Aside from wearing ill-fitting shoes or footwear, there are many causes of foot pain. Overuse, injuries and arthritis are common causes. There may be damage to bones, nerves, tendons and ligaments. One in 5 Australians suffers from foot pain. If you have sore feet, read on to explore the most common causes of foot pain.
Symptoms of foot pain
The foot is a complicated anatomical structure that carries the weight of the body, and pain can manifest in different ways depending on the cause. Pain may be in the arch of the foot, along the outer side of the foot, on the sole of the foot, in the ball of your foot, in the toes, heels, ankles or tendons of the foot.
The pain may be an ache, a burning sensation, inflammation or tenderness, or a sharp pain, depending on the cause. It may come and go, depending on your activity.
Here are some of the top 10 causes of foot pain.
Bunions
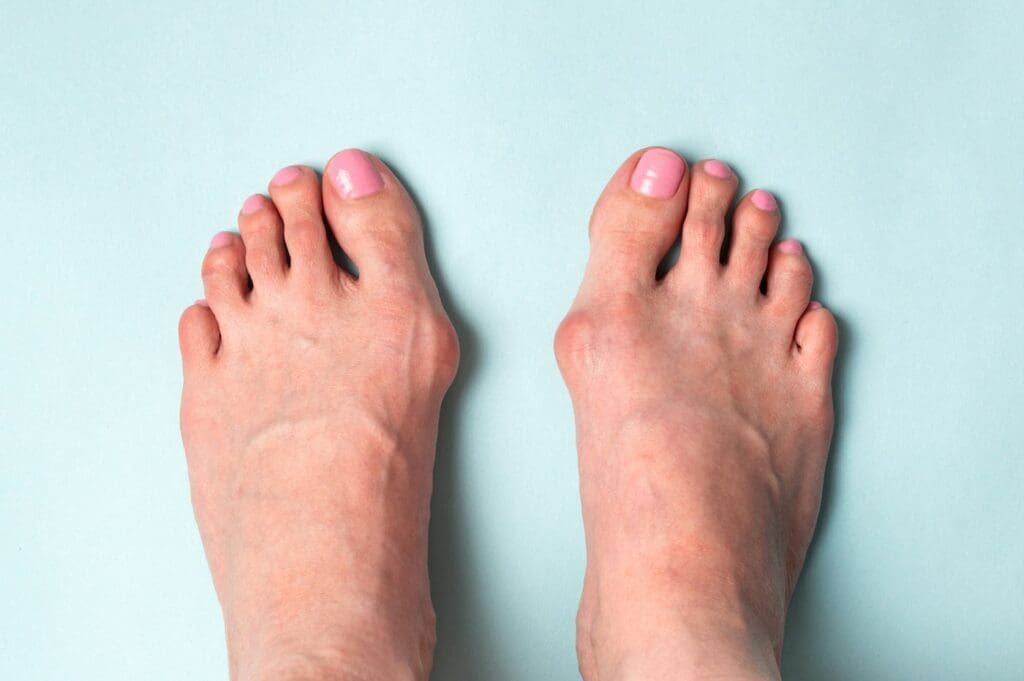
A bunion is an abnormal, swollen bony bump that appears on the joint at the base of the big toe. Bunions often result in pain in the big toe or foot, making wearing shoes and walking painful.
