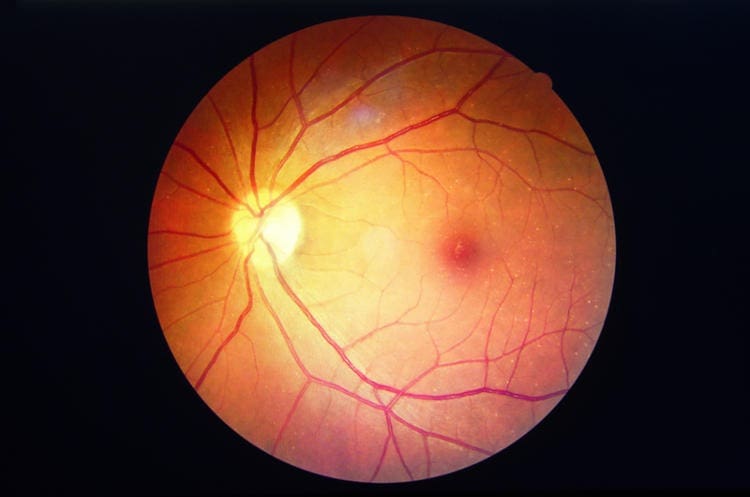
Diabetic retinopathy is one of the most common complications of diabetes. It can develop in people with both type 1 and type 2 diabetes, and usually affects both eyes. People with retinopathy have damaged blood vessels in their retina – the light-sensitive layer at the back of the eyes.
Diabetic retinopathy develops slowly over many years, so regular eye checks are important if you have diabetes. Keeping good control of your blood sugar levels can help prevent retinopathy or slow down its progression. But if you do develop retinopathy, there are treatments available to help improve your vision.
Symptoms
During the early stages of diabetic retinopathy, there are often no symptoms.
As diabetic retinopathy becomes more advanced, you may gradually start to experience several symptoms. Your vision may become blurred, distorted or patchy. You may also have reduced colour vision or have shapes floating in your field of vision (floaters). These vision problems can’t be corrected with prescription glasses.
See your doctor straight away if you have any sudden changes in your vision, such as blurry, spotty or hazy vision. You should seek urgent medical attention if you suddenly cannot see from one or both eyes – you may need to have emergency treatment. Permanent loss of vision (blindness) is rare in people with diabetic retinopathy.
Cause of retinopathy
Having raised blood sugar levels over many years can damage the blood vessels in your body, including the small blood vessels in your eyes. There are 2 main forms of diabetic retinopathy – non-proliferative and proliferative.

Non-proliferative diabetic retinopathy
In non-proliferative diabetic retinopathy, the following changes can develop in the eyes.
- The walls of blood vessels in the retina can become thin and bulge outwards, forming tiny aneurysms (microaneurysms).
- Blood vessels can start to leak fluid and bleed into the retina.
- The blood vessels in the retina may start to become distorted and blocked, starving areas of the retina of oxygen and nutrients.
The above changes on their own do not usually affect eyesight.
Proliferative diabetic retinopathy
Proliferative diabetic retinopathy is more severe and can affect or threaten your vision.
In this advanced stage, the reduced blood supply to the retina stimulates the growth of new blood vessels, which grow across the retina and into the middle of the eye. These blood vessels are abnormal and extremely fragile. They leak fluid and bleed, which can lead to the formation of scar tissue.
Several complications can then develop, including:
- bleeding into the jelly-like substance in the middle of your eye (vitreous humour) – this is called a vitreous haemorrhage; and
- retinal detachment (where the retina is pulled away from where it is normally attached to the inside of the eye), which can happen if scar tissue pulls on the retina.
These complications can cause serious problems with vision, and even a sudden loss of vision in one eye. Sudden loss of vision is an emergency and you should seek medical help immediately.
Macular oedema
At any stage of retinopathy, the retina and its nerve fibres can become swollen with fluid. This is called macular oedema when it involves the central part of the retina (the macula).
The macula is responsible for sharp, straight ahead vision used for tasks such as reading and driving. Macular oedema is the most common cause of vision loss among people with diabetic retinopathy.
Who is at risk of diabetic retinopathy?
The risk of retinopathy increases the longer you’ve had diabetes. In fact, almost all people with diabetes develop some degree of retinopathy eventually.
Other factors that further increase your risk include:
- having had diabetes for longer than 10 years;
- poorly controlled diabetes;
- having high blood pressure;
- high cholesterol levels;
- having a family history of severe diabetic retinopathy;
- also having diabetic kidney disease; and
- being an Indigenous Australian.
Regular eye checks
People with diabetes should have regular eye checks, even when they have no symptoms. Regular eye checks are important to diagnose diabetic retinopathy and other eye conditions related to diabetes as early as possible, before symptoms develop.
Eye checks involve testing your vision plus looking inside your eyes and taking photographs of the retina.
People with type 1 diabetes should start having eye checks within 2 years of diagnosis (starting at age 9) and then once every 1-2 years.
People with type 2 diabetes should have an eye check when first diagnosed and then at least once every 2 years. Those at increased risk of retinopathy (see above) should have eye checks at least once a year.
If you’ve been diagnosed with retinopathy, you’ll need to have more regular eye checks. Women with diabetes who become pregnant also usually need more frequent eye checks than usual, as changes can happen more quickly during pregnancy.
