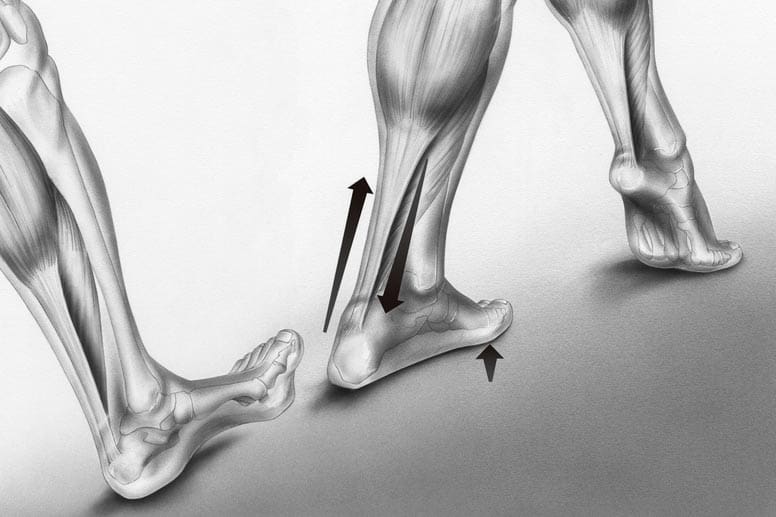
What is Achilles tendinitis?
Achilles tendinitis, also known as Achilles tendonitis, is inflammation of the Achilles tendon. The Achilles tendon connects your calf muscles to the back of your heel bone. It allows extension of your foot downward, away from your body, which lets your heel lift off the ground as you move forward when walking. Every time you take a step you rely on your Achilles tendon.
What causes Achilles tendinitis?
Achilles tendinitis can be caused by:
- overly tight calf muscles;
- excessive running up hill or down hill;
- a sudden increase in the amount of exercise, e.g. running for a longer distance;
- wearing ill-fitting running shoes, such as those with soles that are too stiff; or
- wearing high heels regularly, or changing between high heels all day and flat shoes or low running shoes in the evening.

Overuse is common in walkers, runners, dancers and other athletes who do a lot of jumping and sudden starts/stops, which exert a lot of stress on the Achilles tendon.
Continuing to stress an inflamed Achilles tendon can cause rupture of the tendon – it snaps, often with a distinctive popping sound. A ruptured Achilles tendon makes it virtually impossible to walk. An Achilles tendon rupture is usually treated by surgical repair or wearing a cast.
Symptoms of Achilles tendinitis
- Pain anywhere along the tendon, but most often on or close to the heel.
- Swelling of the skin over the tendon, associated with warmth, redness and tenderness.
- Pain on rising up on the toes and pain with pushing off on the toes. If you are unable to stand on your toes you may have ruptured the tendon. This requires urgent medical attention.
- A painful heel for the first few minutes of walking after waking up in the morning.
- Stiffness of the ankle, which often improves with mild activity.
What you can do in the first 48 hours of an Achilles injury
- Rest the affected foot and avoid weight-bearing activities.
- Use ice packs to help ease the swelling, pain and redness.
- Compress the affected foot and ankle with an elastic compression bandage.
- Elevate the affected foot as much as possible while the inflammation settles.
If you cannot walk properly and think you may have ruptured the tendon, see a doctor straight away. Similarly, if you have a sudden feeling like you have been kicked in the back of the leg, seek medical advice.
Rehabilitation for Achilles tendinitis
See your doctor or sports physiotherapist for further advice. You may be prescribed anti-inflammatory medicine and a rehabilitation programme. Sometimes, the ankle may be put into a walking boot or cast to immobilise the ankle in the short term.
- Gentle calf stretching is the first stage of rehabilitation. Don’t stretch to the point of pain.
- Strengthening the Achilles tendon is the second stage. Your doctor or sports physiotherapist will be able to advise you on exercises for this.
- Special exercises called eccentric calf raises, that contract the calf muscle as it is lengthening (during the lowering part of the movement), are the standard exercise used in the rehabilitation of Achilles tendon injuries.
- Sometimes a heel raise or orthotics may be useful.
- As symptoms resolve, resume normal weight-bearing activities gradually.
- Avoid running until all tenderness has gone. Swimming or cycling in low gear are good replacement activities.
Preventing Achilles tendinitis
- Do strengthening and stretching exercises to keep calf muscles strong and flexible.
- Keep your hamstring muscles flexible by stretching.
- Warm up and stretch adequately before participating in any sports.
- Always increase the intensity and duration of training gradually.
- Do not continue an exercise if you experience pain over the tendon.
- Wear properly fitted running and other sports shoes, including properly fitted arch supports if your feet roll inwards excessively (over-pronate).
When to see a doctor
Consult a doctor if you feel pain over your heels, or the back of your legs, that worsens with exercise.