Corns
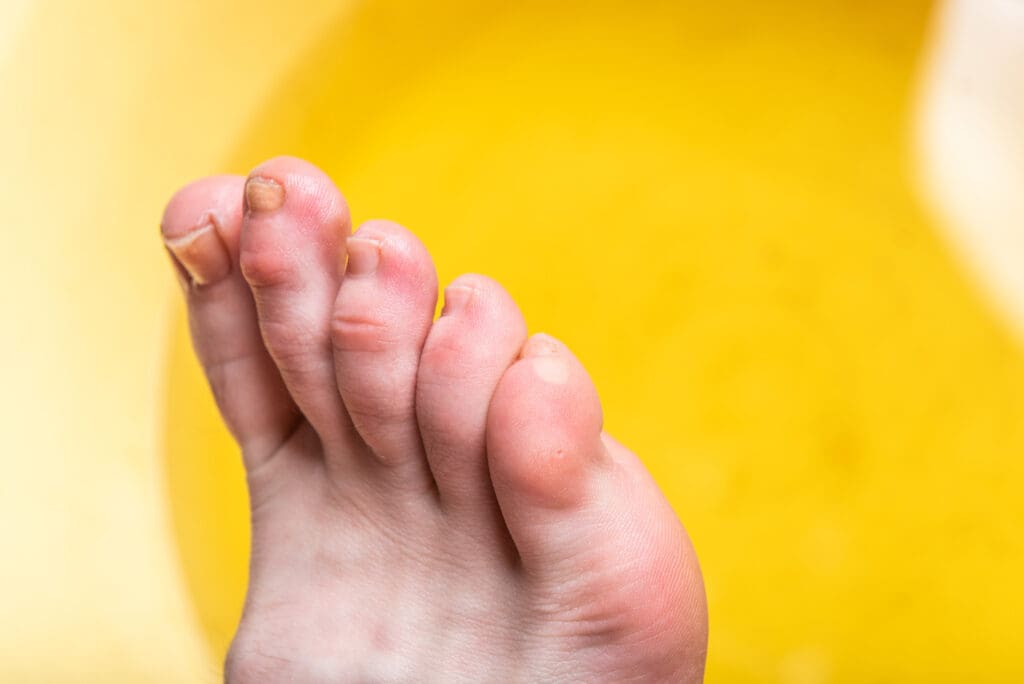
Corns – small, round areas of thickened, hard skin – can result in pain and discomfort in the feet when walking. Corns typically occur on the sides or tops of the toes, but can also affect the sole of the foot. They are caused by pressure and friction on the feet, usually from poorly fitting shoes.
Ingrown toenails
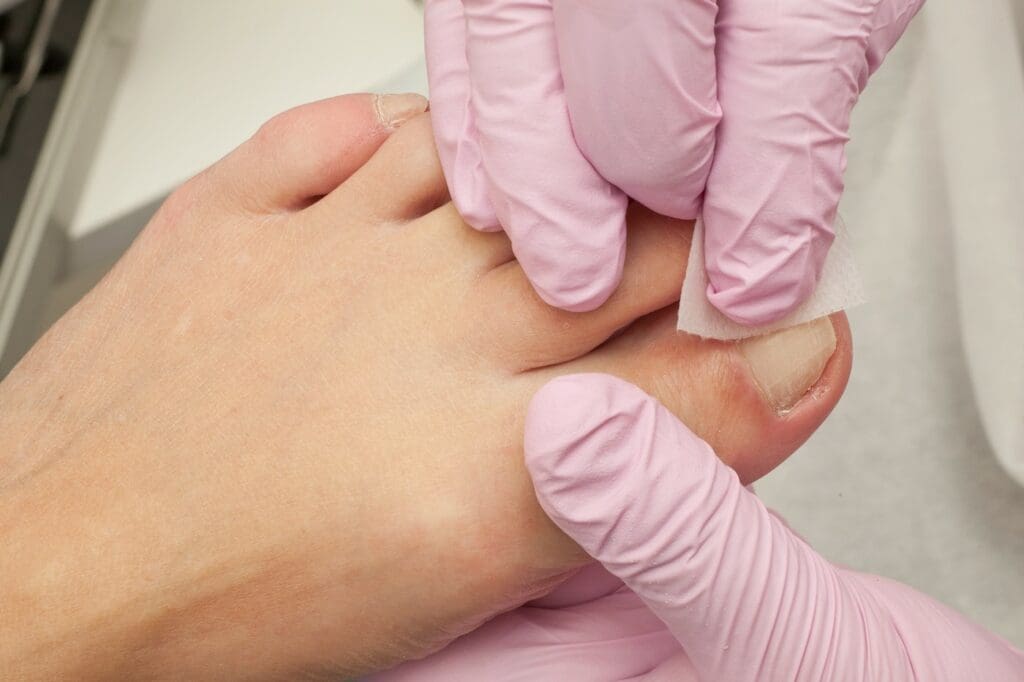
Ingrown toenails cause pain and inflammation along the edge of the toenail, usually the big toe. Ingrown toenails are common and most often affect young adults. Factors that can cause ingrown toenails to develop include cutting toenails too short or in a curve (rather than straight across), and wearing pointed-toe and high-heeled shoes.
