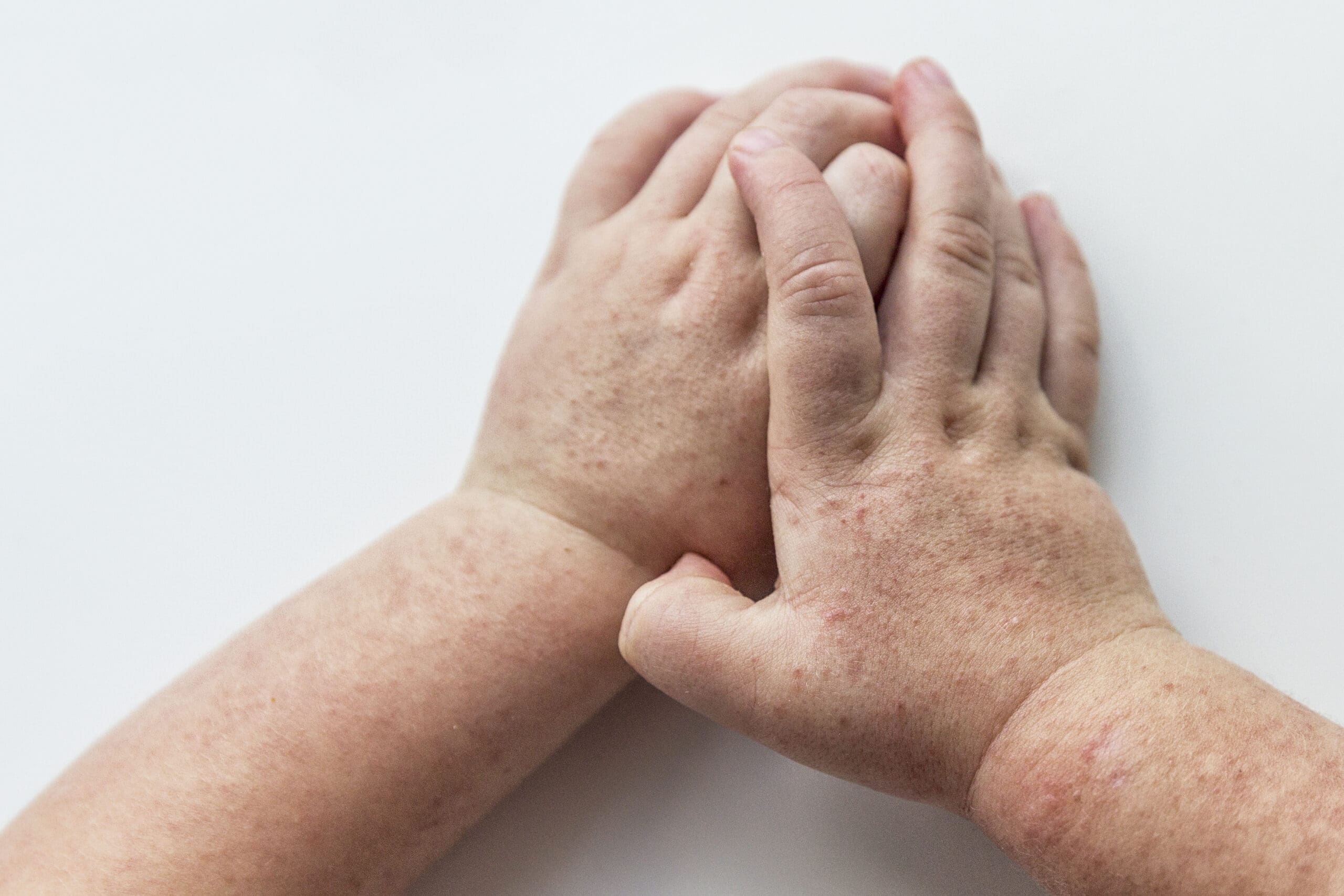
What is scarlet fever?
