Introduction
This booklet aims to answer many of the questions that people have when they find out that they or their children have spina bifida occulta. Many people are worried by the term spina bifida occulta, yet in the majority of cases spina bifida occulta will cause no problems.
The term spina bifida occulta covers two different conditions and this can be very confusing. One of them is relatively harmless and common – an anatomical anomaly rather than a medical condition. The other condition is much less common but it can cause significant problems. It is similar to a mild form of spina bifida.
This booklet has been written for two groups of people. The first group are those with the common harmless type and the message for them is that they have little need to be concerned about it. The second group are those few people who do have the mild form of spina bifida and the bulk of the information in this booklet is for them.
What is spina bifida occulta?
Spina bifida is Latin for split spine and occulta means hidden. So spina bifida occulta is a split in the spine hidden by skin. What this means is that at least one vertebra is malformed or has not developed fully. Nobody knows for sure but it is assumed that spina bifida occulta develops in a similar way to spina bifida.
The development of spina bifida
Spina bifida is one of a group of conditions called neural tube defects. About half of the foetuses affected by a neural tube defect have spina bifida.
The neural tube is that part of the very young foetus which later develops into the central nervous system and the structures surrounding it. It comprises the brain and spinal cord, their three layers of lining called the meninges as well as the vertebrae (backbone) and skull.
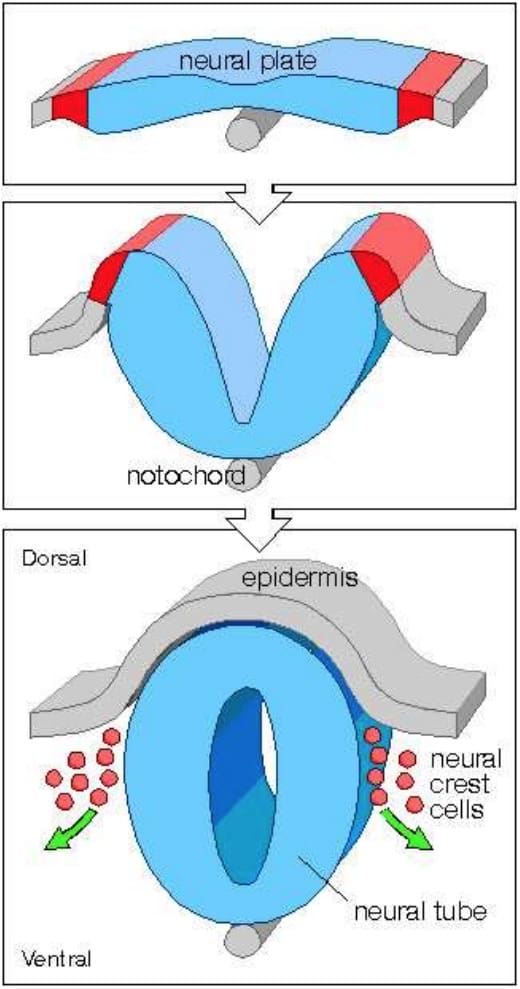
Around the third week of pregnancy a flat sheet of cells called the neural plate starts to change shape and forms a groove. The process continues until a tube is formed. This tube is called the neural tube.
If the process does not complete and an opening is left somewhere along the length of the neural tube then the result is what is called a neural tube defect.
If the opening is in the top part of the tube which later forms the brain and skull, the defect is called anencephaly and it is always fatal.
If the opening is in the bottom part of the tube the defect is spina bifida. Because the bottom part of the neural tube develops into the spinal cord, meninges (linings) and vertebrae, any or all of these structures can be involved in the spina bifida.
