- General Information
- See Your Pharmacist or Medical Professional
- Treatment Tips
- Treatment Options
- More Information
General Information
Psoriasis is an inflammatory skin condition that can occur anywhere on your skin. It has been reported to affect 2% of the Australian population, with males and females affected equally, and can occur at any age. The most common age for psoriasis to begin is between 20 and 30 years.
About 25% of people find their psoriasis is itchy, and others may have a burning feeling on the skin.
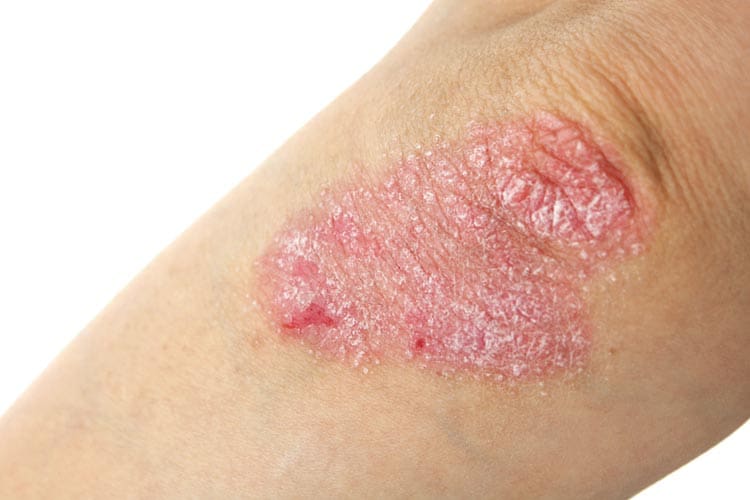
The appearance of psoriasis depends on what part of your body is affected. On areas such as your back, trunk, arms and legs there may be red patches, often covered with thick silvery-white scales (‘plaque’ psoriasis), or there may be small red spots scattered across your skin (‘guttate’ psoriasis).
Psoriasis on your scalp can look like severe dandruff, and there can be hair loss. It can affect your nails, distorting their shape and making them pitted and yellow; this is usually only seen in patients who have had the skin condition for a long time. On the palms of your hands and the soles of your feet, psoriasis can look like pustules, or blisters surrounded by red skin.
Psoriasis can also occur in your skin folds, such as in your groin, under breasts or in your armpits. Here, it often appears as smooth, shiny red patches.
Between 10% and 30% of people with psoriasis will also have psoriatic arthritis, which causes pain, stiffness and swelling of the joints.
Psoriasis tends to come and go over time. There is no cure, but there are treatments available to relieve the symptoms. It is not contagious and cannot spread from person to person. Unlike dermatitis or eczema, psoriasis is generally not itchy.
Triggers for psoriasis
The cause of psoriasis is not known, but it often runs in families, and the environment may affect it.
Some of the known factors that can trigger psoriasis or make it worse include:
- injury to the skin, including severe sunburn
- infections
- stress
- certain medicines
- alcohol
- smoking
- scratching
- hormonal changes
See Your Pharmacist or Medical Professional
- if you think you have psoriasis
- if you do have psoriasis, you may be referred to a dermatologist (skin specialist), who can give you a personalised treatment plan
- psoriasis can be distressing; your doctor can give you advice and refer you to community support organisations
Treatment Tips
- avoid scratching, rubbing or picking at the psoriasis
- keep your skin cool and moisturised to help reduce itching
- avoid soaps which can dry and irritate skin. Instead use soap-free washes
- try to avoid triggers which you know make your psoriasis worse
- don’t smoke
- minimise alcohol
- have a healthy varied diet
- use relaxation techniques to minimise stress
- exposure to the sun may help, but be mindful of the need to balance sun exposure against the risks of skin cancer. The Slip, Slop, Slap, Seek and Slide sun care plan is still recommended.
Treatment Options
- your doctor or dermatologist can prescribe treatments for your psoriasis
- management of your psoriasis may require long-term treatment
- mild psoriasis can usually be managed with creams and ointments
- you may need to try more than one treatment before you find the one that works for you
- emollients and moisturisers can help to reduce dryness and scaling
- more severe psoriasis may need treatment with medicines taken by mouth
- phototherapy may also be prescribed by the dermatologist, and consists of sessions under a sun lamp
- there are some treatments you can buy from your pharmacy which may be helpful to have on hand at home, but always discuss using these with your GP or dermatologist
- not all products are suitable for use by children or during pregnancy or breastfeeding; ask your pharmacist for advice
Emollients and moisturisers
[GENERAL SALE]
e.g. QV range, Aveeno range, Alpha Keri Lotion, Hamilton range, E45 range, Cetaphil range, DermaVeen Baby range
- can be used as often as needed to help soften and soothe skin, reducing cracking and dryness
- when using a new product for the first time, do a patch test to ensure that you are not sensitive to the product. Take a small amount of product and dab it onto a small area of skin. Wait for a few hours. If no redness or irritation is seen, the product should be safe to use on your skin
Coal tar, salicyclic acid and sulphur-containing products
[GENERAL SALE]
e.g. coal tar products (Exorex Psoriasis Medication Topical Emulsion, Ionil T Shampoo, Linotar Gel, Neutrogena T/Gel Therapeutic Shampoo, Polytar Liquid)
e.g. coal tar + salicylic acid (Sebitar Shampoo, Ionil T Scalp Cleanser)
e.g. coal tar + sulphur + phenol (Egopsoryl TA Gel)
e.g. coal tar + salicylic acid + sulphur (Psor-Asist Cream)
e.g. pantothenic acid + retinol + salicylic acid + urea (Psor-Asist Scalp Lotion)
- coal tar, salicyclic acid and sulphur have been used for many years in the management of psoriasis; some products contain a combination of these ingredients
- coal tar may help to reduce itching, scaling and inflammation, and is available in gels, ointments, shampoos and bath products. Be careful when applying as it can stain skin and clothing
- salicyclic acid may help to remove or soften scales and is available in many types of products
- these products are not suitable for use during acute flare-ups or for pustular psoriasis
- don’t apply coal tar products to broken, inflamed or blistered skin
Ichthammol-containing products
[GENERAL SALE]
e.g. Egoderm Cream, Egoderm Ointment, Toppin Ichthammol Ointment
Anti-itch products
[GENERAL SALE]
e.g. Pinetarsol range
Topical steroids
[PHARMACY ONLY]
e.g. hydrocortisone 0.5% (up to 30 g) (DermAid Cream, DermAid Soft Cream, Sigmacort Cream and Sigmacort Ointment, Cortic DS Cream and Ointment)
[PHARMACIST ONLY]
e.g. hydrocortisone 1% (DermAid Cream, DermAid Soft Cream, Sigmacort), clobetasone 0.05% (Eumovate Cream, Kloxema Cream, Becoderm-C Cream)
[PRESCRIPTION ONLY]
e.g. hydrocortisone 1% [more than 30 g]; more potent steroids
- steroid creams should only be used for psoriasis if recommended by your doctor
- they reduce redness, scaling and itching
- do not apply to broken or infected skin
- do not use on your face except on medical advice
- steroid creams can cause permanent thinning of your skin if overused, so apply sparingly and do not use more often than recommended
- do not use steroid creams for longer than 1 week or in children under 2 years old, except on medical advice
More Information
Availability of medicines
- GENERAL SALE available through pharmacies and possibly other retail outlets.
- PHARMACY ONLY available for sale through pharmacies only.
- PHARMACIST ONLY may only be sold by a pharmacist.