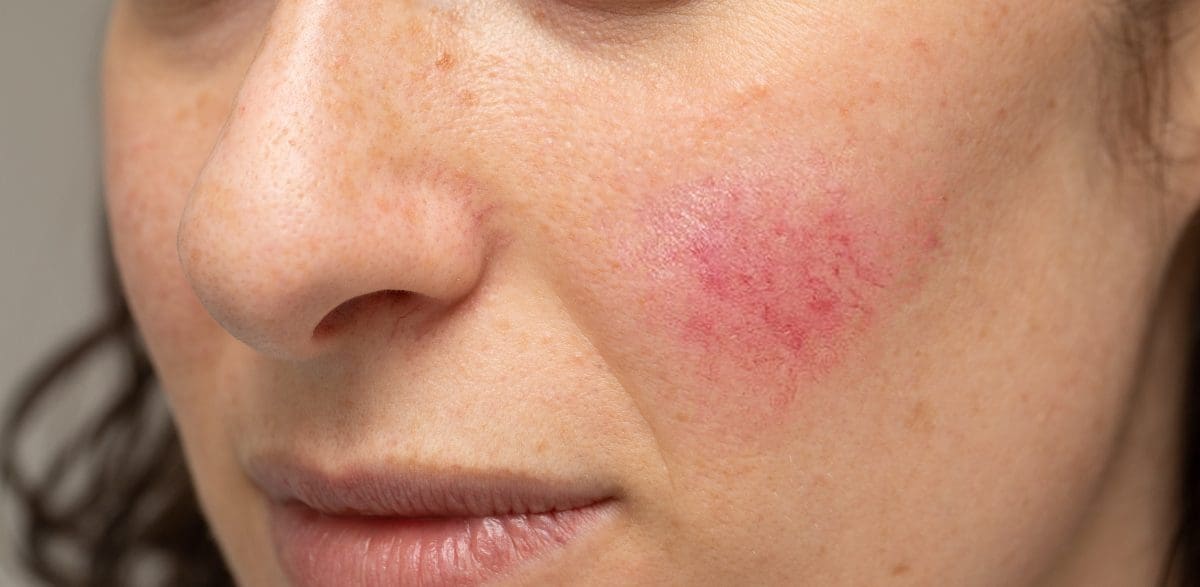
Rosacea (pronounced rose-ay-sha) is a common skin condition which causes the face to become red and inflamed, with enlarged and broken blood vessels and often with spots or bumps which look similar to acne.
Symptoms
The symptoms of rosacea may come and go, with the severity of skin redness and inflammation of the face changing over time. The symptoms of rosacea can include:
- A red, flushed face, particularly on the cheeks, nose, forehead and chin;
- Small red spots and bumps (papules) that may be filled with pus (pustules);
- Visible small blood vessels on the face, particularly the cheeks and the nose;
- Frequent blushing or flushing;
- A stinging or burning feeling on the face, or the face feels hot;
- Sensitive skin that is dry and flaky and easily irritated by skincare products, sunscreen or strong sunlight;
- Dry, red, itchy or burning eyes and inflamed eyelids, often with a feeling that there is grit stuck in the eye; and
- A red, swollen nose with thickened skin that looks like orange peel.
The progression of rosacea
The first sign of rosacea is usually blushing, with the face becoming flushed and red, particularly on the cheeks, nose and chin. The flushing is due to blood vessels in the skin becoming enlarged and more visible.
Over time, blushing may become more frequent and result in the face becoming constantly red. With repeated episodes of blushing, the small blood vessels in the skin (capillaries) may burst, which worsens the redness. The skin may become inflamed and break out in red spots (papules) or pus-filled bumps (pustules) that look like acne. In fact, the condition used to be called ‘acne rosacea’ for this reason. But it is now known that rosacea is not a form of acne.
Causes
Rosacea is a complex condition and the exact cause is not yet known. Rather than being due to just a single cause, a combination of factors is likely to be involved. This can include your genes and environment, plus factors related to your immune system, skin and blood vessels.
A microscopic mite that normally lives harmlessly in the hair follicles (such as the eyelashes) may also play a role in causing the spots (papules) of rosacea, but its exact role is not yet clear.
Rosacea is not caused by alcohol consumption, although alcohol does make rosacea worse.