Arthritis, including gout
Many common forms of arthritis, including osteoarthritis, gout and rheumatoid arthritis, can affect the feet and cause foot pain. One of the most common symptoms of gout is severe pain, redness, and swelling at the base of the big toe.
Plantar fasciitis and heel spurs

Pain along the sole of the foot can be caused by plantar fasciitis. The plantar fascia is a strong band of tissue that stretches across the sole of the foot and is attached to the heel bone.
With repeated activity on our feet, the plantar fascia can become tight and cause persistent traction (tugging) on its attachment point into the heel bone, resulting in inflammation and pain. Sometimes a ‘spur’ develops at the site of this traction on the bone and protrudes into the surrounding tissue. This is known as a heel spur.
Sprains and strains
Sprains and strains of the muscles and ligaments in your feet, such as an ankle sprain, often occur with overuse or after doing more physical activity than you are used to.
Symptoms of sprains and strains include pain, swelling, bruising and loss of movement.
Stress fractures
A stress fracture – a small crack in one of the bones of the feet – usually occurs in people doing a lot of high-impact sports. There may be tenderness and bruising of the skin as well as pain in the foot with these injuries.
Metatarsalgia
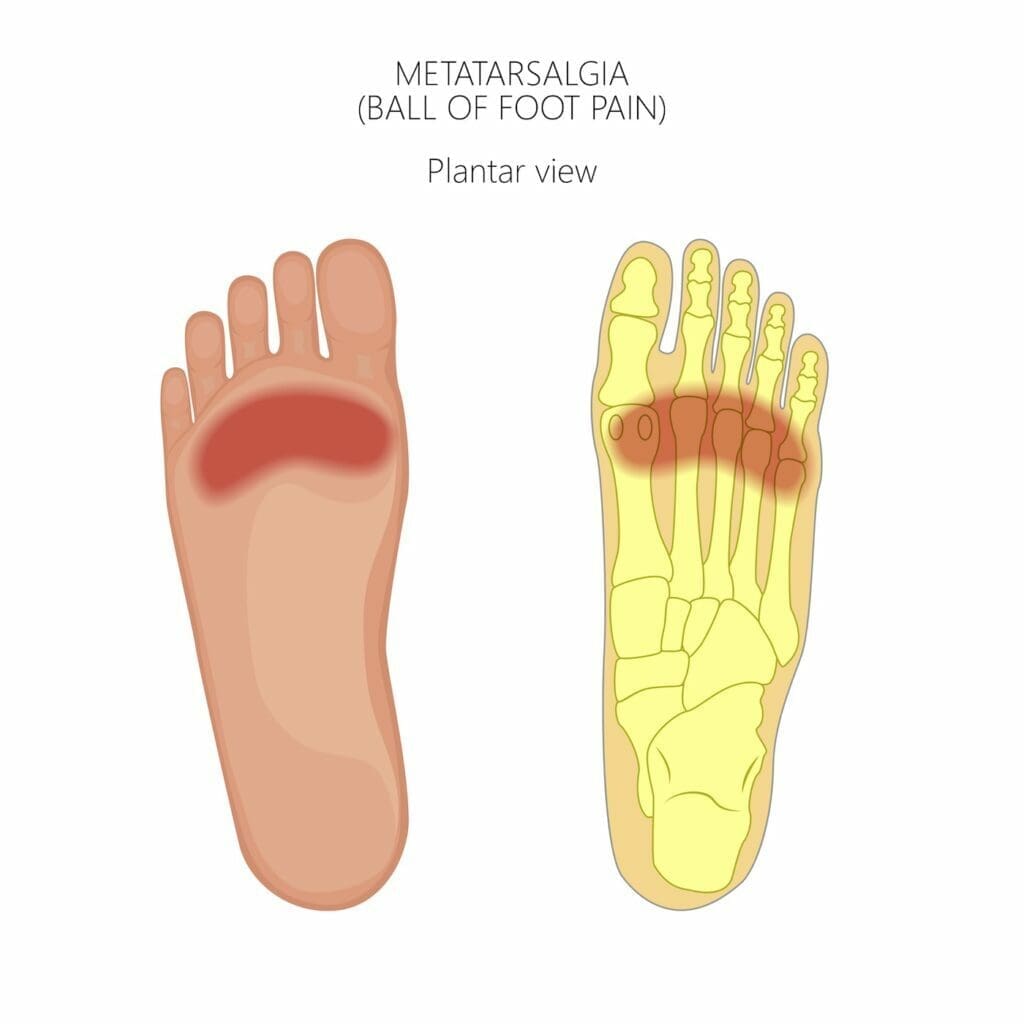
Metatarsalgia describes a painful condition that affects the metatarsals – a group of 5 bones in the midfoot.
Symptoms include pain and inflammation in the ball of the foot – the area between the toes and the arch of the foot. There may be a burning sensation or tingling and numbness in the ball of the foot or the toes. You may feel like there is a pebble or something in your sock or shoe.
