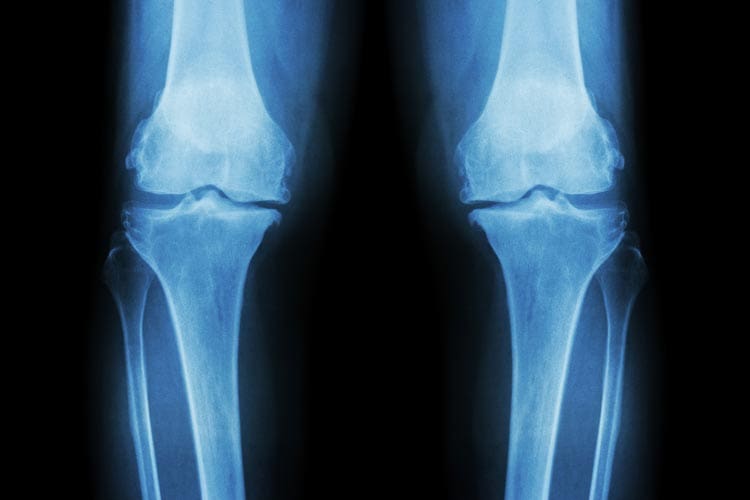
Osteoarthritis affects most of the structures of a joint – not just the cartilage.
A joint is where 2 or more bones meet. The ends of the bones are covered by a hard slippery substance called cartilage. Cartilage acts as a ‘shock absorber’ and allows the bones it covers to glide over each other smoothly.
Osteoarthritis used to be blamed on simple wear and tear of the joints. It was thought to be mostly due to changes in the cartilage. But while the loss of cartilage is a major part of the process, other parts of the joint are affected and involved in osteoarthritis.
Osteoarthritis is the most common form of arthritis – and is characterised by joint pain and stiffness. Osteoarthritis most commonly affects the joints of the hands, neck, lower back, knees and hips.
Changes to the joint in osteoarthritis
These are some of the changes that occur in joints affected by osteoarthritis.
Cartilage deteriorates and is lost. Loss of cartilage that cushions the ends of your bones is a major feature of joints affected by osteoarthritis.
The structure and composition of the cartilage also change at a microscopic level, so that it becomes less resilient.
The cartilage becomes roughened and pitted. It thins and develops tiny cracks. This process deprives the bones of their normal cushioning.
Thickening of sub-chondral bone. Bones affected by osteoarthritis become denser just below the cartilage (known as sub-chondral bone). It is still not entirely clear whether the thickening of the sub-chondral bone is in response to the loss of cartilage, or whether it happens before the cartilage starts to wear away. Some evidence suggests that the changes in sub-chondral bone occur before the changes to the cartilage.
Bone spurs (or osteophytes) are small smooth outgrowths of bone that form at the edges of bone near joints.
A defective repair process can cause these bone spurs to develop over time at the ends of the bones. The bone can also form cysts or develop tiny fractures. Many bone spurs don’t cause any pain, but some do and may result in a loss of range of motion in a joint. Bone spurs may cause a knobbly appearance in the finger joints.
Synovitis is inflammation of the synovium (synovial membrane). The synovium is the inside lining of the joint capsule of a synovial joint. Synovial joints are the most common joint in the body.
Osteoarthritis is not typically thought of as an inflammatory process (like rheumatoid arthritis), but inflammation occurs in the synovium of the majority of people affected by osteoarthritis. Again, these changes may occur before any changes to the cartilage are seen.
Many scientists believe that tiny pieces of cartilage that fall off as the cartilage degrades can aggravate the synovium and increase the release of inflammatory chemicals into the joint.
Synovitis is related to pain in osteoarthritis.
Thickened joint capsule. The joint capsule seals the synovial fluid in synovial joints and provides some stability by limiting movement of the joint. In osteoarthritis, the joint capsule may slowly thicken as it tries to stabilise the changing joint.
Increased synovial fluid. Osteoarthritis can cause an increase in synovial fluid in the joint. This joint effusion happens commonly in the knee and is sometimes known colloquially as ‘water on the knee’. The build-up of fluid can cause pain and stiffness in the knee, making it difficult to bend your leg. It may also be difficult to weight-bear. The knee may appear swollen and puffy.
