What is syphilis?
Syphilis is a sexually transmissible infection (STI). You can get syphilis if you have unprotected sex with an infected person. Syphilis is caused by the bacterium Treponema pallidum and can be cured with antibiotics. Syphilis is passed from person to person when the skin or mucous membranes have contact with the sores on a person with syphilis. It is highly contagious. Both men and women can be infected.
There are 3 stages of syphilis which each have different symptoms. The most common symptom is a painless ulcer (a breakdown of skin) in the genital or anal area. However, syphilis can be present in your blood without symptoms or may take weeks for any symptoms to become apparent.
Primary syphilis symptoms
During the first stage of syphilis, known as primary syphilis, there are 2 common symptoms:
- a painless ulcer (usually in the genital region) known as a “syphilis sore” or chancre – this is highly contagious. The ulcer may also occur at the back of the throat, in the mouth, inside the vagina or in the anal region. It is harder to spot in these locations
- Swollen lymph nodes (or glands), usually in the groin region on both sides
The chancre often occurs 2-3 weeks after getting syphilis from someone but can be delayed up to around 3 months. Mostly there is a single sore, but there can be multiple ulcers. It may be painful in some people. Even without treatment, this sore generally heals itself within a month, which can make it easy to miss. This does not mean you are cured. Although these symptoms may settle, syphilis is spreading throughout your body (systemic spread).
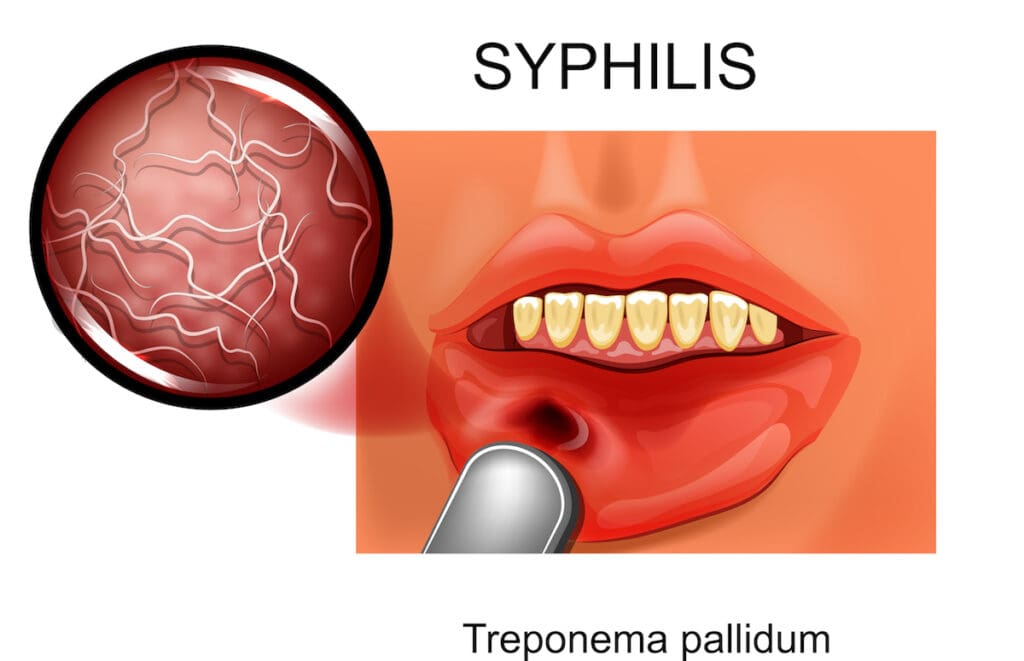
What does a syphilis sore (chancre) look like?
When this ulcer first appears, it will look like a small pimple or area of swelling. The skin then breaks down and becomes a raised open sore. This is when Treponema pallidum enters through your skin into your body.
Secondary syphilis symptoms
If syphilis remains undetected and untreated, it will progress to the second stage – secondary syphilis. This is usually seen within weeks or months after primary syphilis. Secondary syphilis affects many organs, leading to many different symptoms, which include:
- Skin rash. This highly contagious red rash may cover most of your chest, arms, and legs. It will also include the palms of the hands and soles of the feet. The spots are often red or coppery in colour. The rash can also be seen in the mouth and genital or anal areas. Due to the different skin and environments in these areas, the rash here looks like large, raised grey patches.
- Swollen lymph nodes.
- Hair loss, especially of the eyebrows and on the head.
- Flu-like illness (fever, headache, tiredness), potentially including aches and pains in your joints.
- Hepatitis (liver inflammation).
The symptoms of secondary syphilis will disappear, whether you are treated or not. But if you are not treated the disease will progress to the latent stage, where it is essentially ‘hidden’ and there are no symptoms. However, you will still be infected. The disease may remain dormant for life, or may develop into tertiary syphilis.
Tertiary syphilis symptoms
The third stage (tertiary syphilis) is much less common in Australia. However, the consequences of this stage are devastating and can cause death. These include infection of the brain, heart, eyes and skin. Tertiary syphilis symptoms may not appear until up to 30 years after first catching the disease.
How is syphilis spread?
Syphilis is spread by skin or mucous membrane contact with the sores during unprotected sexual activity with someone who is in the first 2 stages of syphilis. Syphilis can be spread by vaginal, anal or oral sex. Treponema pallidum (the bacterium that causes syphilis) enters small breaks in the skin of the mouth, genitals, and anus. This is known as acquired syphilis.
Syphilis can also be spread from mother to baby either during pregnancy or birth, which is termed congenital syphilis. Syphilis causes many serious problems for the baby, both as it grows in the womb and after birth. There is a much higher risk of miscarriage and stillbirth than in normal pregnancies.