Morton’s neuroma
Morton’s neuroma is a condition affecting the ball of your foot, involving thickening of tissue around one of the nerves leading to your toes. The symptoms include a feeling of there being a pebble or lump in your shoe under your foot, tingling, burning or numbness. While other nerves in the foot may have a neuroma, the most common neuroma is Morton’s neuroma, which occurs between the third and fourth toes.
The compression and irritation of the nerve can eventually lead to permanent nerve damage.
Posterior tibial tendonitis

The posterior tibial tendon provides support and stability to the arch of the foot when we walk. If the tendon is inflamed or torn, it may not be able to support the arch. Over time the arch will drop, resulting in what’s known as flatfoot. This condition is the most common cause of acquired flatfoot in adults.
Symptoms of posterior tibial tendonitis include pain along the inside of the foot or ankle, along the course of the tendon, inward rolling of the ankle, and redness, warmth and swelling of the area. As it progresses, the pain may shift to the outside of the foot.
Other causes of foot pain include:
Flat feet (fallen arches)
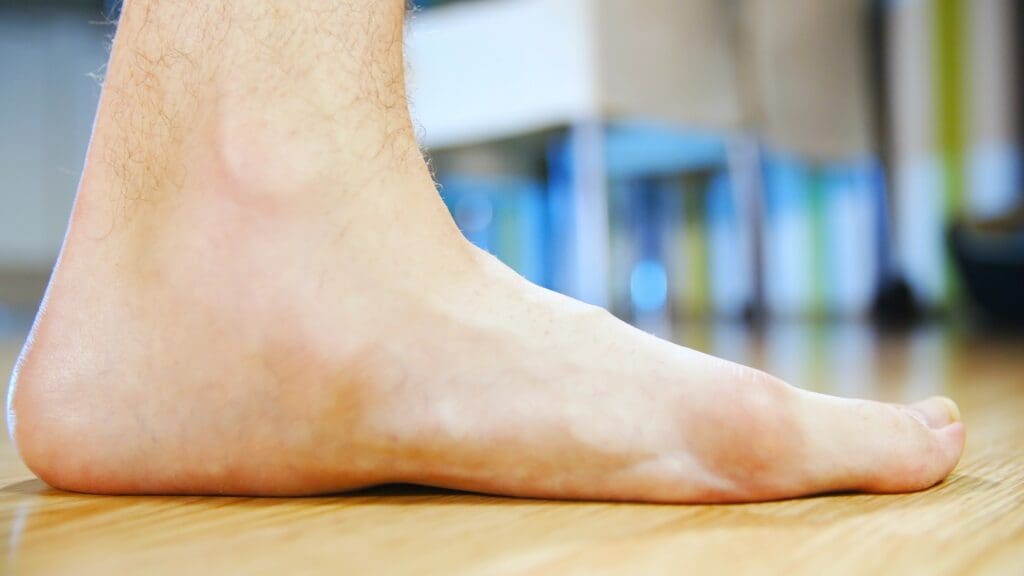
If the tendons that normally work together to support the arch of your foot become damaged or stretched, the arch may start to sag and eventually appear flattened. Colloquially, this is known as fallen arches. Fallen arches and flatfoot can be caused by arthritis, torn ligaments and posterior tibial tendon injury.