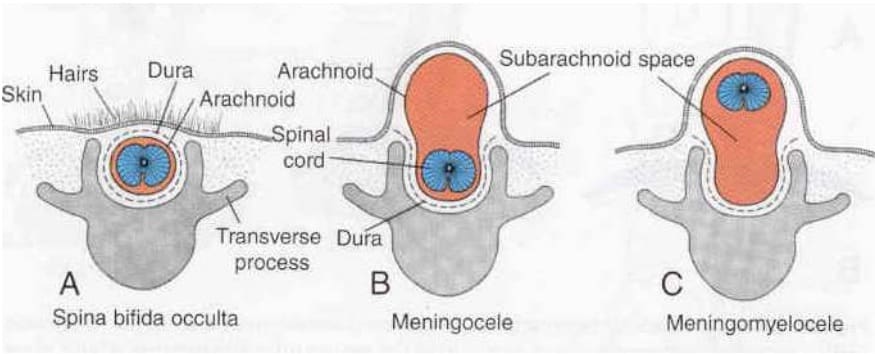
Where the spinal cord and meninges (linings) protrude into a sac on the back which is exposed, it is called meningomyelocele or sometimes myelomeningocoele. Where the meninges, but not the spinal cord, protrude through the opening in the vertebrae into an exposed sac, the condition is called meningocele. The sac is exposed (not covered by skin) when the baby is born so these forms of spina bifida are very obvious at birth. They are also usually detected by ultrasound when scans are taken in the 18th week of pregnancy.
Where there is no exposed sac and the lesion is covered by skin the condition is called spina bifida occulta. The spinal cord and meninges are usually not affected. However the skin may show some unusual signs of underlying problems and this will be discussed later. Spina bifida occulta almost always occurs at the bottom of the spine – in the lumbar or sacral area.
Spina bifida occulta – the common form
Spina bifida occulta where the spinal cord or meninges are not involved is quite common. A few recent medical studies show that about 22% of people have it. In this form of spina bifida occulta it is usually only one vertebra which has not formed completely and the opening is usually very narrow.
In theory, because the spinal cord and meninges are not involved in any way, this form of spina bifida should cause no problems. However, there is some medical evidence that older children with urinary problems and adults with spondylolysis are over-represented in the group of people with this type of spina bifida occulta. Spondyloysis is a crack or stress fracture of the back part of one of the vertebra and it is reasonably common.
The association between spina bifida occulta and these conditions does not necessarily mean that the spina bifida occulta causes urinary problems or spondylolysis. It might mean that some of the things which caused the neural tube to not close fully have also caused other things to happen and these have led to the other conditions. This is one of the areas regarding spina bifida occulta that medical research has yet to provide an answer.
Spina bifida occulta – a mild spina bifida
This type of spina bifida occulta (SBO) is sometimes called occult spinal dysraphism or closed spina bifida. For clarity, this type will be referred to as occult spinal dysraphism or OSD from this point on in this booklet.
OSD differs from the common type of SBO in that the spinal nerves and or meninges are mixed up in some way with their surrounding structures and this involvement causes complications. Unfortunately, it is not always easy to say with any certainty which type a person has. There seems to be a range of lesions with very obvious cases of harmless SBO at one end and very obvious cases of OSD at the other and a grey area in the middle. While MRI technology has gone a long way to shed light on what is happening at the site, it seems that there are a number of people with no apparent involvement of nerve tissue who do have complications.
While SBO is very common, there are much fewer people who have OSD. Estimations of the incidence vary from 1 in 250 to 1 in 5,000 of the general population. However, these figures may change as medical technology improves and the ability to detect what is happening at the lesion site improves. The condition may also be undiagnosed in many people. The incidence of OSD may be found to be similar to the incidence of spina bifida in the way that it varies from one geographic area to another and from one racial group to another. It is usually just one vertebra that is involved with the common SBO and if there are more involved then the diagnosis is more likely to be OSD. Apart from the size of the defect and the number of vertebrae involved, there can be some telltale signs on the skin which are visible at birth which might give a clue that something unusual is going on underneath.
As many as 80% of people with OSD have at least one of these outward signs or herald marks. The signs include:
- A hairy patch in the middle of the lower back
- A fatty lump over the bottom of the spine
- A stork bite or haemangioma (a reddish or purple spot) on the skin
- A dimple or sinus (hole) above the level of the crease in the buttocks (Dimples below the level of the crease are common in newborns and are usually no cause for alarm)
- A pigmented area or birthmark over the bottom of the spine.
- A small tail
OSD can be very complex because it is not just one condition. It represents a number of conditions which can occur separately or in combination. Some of these conditions are:
- A tethered spinal cord where the lower end of the spinal cord is stuck or attached to surrounding bone or other structures. The spinal cord is usually free (to some extent) to move up and down within the spinal canal.
