What is myotonic dystrophy?
Myotonic dystrophy is a muscle condition that falls under the umbrella term ‘muscular dystrophy’. The muscular dystrophies all have three features in common; they are hereditary, they are progressive; and each causes a characteristic, selective pattern of muscle wasting and weakness.
Myotonic dystrophy is the most common adult form of muscular dystrophy – thought to affect at least 1 in 8,000 people worldwide. Unlike the other muscular dystrophies, the muscle weakness is accompanied by myotonia (delayed relaxation of muscles after contraction) and by a variety of symptoms that affect parts of the body other than the muscles. Myotonic dystrophy can affect both males and females.
Myotonic dystrophy is often abbreviated as DM after its Latin name dystrophia myotonica and is also known as Steinert’s disease. There are two forms of myotonic dystrophy, usually referred to as type 1 or DM1 and the rarer type 2 or DM2. Both conditions are genetic disorders but each affects a different gene.
In this factsheet:
- What are the symptoms of myotonic dystrophy?
- What is the age of onset?
- How is myotonic dystrophy diagnosed?
- What causes myotonic dystrophy?
- How does a person get myotonic dystrophy?
- Do people with myotonic dystrophy become disabled?
- What is congenital myotonic dystrophy?
- What is type 2 myotonic dystrophy (DM2)?
- Is there any specific treatment?
- What research is being done?
What are the symptoms of myotonic dystrophy?
There is a wide range of severity of myotonic dystrophy and symptoms may appear at any time from birth to old age. Some people may only start to show some mild signs as adults and the rate of deterioration is usually slow, with little change over a long period; some people never have significant muscle disability and many live a normal life span. At the other end of the spectrum some babies are born with a severe form of the condition called – congenital myotonic dystrophy.
One of the first signs of myotonic dystrophy is often muscle stiffness – delayed relaxation of voluntary muscles after contraction (myotonia). This is often noticed when trying to release the hand from a grip – when shaking hands with somebody for example. However, this is generally less noticeable after the early stages of myotonic dystrophy.
The first muscles to be affected by weakness are those of the face, neck, hands, forearms, and feet. The large, weight-bearing muscles of the legs and thighs are much less affected.
Myotonic dystrophy can affect the tissues and organs of many body systems in addition to the muscles. The list includes heart problems, cataracts, trouble breathing, adverse reactions to anaesthesia, difficulty swallowing, digestive problems, excessive daytime sleepiness and, in children, learning difficulties. Hormonal problems may also occur including reproductive abnormalities, thyroid dysfunction and diabetes. Consequently myotonic dystrophy may present itself in what one expert has called a “bewildering variety of ways”. Note that not everybody with myotonic dystrophy has all of these problems.
What is the age of onset?
About half of those with the disorder show visible signs by about twenty years of age, but a significant number do not develop clear-cut symptoms until after age fifty. However, when myotonic dystrophy is suspected (because it is present in other members of the family) careful examination may reveal typical abnormalities before obvious symptoms appear. There are also less common forms of myotonic dystrophy with onset in infancy or childhood.
The condition tends to be more severe and have an earlier age of onset with each generation in a family. So a grandparent might experience their first mild symptoms at age 60, while their children notice symptoms at 30, and grandchildren may be born with severe symptoms – congenital myotonic dystrophy.
How is myotonic dystrophy diagnosed?
A physical examination will usually reveal the typical pattern of muscle weakness and wasting and the presence of muscle stiffness (myotonia). In addition, early in the disease process, weakness and wasting of facial, jaw, and neck muscles, and frontal balding of men often give the face a characteristic look. However, as many doctors are unfamiliar with myotonic dystrophy, getting the correct diagnosis can take some time. Complicating the immediate recognition of myotonic dystrophy is the fact that patients frequently first seek medical attention for one of the conditions accompanying muscle involvement. In particular eye problems are what may bring a patient to the doctor’s office.
Tests that may be done to confirm the diagnosis include a blood test, a muscle biopsy, and an electromyogram (EMG). The most precise diagnosis is made by analysing the DNA in a blood sample as it will look for the specific genetic error that causes DM1 or DM2.
What causes myotonic dystrophy?
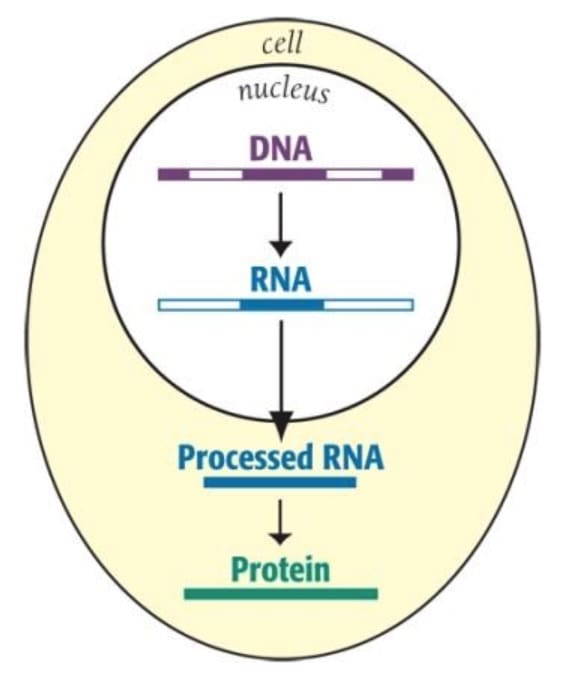
A molecule called ‘RNA’ is key to causing myotonic dystrophy. RNA is the carbon copy of DNA that carries genetic messages from the centre of the cell (the nucleus) to the rest of the cell in order to build proteins.