Rosacea is not contagious, so it can’t be spread from person to person.
Risk factors and triggers
Rosacea is more common in fair-skinned people with blue eyes who have an English or Celtic background, particularly if there is a family history of rosacea. Rosacea usually affects people between the ages of 30 to 60, with women more often affected than men.
Any factor that leads to the blood vessels in the skin becoming dilated (swollen) can trigger rosacea or make the condition worse. Known trigger factors include:
- Alcohol;
- Spicy foods;
- Hot foods and drinks;
- Being stressed, embarrassed or angry;
- Strong sunlight;
- Extremes of temperature (including hot baths/showers or heated pools/ saunas);
- Certain drugs that cause blood vessels to expand (dilate), such as some blood pressure medicines;
- Reactions to some skincare products;
- Strenuous exercise; and
- Corticosteroid medicines (either applied to the skin or taken as tablets).
Complications
People with long-term severe rosacea (usually men) sometimes develop a distinctive, red swollen or bulbous nose, with enlarged pores. This is due to swelling of the blood vessels and glands in the nose, along with changes in the structure of the skin due to the chronically swollen spots (papules and pustules) of rosacea.
Untreated rosacea of the eyes can damage your vision, so speak to your doctor or an eye specialist (ophthalmologist) if you have symptoms affecting your eyes.
Diagnosis
Rosacea can usually be diagnosed without needing any tests. Your GP (general practitioner) or a skin specialist (dermatologist) should be able to make a diagnosis by examining the skin on your face. Rarely, a skin biopsy or blood test might be necessary to rule out other causes of redness of the face.
Rosacea treatments
There is currently no cure for rosacea. Although the condition tends to worsen over time, there are a number of ways to manage symptoms. The right treatment for you will depend on the severity of your rosacea.
Self-care for rosacea
There are a few things you can do to help improve your symptoms.
- Avoid trigger factors (see above).
- Sooth sensitive skin. Use gentle soap-free cleansers and oil-free skincare products.
- Protect your skin from sunlight. Wear low-irritant/oil-free sunscreen and a hat.
- Put an ice block in your mouth between your gums and cheek – some people find that this can temporarily reduce facial redness.
Medicines
Lotions, gels or creams may be prescribed by your doctor or specialist, with or without medicines that you take as tablets.
Treatments applied to the skin may include:
- Metronidazole cream or gel (e.g. Rozex)
- Azelaic acid (e.g. Azclear lotion)
- Antibiotic creams or gels (e.g. erythromycin or clindamycin)
- Brimonidine gel (e.g. Mirvaso gel)
- Ivermectin cream (e.g. Soolantra cream)
Corticosteroid creams should be avoided as they may make rosacea worse.
Treatments taken as tablets may include antibiotics and isotretinoin.
- Antibiotic tablets can reduce skin inflammation and redness, with the duration of treatment depending on the severity of rosacea (a course of 8-12 weeks is generally required). Doxycycline, erythromycin and minocycline are some of the commonly used antibiotics. Antibiotic tablets are usually combined with treatments applied to the skin.
- Isotretinoin tablets may be useful if a course of antibiotics has not helped. However, this medicine can potentially have serious side effects so speak to your doctor about whether it is a suitable option for you.
- Some heart medicines can help reduce facial flushing, including alpha-2 receptor agonists (e.g. clonidine) or beta-blockers (e.g. carvedilol).
Laser therapy and other procedures
Your doctor may recommend laser therapy or cosmetic surgery to treat your rosacea.
Laser therapy can help reduce swollen blood vessels, but multiple treatments are required. Also, the redness will eventually come back and need further treatment. IPL (intense pulsed light) therapy can also be used, but it is generally not as effective as laser therapy.
Cosmetic surgery may be needed to treat a swollen or bulbous nose (rhinophyma).
The outlook for rosacea
As there is no cure, rosacea needs to be managed over a long time. Rosacea varies greatly from person to person – some people will have constant symptoms, whereas others will have times when the symptoms go away for a while. Similarly, rosacea can be stable in some people, whereas others may experience slow worsening of the condition over time.
As with many conditions, early treatment can improve the outlook. So If you have a red flushed face, ask your doctor whether it could be rosacea.