Symptoms of flatfoot include pain that is worse on activity, pain along the posterior tibial tendon, pain on the outside of the ankles, bony spurs on the top of the foot,
Tarsal tunnel syndrome
Tarsal tunnel syndrome is a condition caused by compression of the posterior tibial nerve as it runs through a canal called the tarsal tunnel at the level of the ankle.
The symptoms of tarsal tunnel syndrome are tingling, pins and needles, shooting pains, numbness or burning along the inside of the ankle or foot. Tarsal tunnel syndrome is similar to carpal tunnel syndrome, which occurs in the wrist.
Peripheral arterial disease
Peripheral arterial disease is a condition affecting the circulation outside of the heart and brain, such as in the legs and feet.
Narrowing of the arteries caused by fatty deposits called plaque limits the amount of blood reaching the legs. This starves the muscles of oxygen, leading to symptoms called intermittent claudication. These include cramps, pain, aching or numbness in the legs when walking, with the pain going away at rest. If the blockages in the arteries are severe, the pain may happen at rest, and there may be pain in the feet.
Diabetic neuropathy
Diabetic neuropathy is a complication of diabetes and is caused by high blood sugar damaging the nerves. It occurs most often in the nerves of the legs and feet.
Symptoms include tingling or numbness in the feet. There may be burning sensations or sharp pain. The condition is progressive, so the symptoms will get worse over time and may continue up the legs. A person with diabetic neuropathy may not be able to feel heat, cold or injury to their feet. A person with diabetes must have regular check-ups of their feet.
Blisters
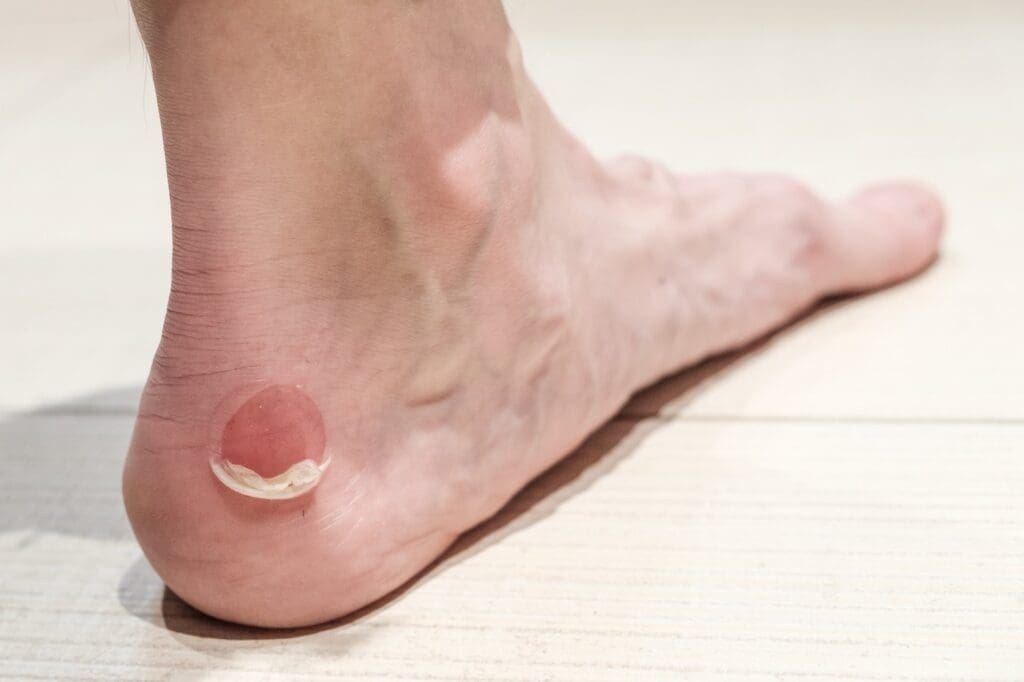
Blisters are tender, fluid-filled sores on the skin. Blisters on the feet are usually the result of friction from ill-fitting footwear.
Athlete’s foot
Athlete’s foot – also called tinea pedis – is a common fungal infection of the toes and feet. Symptoms include scaling and peeling skin (particularly between the toes), small blisters on the feet, itching, stinging and burning.
Fungal nail infections
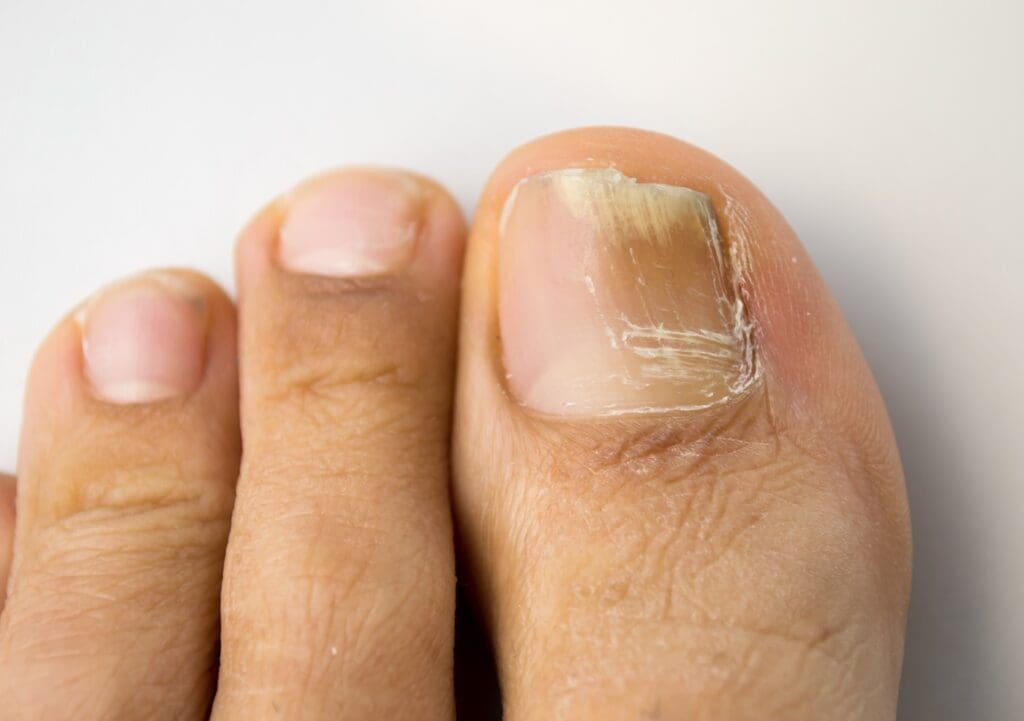
Fungal nail infections are also called onychomycosis. Changes in affected nails can include:
- thickening and roughness
- nail discoloration (nails may turn white, yellow or brown)
- brittle, crumbling nail edges, and
- pain and tenderness if left untreated.
