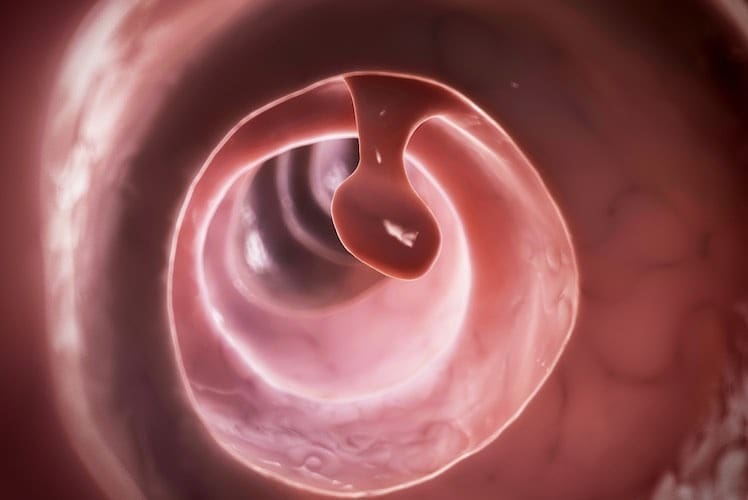
Bowel polyps, also known as colon polyps, are small growths of tissue on the wall of the colon (large bowel) or rectum. Most polyps are small, usually less than 1cm in size, although they can grow larger. Polyps can appear in many forms: they may look like a small raised lump, a wart, a grape or a mushroom on a stalk or a cluster of many small bumps. Some people have just one polyp, while others can have several.
Most polyps are harmless, but over time some can develop into bowel cancer. That’s why they are usually removed if found.
Types of bowel polyps
The 2 most common types of polyps are adenomas and hyperplastic polyps.
- Adenomas (adenomatous polyps): These are usually small, less than one cm in diameter; there is a small risk that they will develop into cancer; most bowel cancers develop from an adenoma that has been present for 5 to 15 years.
- Hyperplastic polyps: these polyps are very small, usually less than half a centimetre in diameter; generally considered harmless as they do not usually develop into cancer, except very rarely.
What are the symptoms of bowel polyps?
In most cases, polyps do not cause any symptoms, and are often discovered by accident (e.g. during routine bowel screening or another investigation).
However, sometimes larger polyps (those over one centimetre in size) cause some symptoms. These may include:
- Rectal bleeding.
- Change in bowel habits (mucus in the stool; constipation or diarrhoea that lasts longer than one week).
- Change in stool colour (stools may appear black or streaked with blood).
- Crampy abdominal pain, nausea or vomiting.
What causes colon polyps?
Bowel polyps are thought to develop because of an abnormal production of cells in the lining of the bowel. This process may occur because of a fault or mutation in a person’s genes. It results in an overgrowth or cells, causing a polyp to form.
Who gets bowel polyps?
Anyone can develop bowel polyps, but they are more common in people aged over 50 years. Around one-quarter of all Australians will develop bowel polyps during their lifetime.
Polyps can run in families, so some people are more likely to develop polyps if a family member has polyps. People with a family history of bowel cancer are also more likely to develop polyps.
Other things that may increase a person’s risk of developing bowel polyps include:
- Smoking.
- Obesity.
- Lack of exercise.
- Excess alcohol consumption.
- Poorly controlled type 2 diabetes.
- Inflammatory bowel disease.

Do bowel polyps mean I have cancer?
Most bowel cancer develops from polyps, but having polyps does not mean a person will get cancer. Only a small percentage of polyps turn into cancer – most often the adenomas. It can take anywhere from 5 to 15 years for a polyp to turn into cancer. The risk can depend on the size, number and characteristics of the polyp. Because most bowel cancer begins as polyps, all polyps should be removed when found. The earlier they are removed, the less likely it is that they will turn into cancer. If a person has any adenomas removed they will usually need ongoing screening to check for the development of more polyps or signs of bowel cancer.
Several rare genetic conditions can cause bowel polyps to develop, and these have much greater risk of turning into cancer. For example, in people with familial adenomatous polyposis (FAP), a hundred or more small polyps develop on the colon, so that it looks like a carpet of small raised lumps. Several members of a family may suffer from this condition. If FAP is not recognised and treated, there is almost a 100% chance that a person will develop bowel cancer before the age of 50. Therefore, all people who have a relative with FAP should have regular bowel screening. Most people with FAP are advised to have their large intestine removed to prevent cancer.
How are colon polyps diagnosed?
Because there are often no symptoms, bowel polyps are usually found during a bowel cancer screening test or a bowel investigation for another reason. Most bowel polyps are found through a colonoscopy, which is a type of investigation that looks at all parts of the colon. A colonoscopy involves inserting a thin, flexible tube into the rectum. The tube known as a colonoscope, has a light and camera attached so that images can be relayed onto a screen and the doctor can see any polyps. The tube is long enough to examine the full length of the colon and also allows the doctor to take samples of tissue to examine or remove the polyp.
Sometimes, a bowel polyp is diagnosed with other tests such as a sigmoidoscopy (like a colonoscopy, but uses a shorter tube to examine the rectum and lower part of the colon).
People aged over 50 and those with a greater risk of developing polyps or bowel cancer require regular bowel screening to check for polyps and other changes in the bowel.
How are bowel polyps treated?
Bowel polyps are usually removed, even if they are not causing symptoms. This helps minimise the development of bowel cancer.
Bowel polyps can be removed during a colonoscopy. Duriing the procedure, the doctor manoeuvres a long wire loop through the colonoscope and around the base of the polyp. The loop is pulled tight, cutting off the polyp. Surgery is rarely needed to remove polyps, but may be necessary if the polyps are very large or can’t be reached safely during the colonoscopy.
After removal, the polyp is sent to a pathology lab to check for any signs of cancer. The lab will also be able to tell if the polyp has been entirely removed or if there is a chance of it growing back.
If any signs of cancer are found, further treatment may be required.
Can colon polyps be prevented?
A person can lower their risk of developing bowel polyps by having regular check-ups and taking part in recommended bowel screening programs.
It can also help to:
- Eat a healthy diet that’s high in fibre and low in fat.
- Stop smoking.
- Do regular exercise and maintain a healthy body weight.
- Reduce alcohol intake.