to have ticks.
Removing a tick
If you have a tick attached to your skin, the aim is to kill and remove it. Australian experts and ASCIA (the Australasian Society of Clinical Immunology and Allergy) recommend the following steps for removing a tick.
- Use a freezing product that contains ether (such as Medi Freeze Tick Off or Tick Tox, available from pharmacies) to kill the adult tick on your skin. Then allow the tick to drop off – this should happen within 24 hours. Take care not to compress or squeeze the tick during this time.
- When the tick has dropped off, clean the area with an antiseptic or soap and water.
Removing a tick in this way may reduce your risk of tick-borne illnesses or developing an allergy to ticks. Alternatively, you can leave the tick in place and see your doctor as soon as possible for removal of the tick.
What not to do
- Don’t use methylated spirits, kerosene or other chemicals, which may cause the tick to inject more toxins and does not help remove ticks.
- Don’t use a lighted match or other hot object to try and kill the tick or detach it. Aside from the risk of burning yourself, this method does not effectively remove ticks.
- Don’t use blunt-nosed household tweezers to remove a tick as they are more likely to squeeze the body of the tick. Fine-tipped tweezers are commonly recommended for removing ticks, but ASCIA recommends avoiding using any type of tweezers to pull out ticks. That’s because they can squeeze the tick and cause it to inject its contents into your skin. Certainly if you are allergic to ticks, do not use tweezers.
- Don’t handle a tick with bare hands, as infective agents or allergens can enter your body through breaks in your skin or by rubbing your eyes. Wash your hands with soap and water if you have touched or handled a tick.
See your doctor if you are having trouble removing a tick or are concerned about tick-borne illnesses.