Plantar warts
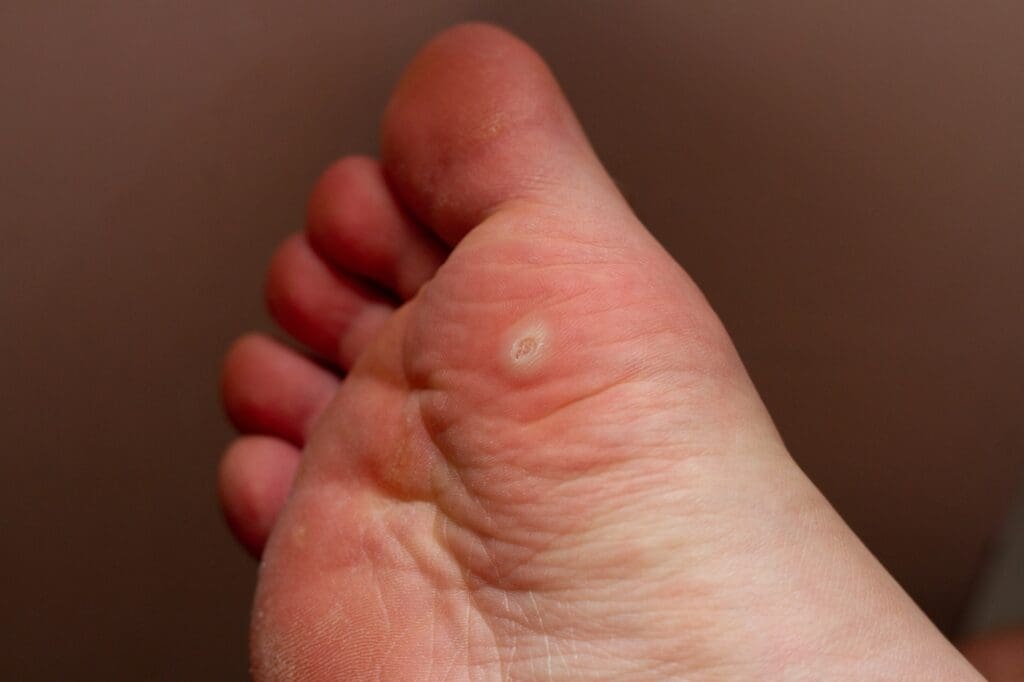
Plantar warts are small, bumpy growths that appear on the soles of the feet, caused by infection with certain strains of the human papillomavirus (HPV). They sometimes have small black dots on the surface and can be painful when walking or standing.
Who should you see about foot pain?
Your GP is a good starting point if you have symptoms of foot pain. Other healthcare professionals who may be involved in the diagnosis and treatment of foot pain in Australia are podiatrists, physiotherapists and sports physicians.
Podiatrists are healthcare professionals who specialise in problems with the feet and foot health. In Australia, podiatrists must have a Bachelor of Podiatry and be registered to practise.
Diagnosis of foot pain
To diagnose the cause of foot pain, your feet will be examined closely, including the nails and the soles. The doctor or other healthcare professional will want to know when and how the symptoms started. You may be asked to perform some simple movements.
Sometimes imaging is helpful in diagnosis, including X-rays, CT scans, MRI scans, ultrasound or bone scans. CT scans show soft tissues better than a plain X-ray and are useful to show ligaments and muscles. Ultrasound is non-invasive and is good for showing ligaments and tendons (including the Achilles tendon), nerves, and the plantar fascia.
Bone scans use radioactive tracers injected into a vein and can show differences in bone metabolism (called hot spots). This makes them good at showing stress fractures as well as other fractures. MRI of the foot and ankle can be used to show tendons, ligaments and cartilage.

