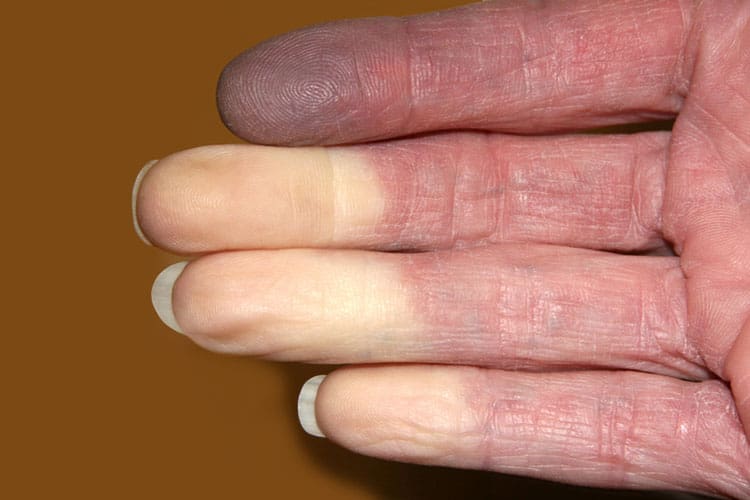
Raynaud’s disease is a common condition which causes a temporary spasm (narrowing) of the arteries leading to their fingers and toes, which means the tissues in these areas temporarily do not get enough blood and hence enough oxygen.
Symptoms of Raynaud’s phenomenon
Initially the affected fingers or toes appear white and may feel numb or cold, then turn blue. The colour can have a patchy appearance. As the blood returns they turn red and may feel painful with tingling, a feeling of ‘pins and needles’ or burning. The colour sequence is not the same for everyone with Raynaud’s disease.
These symptoms may last from a few minutes to a couple of hours.
What’s the difference between Raynaud’s disease and Raynaud’s phenomenon?
Raynaud’s disease or syndrome and Raynaud’s phenomenon are the same condition. Doctors classify Raynaud’s into 2 types: primary (most common) – when it develops by itself and secondary – when it results from another health condition.
Causes of Raynaud’s phenomenon
The cause of Raynaud’s phenomenon is not known exactly, although it appears that the blood vessels in the hands and feet of affected people overreact to cold temperatures or emotional stress or anxiety.
Risk factors
Risk factors for Raynaud’s phenomenon include:
- Being a woman. Women are more likely to suffer from Raynaud’s.
- Living in a cold climate.
- Having other family members affected by Raynaud’s.
- Having certain disorders, such as scleroderma, rheumatoid arthritis or lupus.
- Having disease of the arteries, such as atherosclerosis (buildup of plaque).
- Operating vibrating machinery.
- Exposure to certain chemicals.
- Smoking.
- Taking certain medicines.

Diagnosis
To diagnose Raynaud’s phenomenon usually involves a doctor taking a medical history, examining you and doing some tests, which may include:
- Cold stimulation test: The doctor may ask you to put your hands in cold water to observe whether you show symptoms of Raynaud’s.
- Fingernail examination: The doctor may also wish to look at your capillaries (tiny blood vessels) where your nail meets your finger. These capillaries can look like red pen marks and be enlarged in people with secondary Raynaud’s disease.
- Blood tests may be done to look for signs of conditions which are linked to secondary Raynaud’s. These blood tests may include ANA (antinuclear antibody), ESR (erythrocyte sedimentation rate), and CRP (C-reactive protein).
Raynaud’s disease treatment
There is no simple treatment for Raynaud’s disease. The key to treating Raynaud’s is to try and avoid attacks.
Keep warm: Affected people must do all they can to keep themselves, and particularly their hands and feet, warm. This may mean wearing thick socks and gloves most of the time. Portable hand warmers and feet warmers, such as those sold by skiing or outdoor shops, may help when you are outside for a long time.
Stop smoking: Smoking must be avoided as it makes the problem worse. Avoid stress: Some people find that stressful situations trigger their attacks and, in these people, stress management techniques, such as biofeedback, can help.
Medicines – vasodilators: People who are severely affected by Raynaud’s phenomenon may be advised to take vasodilator medicines – these are prescription medicines which open up the blood vessels and reduce the likelihood of spasm which narrows the vessels.
Avoid trigger medicines: It’s also important to avoid any medicines, including certain over-the-counter cold and flu medicines, such as some decongestants, that can aggravate Raynaud’s disease by increasing blood vessel spasm.
Surgery for Raynaud’s phenomenon
An operation known as a sympathectomy, which divides certain nerves that stimulate blood vessels to contract, may help chronic cases, but is rarely recommended. Alternatively, chemicals can be injected to block these nerves.
It is important to remember that most people with Raynaud’s phenomenon will respond to the treatments available such that Raynaud’s should not interfere with their life too much.
Complications
In severe cases, tissue damage leads to gangrene and the ends of the affected digits die and become black, requiring amputation. Fortunately this is a very rare complication and only occurs if there is an underlying connective tissue disorder.