In myotonic dystrophy the extra repeats in the RNA copy of the DMPK gene cause it to fold in half into a hairpin shape and get stuck inside the nucleus. This toxic RNA then hooks onto certain proteins inside the nucleus, trapping them in clumps. The proteins held in these clumps are then unable to perform their normal functions. For example, the protein known as ‘MBNL1’, which has a crucial role in ensuring that the genetic information in certain genes is properly assembled, is trapped by the toxic RNA. Determining which proteins are held and what effect this has on the body is very complex and has taken many years to unravel. This complex mechanism explains how a single genetic change can affect many different processes in the body.
Generally the more repeats a person has, the younger they are when symptoms are noticed and the more severe their condition is. Although individuals with a similar repeat count may be quite differently affected. Severely affected children born with symptoms may have several thousands of repeats. The number of repeats tends to increase in each generation of a family, resulting in the increasing severity that was mentioned above. This phenomenon is known by geneticists as ‘anticipation’.
See below to find out what causes myotonic dystrophy type 2 (DM2).
How does a person get myotonic dystrophy?
Myotonic dystrophy is inherited in an ‘autosomal dominant’ pattern. This means that only one myotonic dystrophy gene inherited from either the father or mother, is required to cause the condition. On average half of the children of a person with myotonic dystrophy will have the condition. Both men and women are equally likely to be affected and to pass on the disorder, but affected women are more likely to have a severely affected child.
Very few cases of myotonic dystrophy occur ‘out of the blue’. Almost always, one parent proves to be affected, often very mildly. Some parents (or grandparents) prove to carry a very slight genetic change that will never give them symptoms. Relatives of people with myotonic dystrophy can have genetic testing on a blood sample to find out whether they have the condition and the risk of passing it on to their children, but this should always be done as part of genetic counselling. Genetic testing of healthy young children is not recommended.
Do people with myotonic dystrophy become disabled?
The course of myotonic dystrophy varies too widely, even in the same family, to permit a general statement about its effects. On the one hand, there are people with the disorder whose symptoms are so mild they hardly know anything is wrong. Whatever muscle weakness they experience is something they take for granted and adapt to. In some cases, the only symptom may be a cataract. Nevertheless these people do indeed have myotonic dystrophy and can transmit a serious case of the condition to their children.
For the most part, weakness and wasting slowly progress to the point of some disability, moving beyond the muscles originally involved to those of the shoulders, hips, and thighs. As a rule, disability rarely becomes severe until fifteen to twenty years after the onset of symptoms. The older a person is when muscle weakness is first noticed, the slower is the progression and the less serious the consequences.
What is congenital myotonic dystrophy?
Congenital myotonic dystrophy is the early childhood form of myotonic dystrophy. As the name indicates, it is present at birth, almost invariably in infants whose mothers are so mildly affected by myotonic dystrophy that they are unaware of it. Congenital myotonic dystrophy is a rare variant of the disease with striking differences from the form it takes among adults.
In the newborn period, an affected infant is profoundly weak and floppy, has difficulty with sucking and swallowing, and may have trouble breathing. Respiratory problems may continue after the birth, and can be very severe and life threatening, especially if the baby is premature. Once the neonatal period (28 days after birth) has passed, the respiratory problems tend to improve.
Parents, family and carers should be aware that these children often have facial weakness which makes it difficult to make facial expressions – it doesn’t mean the child is unresponsive. This may improve with time. Older children tend to have poor motivation and concentration and are easily tired. The motor and intellectual milestones tend to be delayed in a child with congenital myotonic dystrophy. Speech therapy can help with speech difficulties and a stimulating environment can help with learning and development.
Feeding difficulties are common and input from a range of professionals will be needed to manage this. Special bottles, food supplements, tube feeding (nasogastric tube) and/or IV drips may be needed at different stages. Some children have a squint, and very occasionally children may have impaired vision. Children commonly have club feet (talipes). This can be helped by physiotherapy but if severe corrective surgery will be required. The development of control over the bladder and bowel are sometimes delayed and problems with constipation may persist.
Generally, the condition improves through the early years but deteriorates during late childhood and adolescence, when the ‘adult’ features of the disease gradually emerge. Congenital myotonic dystrophy can vary considerably in severity from child to child but sadly, congenital myotonic dystrophy can be fatal, especially in the early weeks of life. However, a child who lives beyond his or her first birthday is likely to live to become an adult.
