What is scoliosis?
Scoliosis is an abnormal sideways curve of the spine. Often as well as the curvature, there is rotation in the spine. Scoliosis is usually diagnosed between 10 and 18 years of age, during periods of rapid growth. The symptoms can range from being very mild and not requiring treatment to severe deformity or pain that may require surgery.
Symptoms
Scoliosis is often noticed by parents or a person as an asymmetry or tilt in the spine, back, shoulders or waist. This asymmetry (difference from one side to the other) is often made more obvious by bending over forwards.
Some signs or symptoms that may be noticed are:
- the head is moved slightly over to one side of the body;
- shoulders are at different heights;
- shoulder blades are at different heights and one is more prominent;
- one hip is sticking out more;
- an obvious curve of the spine is present; or
- a larger gap between the arm and body on one side is visible.
Sometimes, scoliosis is first noticed on X-rays of the lungs or on other medical imaging like a CT scan. Generally, scoliosis doesn’t cause any pain to start with, but pain may develop over the course of the disease.
Often scoliosis will be noticed during times of rapid growth (growth spurts) around puberty. This is usually 6 – 12 months after puberty begins.
Diagnosis
Scoliosis is usually detected by a careful physical examination. Your doctor will identify the curvature of the spine, where the abnormality is, which way it curves and the angle of the curve.
The forward bending test is a simple way for a doctor to detect curves in your spine. The doctor will instruct you to stand with your feet together, place your palms of your hands together and bend over forwards. Leaning forward will generally exaggerate the abnormal curvature.
If there is evidence of scoliosis with the forward bending test, your doctor may suggest you have X-rays. These will be standing X-rays that show the entire spine from the neck to the pelvis, with views from the front and the side.
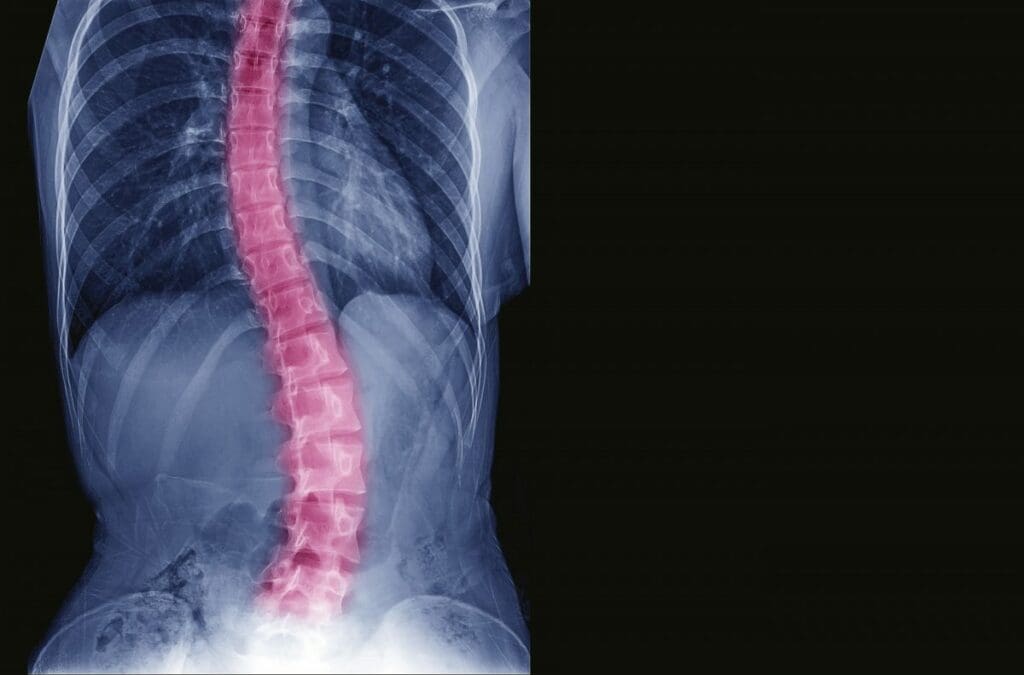
Causes
There are a few types of scoliosis each with their own causes (see below). The cause of the most common type of scoliosis (idiopathic scoliosis) is unknown but doctors know that it tends to run in families. This suggests there is a strong genetic component. Other causes of scoliosis include infections or injuries of the spine and weakness or abnormalities in the muscles or bones in your back.
What are the different types of scoliosis?
Idiopathic scoliosis
Idiopathic scoliosis means scoliosis caused by an unknown factor. Idiopathic meaning a disease due to an unknown cause.