- A lipoma which is a fatty lump whose tissues are often interwoven with those of the spinal cord, making them very difficult to separate. Lipomas can also tether the spinal cord.
- Diastematomyelia where the spinal cord is split in two usually by a piece of abnormal bone or cartilage. This can also tether the spinal cord.
- A dermal sinus which is a connection between the spinal canal and the skin of the back.
All of these conditions can affect the functioning of the spinal cord i.e. its ability to send messages to and from the brain. The cord can become stretched which causes pain and the blood supply to the cells in the spinal cord can be affected with the result that the nerves lose their ability to function properly.
Complications of OSD
Not everyone with OSD will have complications. Sometimes the onset of signs and symptoms will be so gradual that they may not appear until adulthood. For most though, there will be some indications early in the person’s life that the nerves in the spine are not working as they should.
Some of these are:
- Foot deformity
- Weakness in the legs
- Reduced feeling or numbness in the legs or feet
- Back or leg pain
- Bladder infections
- Bladder incontinence
- Constipation
- Scoliosis or other orthopaedic deformities.
All of these symptoms can be caused by conditions other than OSD so it is important to see your doctor for thorough testing and an accurate diagnosis.
It is especially important to seek medical advice where the symptoms are progressing or getting worse. These changes may indicate that the spinal cord is tethered and an operation to untether the cord might be required.
Medical treatment
If is felt that medical intervention is required then treatment may involve untethering of the spinal cord. This procedure is performed by a neurosurgeon.
Because of the way that the nerves are arranged in the lower spinal cord, it is very complex surgery and there is always a risk that some nerves or the spinal cord itself may be damaged. Because of this risk and the fact that there is no guarantee that the operation will be successful in removing the symptoms or even reducing them, many neurosurgeons will wait until the symptoms become relatively serious before operating. On the other hand some neurosurgeons will operate early to try to prevent symptoms from progressing. At the moment there does not seem to be any clear evidence that one approach is better than the other.
Depending on the type or severity of complications, it may be necessary to be treated by another specialist such as a urologist or orthopaedic surgeon.
The procedure to untether the spinal cord creates s car tissue at the site which increases the risk for further tethering. There are a number of ways neurosurgeons try to avoid this, but it is a complicating factor that you and your neurosurgeon must take into consideration.
Genetics
Spina bifida is caused by both environmental and genetic factors. Even though 9 out of 10 children with spina bifida are born to parents with no family history of spina bifida, there is a higher risk of a pregnancy being affected by a neural tube defect (anencephaly or spina bifida) where there is a family history. The risk is higher when the family relationship is closer. The same seems to be true for OSD.
In a family where one child has some form of OSD, any future children seem to have a similar risk (3.5%) of developing a neural tube defect. It is not clear whether the risk is only for OSD or any type of neural tube defect.
Prevention
It has been known for a few decades that folic acid (a B vitamin) when taken for a month prior to conception and for 3 months afterwards can reduce the risk of the baby developing a neural tube defect by up to 70%. For women with no family history of a neural tube defect the recommended dose is 500 micrograms (or .5 milligrams) a day. For women with a family history, including them or their partner, the recommended dose is 4 milligrams a day. In Australia the inexpensive tablet, Megafol, contains 5 milligrams of folic acid and is available from chemists.
Since September 2009 bread making flour in Australia has been fortified with folic acid to reduce the incidence of neural tube defects. Folic acid (called folate in its natural form) is available naturally in leafy green vegetables and some other foods. The levels consumed naturally do not always reach the recommended level for lowering the risk of a neural tube defect – affected pregnancy, so it is important for women of child bearing age to take a daily folic acid supplement.
Because about half of all pregnancies in Australia are unplanned, the recommendation is for all women of child bearing age to supplement their diet with a folic acid tablet. Further information on folic acid is available from SBH Queensland.
Genetic Counselling
Genetic counselling provides diagnosis and counselling for people with an inherited condition in the family. Queensland Health provides a free service at the Royal Children’s, Logan and Princess Alexandra Hospitals and regional centres through Genetic Health Queensland. Referral from a GP is required to access the service.





