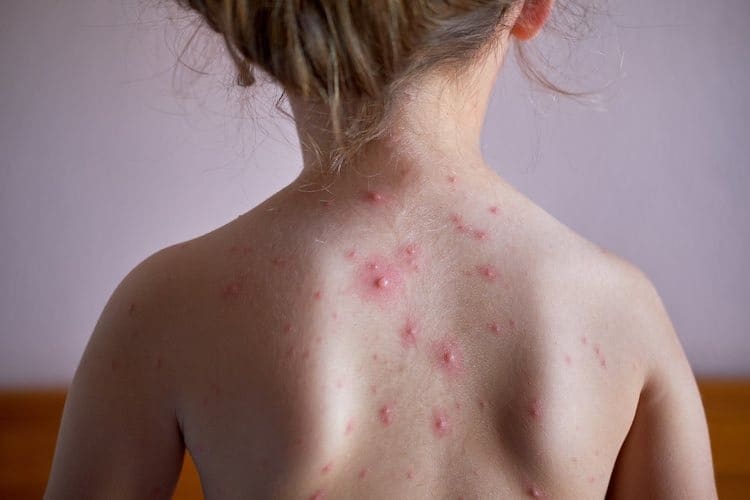
Chickenpox is a highly contagious disease that’s caused by infection with the varicella zoster virus. Most children with chickenpox develop an itchy rash that lasts for about 10 days. Overall, chickenpox tends to be a mild illness in children. Adults with chickenpox often feel more unwell and they are more likely to develop complications than children.
People with chickenpox are infectious from 2 days before the rash appears until the time scabs have formed on the last of the sores. This is usually around 7 days after the rash first appeared. Children should be kept at home until the last crop of sores has formed scabs.
There are treatments available to ease the symptoms of chickenpox, and a vaccine against chickenpox is part of the routine childhood vaccinations in Australia.
What are the symptoms of chickenpox?
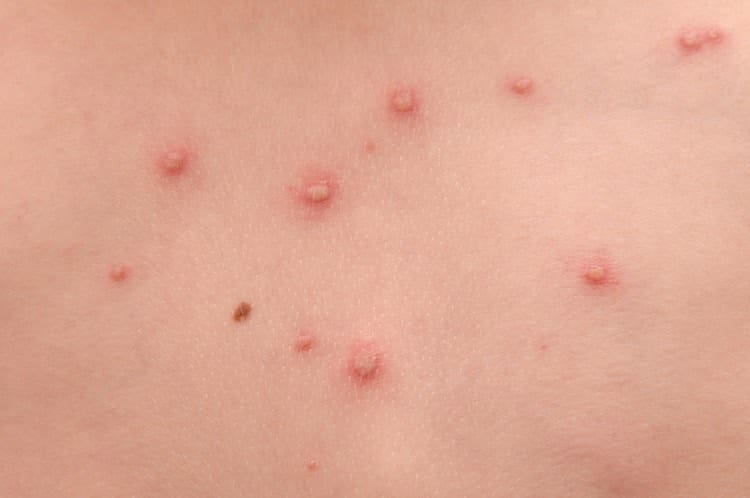
The first symptoms are usually flu-like symptoms, such as a fever, mild headache, tiredness, sore throat and loss of appetite. These initial symptoms are quickly followed by a red and spotty rash. The spots quickly develop into fluid-filled blisters that look like pimples.

The rash normally starts on the chest, face and back, and then spreads to other parts of the body including the scalp, arms and legs. It is usually very itchy. The blisters dry up and form a crust or scab within about 5 to 10 days.
Some children develop only a few spots while others have them all over their bodies — including in the mouth, eyelids, inside the nose and in the vagina in girls.
Most children start to feel better after about a week.
See Your Pharmacist or Medical Professional
- if the person affected has an illness affecting their immune system or is taking medications which can affect the immune system, such as prednisone
- if the person affected is pregnant
- if joint pain develops or the person has a severe headache, high fever or vomiting
- if the skin around the sores becomes very red and warm or there is pus present; sometimes bacteria can get into the sores and cause an infection
What causes chickenpox?
Chickenpox is caused by the varicella-zoster virus. The same virus also causes herpes zoster (shingles).
The virus is spread from person to person by sneezing and coughing or by direct contact with an infected person’s blisters. After being infected it takes 10 to 21 days for symptoms to appear – the ‘incubation period’ (usually symptoms develop after 14 to 16 days).
Chickenpox is less common among children these days because most children are vaccinated against it as part of their routine childhood vaccinations. Since the introduction of the varicella vaccine in Australia in 2005, hospital admissions for chickenpox in children under 15 has fallen significantly.