Idiopathic scoliosis can be classified as:
- infantile (develops before 3 years old);
- juvenile (develops between 3 and 10 years old); or
- adolescent (develops between 10 and 18 years old).
Adolescent Idiopathic Scoliosis (AIS) is by far the most common type. Experts agree that genes play a role in the development of AIS, but the exact genes have not been identified. Other theories that have been proposed but not proven include:
- hormonal imbalances such as decreased melatonin or increased growth hormone; and
- structural tissue abnormalities, such as abnormalities in the ligaments, bone or muscles.
Neuromuscular scoliosis
Neuromuscular scoliosis is caused by an underlying disorder of the muscles or nerves, resulting in the trunk and spine not being supported adequately. This may lead to an abnormal sideways curve as the spine grows. Some neuromuscular disorders that can cause scoliosis include:
- cerebral palsy;
- myelomeningocele – a spinal cord defect that impairs movement and sensation; and
- muscular dystrophies – a group of muscle disorders that cause weakness of the muscles.
Neuromuscular scoliosis can also be caused by differences in leg lengths, trauma or infection.
Congenital scoliosis
Congenital scoliosis is due to vertebrae (segments of the backbone) that are abnormally shaped at birth. Congenital scoliosis is usually noticed before the age of 10 years. The abnormal vertebrae can be seen on X-rays.
Syndromic scoliosis
Syndromic scoliosis is scoliosis that is due to a genetic disorder that usually affects bones, muscles and ligaments (e.g. Marfan syndrome). Similar to neuromuscular scoliosis, these disorders disturb the stability of the spine.
Risk factors
There are some factors which increase the risk of adolescent idiopathic scoliosis:
- a family history of scoliosis; and
- being at the peak of a growth spurt.
Male and females are just as likely to have a mild form of scoliosis but scoliosis is more likely to progress to a severe form in females.
Complications
Generally, the long term outcome is positive for people with AIS, whether they are treated with close monitoring by their doctors, with bracing or with surgery.
In juvenile idiopathic scoliosis or in very severe cases of AIS, the abnormal curvature can impact on the lungs and heart which may stop them working as normal. This may increase the risk of lung infections.
There is a slight increased risk of back pain and degenerative disc changes (changes in the spine as you age) in people with scoliosis.
People with severe scoliosis may become self-conscious about their uneven hips, shoulders and prominent ribs.
As scoliosis can often be identified by you or your family, Scoliosis Australia has created a National Self-Detection Program for girls between 10 and 13 years old.
Treatment
Treatment for adolescent idiopathic scoliosis is aimed at preventing progression of the spinal curvature until your child is fully grown. Once a person is fully grown, scoliosis rarely progresses. Treatment is based on the initial curvature of the spine and the rate of progression.
Treatment options include:
- Monitoring the curvature over time using X-rays – used for mild forms of scoliosis.
- Bracing of the back – used in people with moderate scoliosis. In Australia, the most common scoliosis brace used is the Boston Brace. It is a rigid brace that you wear beneath your clothes. The more hours you wear the brace, the more effective it is in stopping the progression of scoliosis. Many teenagers feel insecure about their brace and it is important to talk to a psychologist if it is affecting you.
- Surgical spinal fusion with the use of instrumentation such as metal plates, wires, rods, hooks or screws – reserved for severe scoliosis
It is generally advised to maintain regular exercise with a focus on strengthening and conditioning core muscles.
Surgery
Surgery for scoliosis is aimed at preventing progression of the spinal curvature. An orthopaedic surgeon will perform the surgery which generally involves fusing vertebrae together and using instrumentation to secure the spine.
The choice of surgical approach and instrumentation is determined by the type of abnormality and the surgeon’s personal preference. Spinal deformity surgery is a major surgery with a number of risk factors that you should closely discuss with your surgeon.
What type of doctor looks after scoliosis?
GPs are the main point of contact for looking after people with scoliosis. If you have moderate or severe scoliosis, then an orthopaedic surgeon will generally be involved in your care and follow up. Physiotherapists may play an important role in strengthening certain muscle groups to help with your posture and pain associated with scoliosis. Psychologists should be able to help you cope with insecurities around wearing a brace or appearing different to your peers.
Support
Your local GP will be able to advise you of local scoliosis support groups. Scoliosis Australia has many online resources for parents or people with scoliosis, including a list of spinal specialists with a particular interest in scoliosis.
Outlook
The outlook for people with scoliosis is excellent. Most people with scoliosis are able to have a normal life involving exercise, work and relationships.