Congenital syphilis may not cause any symptoms, but the baby should be treated as it may develop serious health problems later.
Risk factors
If you fall into any of these groups, you may be at increased risk of getting syphilis:
- Men who have sex with men
- People already diagnosed with HIV
- Aboriginal and Torres Strait Islander people
- Pregnant women
- People with multiple sexual partners
- People having sexual activity with a person with syphilis
It is recommended you talk to your doctor about getting tested or ‘screened’, even if you haven’t noticed any suspicious symptoms in yourself. Screening tests are done to detect diseases in people who do not have any symptoms.
Pregnant women in Australia are always offered screening for syphilis (amongst other infections) as part of their normal care. These screening tests are important as the earlier this potentially ‘silent’ infection is found, the better it can be treated.
Complications
If it remains untreated, syphilis can lead to serious complications, including death. It can also increase your risk of catching and spreading other serious STIs such as human immunodeficiency virus (HIV). As mentioned, having syphilis raises a woman’s risk of a miscarriage or stillbirth, and can cause serious health problems for a baby.
Diagnosis of syphilis
You can visit your GP or a sexual health clinic to be tested for syphilis and for regular sexual health check-ups.
Syphilis is diagnosed using a combination of blood tests, a swab of any ulcers, and information gained by your doctor asking specific questions and examining you.
There are a variety of tests used to diagnose syphilis. Some of these may take up to 3 weeks to produce results. If your doctor is concerned that you are likely to have syphilis, they may recommend that you start antibiotics in the meantime. The doctor may also test for other STIs at the same time.
| Tests used to diagnose syphilis | |
|---|---|
| Test/Investigation | Purpose |
| Blood test | Detects antibodies to Treponema pallidum |
| A swab of an ulcer | Can detect DNA of Treponema pallidum bacteria; May be able to view the Treponema pallidum bacteria under microscope |
How quickly can syphilis be detected after infection?
Syphilis can be detected on tests as early as 1-2 weeks after you’ve been exposed. A swab can detect syphilis earlier than a blood test can detect syphilis antibodies. If you think you could have syphilis or any other STI, it is important to see your doctor as soon as possible to be tested and get the right treatment. Once treatment is finished, it will also prevent the spread of syphilis to other people you have sexual contact with.
Treatment
The treatment for syphilis in Australia is the antibiotic penicillin, which will cure the infection. If you are allergic to penicillin, you should alert your doctor so that they can look at the alternatives.
If you are in one of the first 2 stages of syphilis, the antibiotic will be given as an intramuscular (into the muscle) injection into your shoulder or thigh. It can be given as a single injection, or you may need to have an injection every day for 10 days.
Treatment of tertiary syphilis is given intravenously (into a vein) for a couple of weeks. Other treatments may also be needed to ease complications caused by the disease in this stage.
You will need to be closely monitored after finishing treatment to make sure the penicillin has worked. A ‘test of cure’ (TOC) is performed at 3, 6 and 12 months after completing the antibiotic treatment.
Even if you have been treated for syphilis previously, it does not protect you from being infected with syphilis again.
Public health and syphilis
Aside from treating and protecting yourself, it is important to consider other people you have had or are currently having sexual contact with. Because of this:
- Your doctor will strongly recommend no sexual activity during treatment and for 7 further days after treatment is finished. If you have sex during treatment, you could be infected again, or infect someone else
- Your sexual partners (both regular and casual) from the last few months must be contacted and also checked by a doctor. This process is known as “contact tracing.” Some may need treatment with antibiotics themselves
- Your doctor and the pathology lab are required to notify the state or territory health department as syphilis is a notifiable disease. This is important as it allows tracking of how many people get syphilis and can give early warnings about high numbers in an area (outbreak).
Your doctor may suggest testing for other STIs, either at the start of your treatment or when you come back for further testing at around 3 months.
Support
As well as providing diagnosis, medical advice and treatment, your GP or local sexual health clinic can also direct you to patient information resources for syphilis that you can look through at your own pace. Otherwise, you may find syphilis or STI support groups helpful to talk with other people in a similar situation. Your GP or sexual health clinic can help direct you to these groups in your area.
Outlook
Antibiotics can cure syphilis at all stages of the disease. If it is treated in the early stages, damage to your organs can be avoided. If it is left untreated beyond the early stages, it can do serious damage to your organs and be life-threatening. Even if it is cured at a later stage, the damage to your organs can’t be repaired.
If a baby is infected with syphilis while it is in the womb, there is an increased risk of miscarriage or stillbirth. Babies born with syphilis may have deformities and other health problems and also may die shortly after birth.
Prevention
There is no vaccine for syphilis, so safe sex is the best way to protect yourself. The use of barrier protection is important in all sexual activities, including vaginal, anal or oral sex. Condoms and dental dams act as a physical barrier between you and your partner, which reduces the chance of getting or spreading STIs like syphilis.
- Male condom. This can be used to prevent the spread of syphilis in all types of sexual activity, including oral sex.
- Female condom. A soft pouch of material similar to a male condom with two flexible rings at each end. It is inserted into the vagina or anus before sex. Female condoms can reduce the risk of catching syphilis, though they are not as reliable barriers as the male condom.
- Dental dam. This is a square patch of thin latex used to prevent transmission of STIs during contact between the mouth and the vagina or the mouth and the anus.
As well as practising safe sex, regular STI check-ups will help to ensure you remain free from STIs. They are easy to do, confidential and usually free.
Avoid sex with someone who has a sore on their genitals.