Can you catch chickenpox from someone with shingles?
People usually only have chickenpox once in their life but the virus can lie dormant in the body for many years afterwards. Shingles is caused by reactivation of the chickenpox virus later in life. Chickenpox can be caught from a person with shingles, but shingles cannot be caught from another person, including someone with chickenpox.
Complications
Complications from chickenpox are uncommon in otherwise healthy children. Children with problems with their immune systems or other health problems as well as adults and newborn babies are at higher risk of complications.
Possible complications of chickenpox include:
- pneumonia;
- bacterial skin infections;
- joint or liver inflammation; and
- encephalitis (inflammation of the brain), which is a rare complication.
Do chickenpox blisters scar?
If chickenpox blisters are scratched or picked at, they can leave a scar. These are sometimes called pockmarks. If a blister becomes infected it is also more likely to leave a scar.
Children should be encouraged to leave the spots alone and use anti-itch medicines to soothe the itching.
Tests and diagnosis
Most children with chickenpox can be cared for at home. If you are not sure if your child has chickenpox or your child is unwell, see your GP (general practitioner).
Your doctor will ask about your child’s symptoms and whether you’ve been in contact with anyone who has recently had chickenpox. They will also want to know how long your child has had symptoms and whether they are getting worse. They will check if your child has been vaccinated against chickenpox.
Your doctor will examine your child, looking especially at the rash. In most cases the diagnosis can be made based on the symptoms and appearance of the rash. Tests are rarely needed, but fluid from the blisters can be collected and tested for varicella-zoster virus in some cases.
Treatment of chickenpox
Most children can be treated at home with medicines and self-care remedies that help control the symptoms. Sometimes antiviral medicines are needed for severe cases or for children at higher risk of complications.
Treating itch
For some children, the rash may be no more than a passing inconvenience, but for others it can be very itchy and unpleasant.
Asking your child not to scratch will probably fall on deaf ears, however it is worth trying to distract them as much as you can. Cut their fingernails very short and make sure that their hands and fingernails are kept clean. It might be worth putting mittens or cotton gloves on very young children to stop them scratching.
If the rash or sores are very itchy, try a warm (but not too hot) bath with half a cup of baking soda. Your pharmacist or doctor will also be able to recommend some anti-itch preparations. Calamine lotion and cool compresses can also be useful.
Topical anti-itch products
[GENERAL SALE]
e.g. Pinetarsol, Eurax, Stop Itch cream, Calamine Lotion, Paraderm Plus, SoloSite Gel
- Pinetarsol can be added to bathwater, or diluted and dabbed onto skin to relieve itching. When using Pinetarsol bath oil be cautious of slipping in the bath or shower
- Eurax cream and Paraderm Plus can be used as long as the skin is unbroken
- Calamine Lotion is a traditional remedy for itching but is drying to the skin, increasing the chances of leaving behind scars once the skin heals
- an alternative option that is not drying to the skin is SoloSite Gel
- baking soda (sodium bicarbonate) may also relieve itching; add half a cup to a warm bath
Oral anti-itch products
[GENERAL SALE]
e.g. cetirizine (Zyrtec), desloratadine (Aerius), fexofenadine (Telfast), loratadine (Claratyne)
- these non-sedating or less-sedating antihistamines are available at general sale or pharmacy only (depending on the quantity).
- some of these products are available in various formulations, such as liquid or chewable tablets
[PHARMACIST ONLY]
e.g. dexchlorpheniramine (Polaramine), promethazine (Phenergan, Sandoz Fenezal)
- promethazine and dexchlorpheniramine are antihistamines which can reduce itching
- they often make people feel drowsy and so can assist with sleep, which is helpful if the child is scratching at night
- promethazine and dexchlorpheniramine are available only on prescription if the child is under two years old
Treating pain and fever
Paracetamol can be given as directed to reduce fever. Do not give aspirin or nonsteroidal anti-inflammatory drugs (NSAIDs) to children with chickenpox.
Paracetamol can also help relieve discomfort associated with blisters in the mouth or other areas where local treatments can’t be used.