Scarlet fever is a condition that can occur in people who are infected with a bacterium called Streptococcus pyogenes which belongs to the group A streptococci. Scarlet fever mostly affects children and usually starts as a ‘strep throat’ infection and is followed by the development of a rash. Scarlet fever was a common and dangerous condition during the 19th century, however has since become rare and now usually only causes a mild illness. With antibiotic treatment, most children recover fully within a week without any complications.
Signs and symptoms
The main symptom of scarlet fever is a rash. The rash is red with lots of small bumps that make it feel like sandpaper. It usually starts on your underarms, then spreads to the rest of your body. It is often most noticeable in the skin folds of your underarms and groin. If you press on the rash it goes pale or white.
Your face may become flushed; however, the skin around the mouth is usually unaffected. Your tongue can develop a white coating which then peels and leaves it red and bumpy, giving it a strawberry-like appearance.
There may also be symptoms of ‘strep throat’ which include:
- sore throat;
- fever;
- headache;
- nausea and vomiting;
- fatigue; and
- swollen neck glands.
Rarely, scarlet fever happens after a skin infection called impetigo, also known as ‘school sores’, when it is caused by Streptococcus. The main symptom is a rash covered by a honey-coloured crust, most commonly on the face.
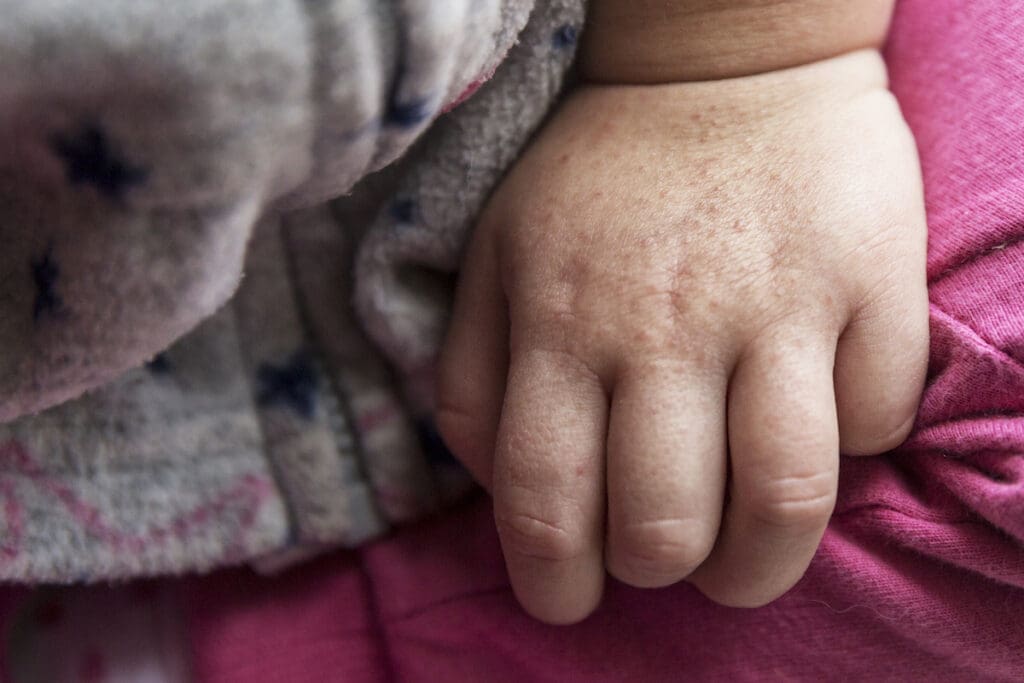
What causes scarlet fever?
Scarlet fever is caused by infection with group A streptococci (group A strep) bacteria. The bacteria usually infect your throat (‘strep throat’) or skin (‘school sores’). The bacteria then release toxins which cause inflammation of the skin and lead to the development of the rash.
Group A strep is found in the saliva and mucus of an infected person. When they cough, sneeze or talk, small droplets containing the bacteria are spread through the air and may be breathed in by nearby people. The droplets may land on things such as towels, cups or cutlery, which can then spread infection to other people if they are used before being washed.
