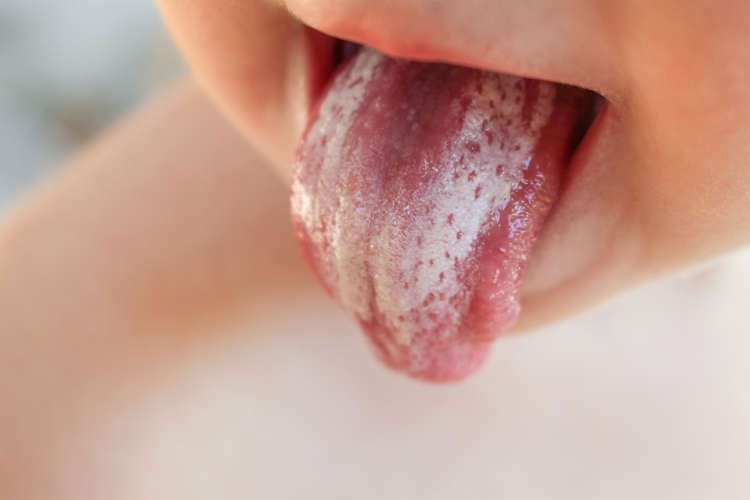
Oral thrush is an infection caused by the yeast-like fungus Candida albicans, or sometimes by other types of Candida, that affects the mouth.
Candida thrives in warm, moist places and can affect the skin, or mucous membranes such as the vagina or mouth, causing the infection commonly known as thrush.
Some types of Candida occur naturally in the body, but they don’t normally cause disease in healthy people. They are known as opportunistic pathogens – they take advantage when the normal environment of the body is upset, such as by taking antibiotics, to multiply abnormally. This results in so-called ‘overgrowth’ of Candida and the appearance of symptoms which may need treatment.
Symptoms
The most common symptom of oral thrush is:
- creamy, white patches on the inside of the mouth and tongue.
Other oral thrush symptoms include:
- mouth pain;
- redness or bleeding if the mouth lesions are scratched or rubbed off; and
- cracks and redness at the corners of the mouth (especially in those who wear dentures).
Babies with oral thrush may refuse feeds, have difficulty feeding and be irritable. They may also have poor weight gain and nappy rash.
Risk factors
The following groups of people have an increased risk of developing oral thrush.
- People who regularly use inhaled corticosteroids (e.g. people being treated for asthma).
- Those who wear dentures, as injury from an ill-fitting denture can provide a breeding ground for the growth of Candida. Also, constant moisture at the corners of the mouth, caused by badly fitting dentures, will allow Candida to grow.
- People with conditions or taking medicines that have an effect on saliva and so interfere with the normal protective mechanisms of the mouth.
- People with poor oral hygiene.
- People who smoke.
- People with conditions such as diabetes, iron deficiency, HIV infection, and cancer.
- People taking certain medicines such as corticosteroids and cancer treatments (which can suppress the immune system) and broad-spectrum antibiotics (which may interfere with normal protective bacteria).
Babies can be susceptible to oral thrush because their immune systems are still developing. The most common age to be affected is 4 weeks or younger. Babies can catch the Candida infection either from their mothers during birth, or soon after from contact with people.
Diagnosis and tests
Doctors can usually diagnose oral thrush by examining the mouth. Sometimes samples from the white lesions are taken to confirm the diagnosis. The samples are examined under the microscope, and sometimes cultured to confirm infection with Candida fungus.
Treatment of oral thrush
Antifungal medicines such as amphotericin, miconazole and nystatin are used to treat oral thrush. Antifungals are available as lozenges, gel, capsules, oral drops and liquid.
Oral thrush in babies often resolves with no treatment after a few days. However, if thrush is persisting, antifungal medicine (gel or oral drops) may be recommended. Breastfeeding mothers of babies with oral thrush may also need treatment with antifungal medicines to prevent the infection being passed back and forth from mother to baby.
It is important for those with underlying medical conditions to get treatment advice from their specialist doctor.
Prevention of oral thrush
The following self-help tips can help prevent oral thrush.
- If you use inhaled corticosteroids, try using a spacer with your inhaler and rinse your mouth thoroughly with water after each inhalation.
- For those who wear dentures, remove dentures at night, clean them and leave them out to dry.
- Effective oral hygiene is important – brush at least twice a day and floss at least once, and see your dentist regularly.
- Eat a healthy balanced diet and cut down on foods that contain sugar and yeast, as these foods can increase your chance of developing oral thrush.
- Smoking can encourage the growth of yeast in your mouth, so if you are a smoker, quit smoking.