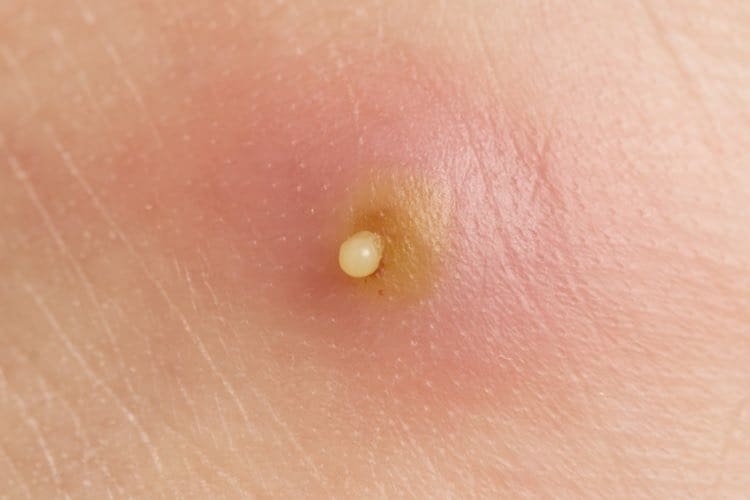
What are boils?
Boils are inflamed, pus-filled areas under the skin that look like oversized pimples. They develop when a hair follicle becomes infected and forms an abscess in the skin and underlying tissue. The medical name for a boil is a furuncle, while a boil with multiple heads is called a carbuncle.
Boils can be treated with simple self-help measures such as a hot compress, but sometimes they need to be drained and treated with antibiotics.
Symptoms
A boil generally starts as a red, tender lump on the skin that becomes firm and hard over time. Eventually, the centre of the boil softens and becomes filled with pus that finally ‘forms a head’ and drains out through the skin.
Boils are painful and can develop anywhere on the body, but often in areas like the armpits, buttocks, groin, thighs, face and neck.
Sometimes boils are associated with fevers and chills.
Complications
Fevers associated with boils can occasionally be a sign of bacteraemia or septicaemia (infection that has spread to the bloodstream) – a serious complication.
Cellulitis (spreading infection of the skin) is another possible complication.
What causes boils?
Boils are usually caused by Staphylococcus aureus bacteria infecting one or more hair follicles on the skin. Sometimes another type of bacteria – Streptococcus pyogenes (group A strep) – accompanies the Staph aureus bacteria.
The bacteria may enter your skin via a cut or any break in the skin, including tiny grazes.
Risk factors
Boils can affect anyone, but there are some people who are more prone to getting them. Your risk of boils may be increased if you have:
- diabetes that is not well controlled;
- eczema;
- acne; or
- have problems with your immune system.
Being a smoker also increases your risk of developing skin infections.
Sometimes adolescents go through a phase of experiencing boils.
Other types of skin abscesses
There are several other skin problems that can have similar symptoms to boils.
- Cystic acne is where pus-filled lumps form beneath the skin’s surface when clogged oil ducts in the skin become inflamed.
- Hidradenitis suppurativa is a condition where multiple cysts or abscesses form under the armpits and/or in the groin area due to inflammation of the sweat glands.
- Pilonidal cyst is a specific type of abscess that develops in the crease of the buttocks, often resulting from an infected ingrown hair. Pilonidal cysts are more common in people who sit for long periods, for example those who drive long distances for a living. This type of abscess usually needs to be drained or treated surgically.
Diagnosis and tests
If you have a painful, red lump on your skin that you are worried about, see your GP (general practitioner). It’s especially important to see your doctor if you develop a fever, if you have a boil on your face, or if you have a boil that is large or getting worse.
Your doctor will ask about your symptoms and how long you’ve had them. They will also want to know whether you have had boils before. They will usually be able to diagnose a boil by examining the affected area.
If your doctor lances and drains your boil (see below) they may send samples to a laboratory to confirm the type of bacterial infection and which antibiotics would best treat it.
How is a boil treated?
Self-care for boils involves applying a hot compress to the affected area. This will help the boil to form a head and then rupture and drain, which will give considerable pain relief. Painkillers such as paracetamol or ibuprofen can also be taken to relieve the pain.
DO NOT burst a boil yourself (by pricking or squeezing it), as the infection may spread. Let it rupture on its own.
After the boil has burst, wash the area thoroughly with soap and water, or an antiseptic solution, and cover it with a dry dressing. Repeat the procedure daily until the area is completely healed. Shower instead of bathing while you have a boil or healing boil, as this decreases the chances of spreading the infection.
Larger boils may need to be lanced and drained by your doctor. This is a minor procedure that can be done in your doctor’s surgery (rooms). Your doctor may also prescribe antibiotics, but antibiotics are not always needed. They are most often prescribed for large boils or if you have other symptoms (such as fever) or redness of the surrounding skin that indicate the infection may be spreading.
If a boil comes back or is not healing you may need a different antibiotic or a longer course of antibiotics.
Treatment of recurrent boils
If you have (or your child has) recurrent boils, further testing and treatment may be needed to help stop the boils coming back.
Swabs may be taken from your nose and skin to see if you are carrying Staphylococcal bacteria. (About per 20-30 per cent of healthy people carry Staph aureus on their skin or in their nose.)
If you are a carrier, an antibiotic ointment to be applied inside your nostrils may be recommended. In addition, you and your household contacts may need to wash all over with antiseptic wash for 5 days.
Stopping the spread of infection
To stop the spread of infection when you have a boil, it helps to follow some simple measures.
- Keep the boil covered with a clean dressing until it is completely healed.
- Wash your hands (or any other part of your body) with soap and water after contact with a boil (especially an oozing boil).
- Wash your towel in hot water after each use and wash bed sheets in hot water at least once a week. Hang the washing in the sun to dry.
Preventing boils
To help prevent boils, regularly wash your skin with soap and water. Don’t share personal items, such as towels, soap or razors with other people in your household. And always cover any wounds you have with clean dressings.