Medicines to reduce fever and relieve pain
[PHARMACY ONLY]
paracetamol liquid preparations (Dymadon Drops, Dymadon Suspension, Panadol (Children), Panamax Elixir, Panamax 240 Elixir)
- paracetamol is suitable for most people but it is important not to give more than the recommended dose; check labels for dosage instructions appropriate to the age and weight of the child
- paracetamol is also available in other forms (e.g. tablets, soluble tablets, capsules and suppositories), which are often medicines classified as for General Sale; these may be preferred by older children and adults (check labels for dose appropriate to age and weight; you can also ask your pharmacist for advice)
- paracetamol is a common ingredient in other medicines, e.g. cold and flu preparations (which may be used by adults and adolescents), so be careful not to double dose
- the routine use of paracetamol to prevent fever at the time of vaccination is no longer recommended except for children with a history of seizures
- ibuprofen is not recommended because of reports of rare, but serious, skin complications when it is used in children with chickenpox
Staying hydrated
Make sure your child rests and drinks plenty of fluids. Water, soups, other fluids, ice blocks and jelly can be offered. Don’t worry if they don’t eat as much as usual while they are sick.
Antibiotics and antiviral medicines
Chickenpox is caused by a virus, so antibiotics are not needed unless your child develops a bacterial skin infection. Skin infections usually develop as a result of scratching the blisters.
Most children do not need to take antiviral medicines. Antivirals may be recommended for children with complicated or severe chickenpox, or those with lowered immunity. Some children with severe eczema may also need treatment with antiviral medicines to reduce the risk of severe chickenpox and complications.
Antivirals may be prescribed for adults if they can be started soon after the rash appears.
Other products
[PHARMACY ONLY]
e.g. Solugel, Solosite Wound Gel
- these water-based gels have a cooling effect
- they are applied over affected areas and covered with a dressing
- they may help reduce infection and scarring
Treatment Tips
- encourage the child or person to drink plenty of fluids
- encourage the child or person to get plenty of rest
- give paracetamol to reduce fever and ease any pain (see Treatment Options below)
- do not give aspirin to children under 16 years of age because it may cause Reye’s syndrome, a serious condition
- avoid scratching as much as possible; cut nails extra short and keep hands and fingernails clean to reduce the chance of skin becoming infected
- try using an anti-itch product if itching is a problem
- wear loose-fitting clothes
- antiviral tablets may be prescribed for adults or for severe cases of chickenpox
- avoid contact with people who have not had chickenpox and ensure good hygiene (e.g. wash hands, cover mouth when coughing) to prevent spread
Vaccination
Vaccination against chickenpox is recommended for all children in Australia at 18 months. The vaccine is given as a combined MMRV (measles-mumps-rubella-varicella) vaccine, and is available free of charge as part of the Australian National Immunisation Program Schedule.
An additional dose may be given to increase protection, but this second dose is currently not funded on the National Immunisation Program. The second dose can be given anytime from 4 weeks after the first dose.
Catch-up vaccination is also recommended for adolescents aged 10 years and over (free on the National Immunisation Program) and adults (on private prescription) who have not had chickenpox or who have not had the chickenpox vaccine previously. People aged under 14 need at least one dose (only one is free) – a second dose will boost immunity. People over 14 are recommended to have 2 doses (both doses are free to those 14-19 years old). Two doses of vaccine are also required in adults for adequate protection, but adults will have to pay for a private prescription.
People who have not been vaccinated may be protected if they get a chickenpox vaccine within a few days of being exposed to the virus. Ask your doctor about vaccination in these circumstances.
Side effects of varicella vaccination
Side effects may include pain, redness and swelling of the skin where the injection was given. Less common side effects include a rash, which usually lasts less than a week, and fever. Febrile convulsions can happen, although this is uncommon.
The tepid sponging of a child to reduce fever after receiving a vaccination is no longer routinely recommended, as it may cause vasoconstriction, reducing heat elimination and increasing temperature.
Does the chickenpox vaccine always work?
Getting vaccinated greatly reduces your chances of getting chickenpox. However, some people do still get chickenpox despite being vaccinated.
Vaccinated children who get chickenpox usually have a much milder form of the illness, with fewer spots and lower fever. They also recover faster than children who have not been immunised.
When can my child go back to school?
Chickenpox is infectious from 2 days before the rash appears until after scabs have formed on all the blisters. This usually takes at least 5 days from when the rash first appeared in non-immunised children and less time in immunised children. Do not send your child to school, preschool or daycare during this time.
You should keep your child at home and away from others until they are no longer contagious. Your child can return to their usual activities when all of the blisters have scabbed over.
Exclusion of contacts: any child with an immune deficiency, such as leukaemia or receiving chemotherapy should be excluded for their own protection.
Key to medicines information
Availability of medicines
- GENERAL SALE available through pharmacies and possibly other retail outlets.
- PHARMACY ONLY available for sale through pharmacies only.
- PHARMACIST ONLY may only be sold by a pharmacist.
- PRESCRIPTION ONLY available only with a prescription from your doctor or other health professional.