Diagnosis and tests
People who notice a change in their vision should see their doctor (GP) or optometrist (a health professional involved exclusively in eye care) as soon as possible. They will ask you about your vision and do an eye test to check your eyesight.
Your doctor or optometrist will also want to examine the inside of your eye with an ophthalmoscope – a special instrument used to view the back of your eyes. Before using the ophthalmoscope they may give you some eye drops to dilate (open up) your pupil, so that they can get a better view.
Digital retinal photography – a newer imaging option – provides a permanent image of the retina for later comparison. It can be done by ophthalmologists, optometrists and GPs who have been trained in its use.
People with diabetes also have a higher risk of developing cataracts (cloudiness in the lens of the eye which leads to vision loss), and glaucoma (a condition where increased pressure within the eye causes impaired vision or even blindness). So, your doctor or optometrist will also check for signs of these conditions during your eye examination.
You may be referred to an ophthalmologist – a doctor who specialises in treating eye conditions – to monitor and treat diabetic retinopathy, especially if it is advanced.
Features of diabetic retinopathy
Features that can be seen with an ophthalmoscope or retinal photography that help diagnose diabetic retinopathy include the following.
- Microaneurysms, which are usually the first abnormalities to be noticed in people with diabetic retinopathy.
- Haemorrhages (bleeds), in the retina which may be described as dot, blot (round-shaped) or flame-shaped, depending on the level of the retina where they occur.
- Hard exudates, caused by the leakage of fluid rich in fat and protein, vary in size from tiny specks to large patches; and soft exudates, often called cotton wool spots.
- Neovascularisation – the development of new tiny blood vessels across the retina.
- Swelling (oedema) of the retina, which may include macular oedema.
Treatment for diabetic retinopathy
There are several treatments that can help improve retinopathy, slow down its progression and prevent further loss of vision. But while there are effective treatments, there is no cure for diabetic retinopathy, and restoring vision that has already been lost is not always possible.
Controlling your diabetes plus regular monitoring of your condition is usually all that’s needed for early or mild diabetic retinopathy.
Controlling your blood glucose levels and keeping your blood pressure and cholesterol levels in the normal range is very important. That’s because it can slow down or even stop the progression of retinopathy and help preserve your vision. Lifestyle adjustments and medicines are usually recommended in combination to control diabetes, blood pressure and cholesterol levels.
Treatment is needed if you develop retinopathy that’s affecting your eyesight or it becomes severe enough to threaten your vision. Your doctor will recommend you have treatment with one, or a combination, of the following treatments. You should discuss the risks and benefits of these therapies with your ophthalmologist (eye doctor).
Medicines
There are medicines that can be injected into the middle of the eye (intravitreal injections) to treat diabetic retinopathy.
Anti-vascular endothelial growth factor (anti-VEGF) medicines can reduce fluid build-up in the retina and treat macular oedema (swelling). They can also help stop and reverse the growth of new, abnormal blood vessels on the retina. Examples include ranibizumab (brand name Lucentis) and aflibercept (brand name Eylea). The injections are done using a very fine needle under local anaesthetic. These injections may improve your vision and help prevent eyesight problems in the future.
Corticosteroids can be injected or an implant can be inserted into the eye to help treat macular oedema.
Fenofibrate (brand name Lipidil), a medicine also used to treat high cholesterol, can help reduce the progression of retinopathy in people with type 2 diabetes. The medicine is taken as tablets.
Laser therapy
There are 2 different types of laser treatment for diabetic retinopathy, which are normally done under local anaesthetic.
Focal macular laser treatment can be used to stop blood vessels from leaking fluid and blood into the eye. The laser is focussed on leaky vessels near the macula (central area of the retina) to help reduce fluid build-up (oedema) and treat macular oedema.
Panretinal photocoagulation (scatter laser treatment) shrinks abnormal new blood vessels that have formed on the retina in proliferative diabetic retinopathy. The laser is directed more generally at the retina, away from the macula and helps to preserve central vision.
Laser treatment can help stop your vision deteriorating, but often cannot improve vision or restore vision that is already lost.
Surgery
A type of surgery called vitrectomy is sometimes needed for advanced retinopathy where there has been bleeding into the vitreous humour of the eye. It involves removing the blood. In some cases, scar tissue that may be pulling on your retina is removed. This surgery can be done under local anaesthetic with sedation or general anaesthetic.
Preventing diabetic retinopathy
If you have diabetes, the best thing you can do to help prevent the development of retinopathy is to have consistently good control of your blood sugar levels. Your doctor can advise you on the best way to do this.
Your doctor will also recommend that you have regular eye health checks, so that if retinopathy does start to develop it will be detected early and can be treated sooner. Early treatment can help protect your vision.
Support
If you have a visual impairment, your optometrist or doctor can suggest visual aids and other supports to help you with daily living.
Talking to people in a support group can also help, whether you have problems with your eyesight or have diabetes and are worried about the prospect of losing your vision. Having diabetes can sometimes feel like a daily struggle to keep on top of your health needs, but you are not alone – diabetes affects many Australians, and there is lots of support available.
Ask your doctor, diabetes educator or search the internet to find out about local support services. Talking to both health professionals and fellow patients can help you understand more about your condition and the best ways to live with it.