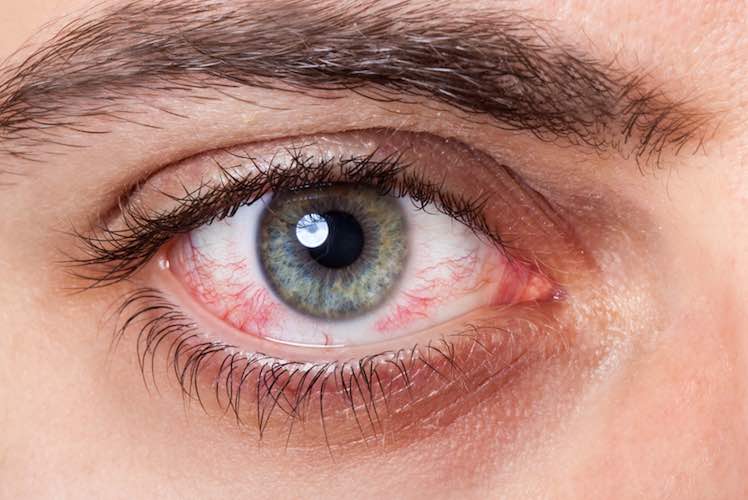
‘Red eye’ is a term used when irritation or infection causes dilated blood vessels on the surface of the eye.
Symptoms
The eye is red, and may be itchy, watery and feel gritty. Vision may be blurred.
Causes
Infection. When a bacterial infection causes the eye to look red, there is usually a thicker discharge and a ‘gritty’ feeling in the eye. A viral infection causes a watery discharge.
Allergy such as hayfever. An allergy results in bloodshot, glazed eyes that are watery and very itchy. The surrounding area may be puffy or there may be dark circles under the eyes.
Sensitivity or allergy to eye drops.
Conjunctivitis. Inflammation of the conjunctiva (the thin layer of tissue covering the eye) causes the blood vessels to swell, and the eye becomes bloodshot.
Burst blood vessel. A blood vessel can rupture on the eye surface after coughing, or spontaneously rupture.
Irritation, such as caused by smoke, dust, eye make-up, or computer screens.
Inflammatory condition. Rarely, red eye may be a result of an inflammatory condition such as iritis or uveitis, which can be caused by problems with the immune system. Iritis may be accompanied by sensitivity to light, blurred vision and headache.
Acute glaucoma. This is an emergency that can result in loss of vision. It occurs when pressure inside your eye rises suddenly. The eye will usuallly be severely red and painful. You may have visual disturbances, such as seeing halos around lights. You need to go to your doctor or ophthalmologist immediately, so you can be treated straighaway.
Corneal ulcer. An ulcer on the clear layer at the front of your eyeball causes the eye to become red and light sensitive. It may feel like something’s in your eye.
Blepharitis.
‘Dry eye’, which is common in the elderly and may be caused by some medicines, may also redden the eyes but requires different treatment to ‘red eye’.
When should you seek medical advice?
You should seek medical advice urgently if:
- the discharge from your eye is thick;
- your eyelids are stuck together on waking;
- you can’t open your eye or keep it open;
- you have a change in vision, or your vision is blurred;
- there is a foreign object in your eye;
- you have been working with metal shavings or wood turning;
- you see a halo effect around lights;
- you have photophobia — pain or discomfort on looking at bright lights;
- your pupils are different sizes or irregular;
- there is swelling around your eye or the lower lid;
- redness or tenderness extends from the eye to the surrounding tissues;
- you experience pain or a feeling of tension in or around your eyes;
- the ‘red eye’ has lasted more than 5-7 days;
- there is a coexisting eye problem such as glaucoma, or ‘dry eye’ in the elderly;
- you have an auto-immune condition such as rheumatoid arthritis or inflammatory bowel disease; or
- you have ‘tired’ eyes, but do not have the accompanying signs of ‘red eye’ (this could be eye strain and requires eye tests).
Self-care
You should try to avoid substances that irritate your eyes, such as smoke, dust, cosmetics and chlorine in swimming pools, if these are known aggravating factors.
Treatment
The treatment your doctor prescribes will depend on what is causing the problem. For example, an allergy may respond to antihistamine eye drops. Soothing eye drops and eye ointments or gels may help.
You should discard all drops, solutions and ointments about one month after opening. However, unit (single) dose lubricant eye drop packs remain sterile until opened, if used within the expiry date printed on the packet.
You should also remove your contact lenses before using some types of eye drops (follow the manufacturer’s instructions or check with your pharmacist), and should not wear contact lenses at all if an eye infection is present. Some drops contain medicines or preservatives that will damage contact lenses.