What is type 2 myotonic dystrophy (DM2)
Type 2 myotonic dystrophy, also sometimes called ‘PROMM’ (proximal myotonic myopathy), is only found in adults, with an age of onset generally between 30 and 60 years. People with DM2 do not usually have the same kind of facial muscle weakness or swallowing problems that are often seen in DM1. Weakness usually affects the muscles closest to the trunk particularly the thighs, and for many patients this is the most disabling feature later in life. It is quite common for DM2 patients to experience muscle pain. In common with DM1 patients, DM2 patients may experience cataracts, heart problems and diabetes.
DM2 is caused by the inheritance of extra pieces of repeated DNA in the ‘CNBP’ gene (also known as ‘ZNF9’) – a different gene to that causing DM1. In DM2 a four letter DNA code is repeated many hundreds of times instead of the usual number which is less than thirty. Unlike DM1, it appears that ‘anticipation’ (repeat count increasing with each successive generation) is not a feature of DM2. The extra DNA repeats inherited by DM2 patients are thought to cause the symptoms of the disease in a similar way to those inherited in DM1 (described above).
Generally DM2 is thought to be much less prevalent than DM1 but this appears to vary in different populations, for example DM2 is thought to be almost as common as DM1 in Germany.
Is there any specific treatment?
No specific treatment has yet been found for the muscle weakness and wasting in myotonic dystrophy, although ankle and leg braces can help to support muscles as weakness progresses. There are also medications that can relieve the myotonia. Heart problems, cataracts, and other abnormalities associated with the disease can also be treated.
Exercise, including range of motion, strengthening and aerobic exercise, is important for the management of myotonic dystrophy. This helps to maintain strength in the muscles for as long as possible and also keep the cardiovascular system healthy. Range of motion exercises are important in maintaining joint function and may play a role in reducing pain that is caused by muscular imbalance or tightness. Since people with myotonic dystrophy often have heart problems, any exercise programme should be undertaken under the guidance of a physiotherapist or other medical professional. Please see the link at the bottom of the page for more information about physiotherapy for myotonic dystrophy.
What research is being done?
Ever since scientists started to understand how the DNA change in people with myotonic dystrophy was exerting its effect in the late 1990s, they have been searching for potential treatments that could stop the chain of events that leads to the symptoms of myotonic dystrophy. There are several strategies that are being researched to specifically block the toxic RNA that is present in the cells of people with myotonic dystrophy (please see ‘What causes myotonic dystrophy’ above). The aim is to either destroy the toxic RNA, or stop it interacting with proteins.
One approach is to use small pieces of genetic material called ‘antisense oligonucleotides’ (AONs) which bind to the toxic RNA and destroy it and/or stop it interacting with proteins. AONs have been shown to reverse some of the symptoms of myotonic dystrophy in a mouse model of myotonic dystrophy. The AONs are similar to those currently being tested in clinical trials for Duchenne muscular dystrophy (a therapy known as exon skipping) and spinal muscular atrophy. In the case of myotonic dystrophy the AONs will act in a different way but it is encouraging that the results of clinical trials of AONs for other conditions are looking promising and importantly the AONs appear to be safe.
ISIS Pharmaceuticals is currently testing an AON drug called ISIS-DMPKRx for myotonic dystrophy. Testing is in the early stages of clinical trial and updates can be found on the ISIS website
Scientists have also been searching for other types of molecules that could disrupt the interaction between the toxic RNA and proteins. In 2011 researchers in Spain showed that small pieces of protein which are called ‘peptides’ were effective in a mouse model of myotonic dystrophy.
Researchers in the US have also had success with ‘small molecules’. Most of the drugs currently on the market are considered ‘small molecules’ so this strategy may result in a drug that is cheaper and easier to make (than AONs or peptides), and which may get into targeted tissues more easily. Small molecules can also be modified so that they can be taken as oral drugs rather than being injected. The researchers have screened large collections of potential drugs – modified versions of known drugs like antibiotics for example – and found those that are effective against the toxic RNA. One new compound, known as 2H-4-CA, is the most potent compound known to date that improves signs of myotonic dystrophy in cells grown in the laboratory. The next step will be to test this compound in an animal model of myotonic dystrophy.
Scientists are gradually learning more about the genetic defect that causes myotonic dystrophy type 2 (DM2). In recent years this has allowed the design of drug candidates with potential to treat the condition which are proving effective in models in the laboratory. Further testing will be required before proceeding to a clinical trial. It is also expected that at least some of the research that is initially focusing on type 1 myotonic dystrophy could be modified and applied to DM2 if successful.
A major hurdle for any therapy for myotonic dystrophy will be to deliver the drug as widely throughout the body as possible. This will be necessary to treat the wide range of symptoms that affect many different parts of the body including the muscles, heart, eyes and brain.
We don’t know yet what approach is most likely to result in an effective, safe treatment, but it is promising that several lines of attack are coming forward.
NOTE: Research is moving forward at a fast pace, so this research summary may not be up-to-date at the time of reading.