Loss of joint space. The body tries to repair the damage, but the cartilage is broken down faster than it can build up. In severe cases, cartilage completely disappears in some places. This puts the bones in direct contact with each other with no cartilage to absorb the pressure. This is known as joint space narrowing or loss of joint space. Cartilage can’t be seen on X-ray, but doctors can see if the joint space has narrowed.
What causes pain in osteoarthritis?
Because cartilage has no blood supply or nerves, it is not the source of pain in osteoarthritis.
Pain in osteoarthritis is thought to be caused by many factors, including:
- tiny pieces of bone or cartilage breaking off and floating inside the synovial cavity
- inflammation of the synovial membrane
- joint effusion (excess fluid in the joint)
- increased pressure and tiny fractures in the bones
- bone spurs (but not always)
- loss of joint space (bone rubbing on bone)
- tendons and ligaments stretching.
Osteoarthritis affects people in different ways. Some people have very few symptoms, while others experience considerable pain and disability.
Osteoarthritis of the knee joint
In osteoarthritis of the knee joint, these processes result in reduced protective cartilage, a narrowing of the joint space, and sometimes bone spurs.
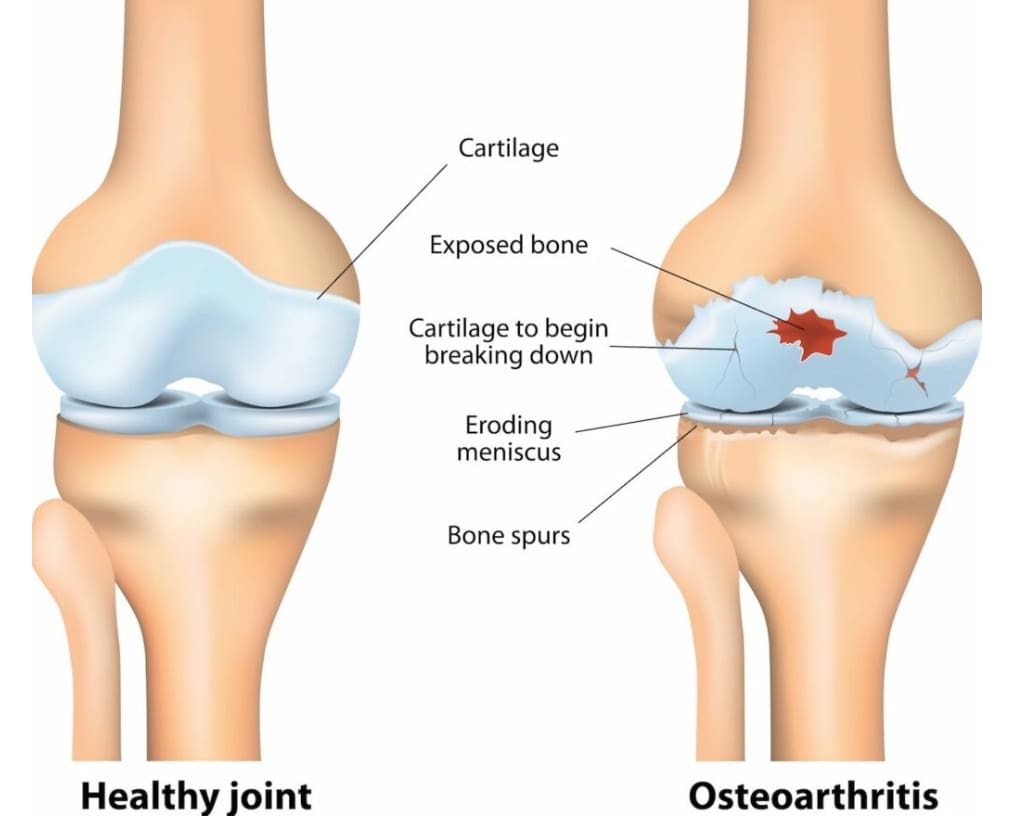
Image: What happens in your knee joint when you have osteoarthritis of the knee
Osteoarthritis of the spine
In osteoarthritis of the spine, the disks between the vertebrae of the neck or lower back become narrowed. Bone spurs (projections that form along edges of bone) may occur. The bone spurs may be painless, but sometimes they can pinch the nerve roots in your spine, causing weakness in an arm or leg.
Osteoarthritis of the hip joint
In osteoarthritis of the hip joint, the cartilage gradually wears away decreasing the joint space between the bones. Bone spurs may also occur in the hip joint.