Only a very small number of people infected with group A strep will develop scarlet fever. If you do develop scarlet fever, it usually takes 2-5 days for the symptoms to start after you get infected.
Who gets scarlet fever?
Anyone can get scarlet fever; however, it is most common in children between the ages of 5 and 15. You are at an increased risk for scarlet fever if somebody else in your house is infected with group A strep and they are coughing or sneezing. School teachers and daycare workers have a higher risk of getting scarlet fever compared with other adults because of the amount of time they spend in contact with children.
How common is scarlet fever?
Scarlet fever was a common and dangerous disease in children during the 19th century. It became much less common during the 20th century and now usually only causes mild illness. This decline is thought to be due to improved hygiene, less overcrowding and the development of antibiotics.
In recent years, however, scarlet fever has been on the rise again in many countries, including England and China. In England, the number of people diagnosed with scarlet fever increased from 4700 in 2013 to 19,000 in 2016. The reason for this rise is uncertain, and it doesn’t seem to be slowing down.
In Australia, the exact number of people who are diagnosed with scarlet fever each year is unknown.
Complications
Complications from scarlet fever have been rare since the development of antibiotics, although they can still happen if the diagnosis is missed or treatment is delayed.
Rheumatic fever
One of the most serious complications of scarlet fever is rheumatic fever. This happens when the toxin produced by group A strep causes inflammation to the heart, brain, joints and skin. Symptoms usually start 2-3 weeks after you recover from scarlet fever and include fever, joint pain, small bumps on the skin, and involuntary jerky movements of the hands and feet.
Rheumatic fever is rare in Australia and almost exclusively occurs in Aboriginal and Torres Strait Islander people.
Spread of the infection
Other complications of scarlet fever are due to the bacteria spreading to other parts of the body. This can lead to:
- otitis media (middle ear infection)
- sinusitis (sinus infection)
- an abscess (collection of pus) behind the tonsils.
How is scarlet fever diagnosed?
If your child has a rash or sore throat, they should be seen by a doctor. The doctor will usually examine the rash and their tonsils. Your doctor may take a throat swab for a rapid strep test or a throat culture to confirm the diagnosis. The rapid strep test can be done in your doctor’s office and usually takes 10-20 minutes for a result. If this test is negative but your doctor still suspects scarlet fever, they may send the swab to a laboratory for a throat culture. It can take several days for a result to come back, however the throat culture may identify an infection that the rapid strep test has missed.
Treatment
Scarlet fever is usually treated with antibiotics. There are three main benefits to using antibiotics: they improve your speed of recovery; reduce the chance of spreading the infection to friends and family; and help prevent the development of complications.
The most common antibiotic used to treat scarlet fever is penicillin. Other antibiotics can be used if a person is allergic to penicillin. It is important that a person takes all antibiotics prescribed by the doctor, even after they start to feel better.
Scarlet fever is contagious up until 24 hours after antibiotics are started. To prevent the spread of infection to other children, your child should not go to school or daycare until they have had 24 hours of antibiotic treatment and they feel well.
Other things that will help with recovery include:
- lots of rest;
- drinking plenty of fluids;
- paracetamol to help with the fever and sore throat; and
- throat lozenges, syrups and gargles to help the sore throat.
How long will the symptoms last for?
Scarlet fever is usually a mild illness. The rash begins to fade after 3 to 4 days and sometimes the skin over the face, palms and feet will peel off like a sunburn. This skin peeling may last for up to a month.
What type of doctor treats scarlet fever?
Scarlet fever can be diagnosed and treated by your general practitioner or by a paediatrician.
Prevention
There are things that you and your child can do to prevent the spread of scarlet fever infection. These include:
- stay home from school or work until 24 hours after starting antibiotics and you are feeling well;
- cover your mouth and nose when you cough or sneeze;
- wash your hands often, particularly after coughing or sneezing, and before eating or preparing food;
- avoid sharing things like towels, cups and cutlery; and
- wash dishes every time they are used.