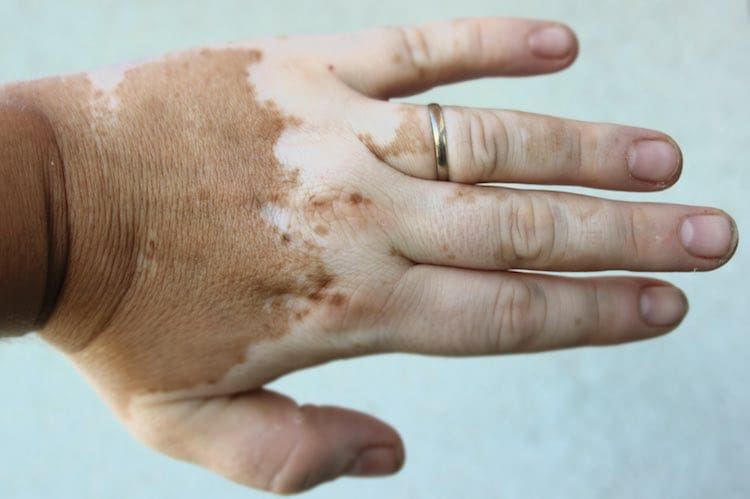
What is vitiligo?
Vitiligo is a skin pigmentation disorder that is characterised by smooth, white, painless spots or patches on various parts of the body. Hair in the affected areas may also turn white.
The white areas arise due to loss of the pigment (melanin) that gives the skin its colour and protects it from the sun’s ultraviolet (UV) rays. Melanin is normally produced by skin cells called melanocytes.
Vitiligo is not contagious. It is a common condition that affects about 1 per cent of people worldwide. Vitiligo can affect people of all ages, but often starts between the ages of 10 and 30 years. Vitiligo generally affects both men and women equally.
Symptoms
Vitiligo is first noticed with the appearance of flat white spots or patches on the skin. The white patches are more commonly seen in areas that are exposed to the sun, such as the hands, arms, face and lips. However, vitiligo may occur in other areas such as the armpits, groin, mouth, eyes, nose, nostrils, navel area and the genitals.
In addition, some people will notice white patches appearing inside their mouth and may have premature greying of the scalp hair, eyelashes, eyebrows or beard.
There is no way to tell if the condition will spread from the original site; however, generally other patches will appear on other parts of the body. This may occur slowly, but for some people it happens rapidly. Factors such as stress, physical illness, pregnancy and severe sunburn may trigger a worsening of vitiligo.
People with vitiligo may find that the white patches sometimes stop forming without any treatment. The white patches may revert to normal skin colour; however, this is rare and does not usually happen to all affected areas.
What causes vitiligo?
The cause of vitiligo is not fully known but there are a number of theories and research is continuing.
One theory suggests that people who develop vitiligo may produce antibodies which destroy the melanocytes, the cells that produce melanin in the skin.
Another theory suggests that the melanocytes attack and destroy themselves.
It has also been suggested that some cases of vitiligo may occur after severe sunburn or an episode of emotional distress.
In some cases, vitiligo is associated with autoimmune disorders — conditions in which your immune system attacks your own tissues.
Autoimmune disorders that have been linked with vitiligo include:
- thyroid disorders;
- Addison’s disease ( a disease of the adrenal glands leading to insufficient production of corticosteroid hormones);
- alopecia areata (patches of baldness);
- pernicious anaemia (a decrease in red blood cells due to the body not being able to absorb vitamin B12 from food); and
- diabetes mellitus.
In some cases vitiligo seems to be inherited and run in families, with children whose parents have vitiligo being at increased risk of developing the condition themselves.
How is vitiligo diagnosed?
Your doctor will use a number of methods to diagnose vitiligo and check for the conditions associated with it. These include the following.
- Checking for a family history of vitiligo.
- Identifying previous trauma to the site (such as sunburn).
- Checking if you or a family member has an autoimmune disease.
- Doing a thorough skin examination.
- Performing tests such as a biopsy of the affected skin (taking a small sample of skin to examine in the laboratory) and blood tests.
- Occasionally, doing an eye examination for uveitis (inflammation of the front portion of the eye).
Treatment for vitiligo
The aim of treating this condition is to improve the skin’s appearance and to stop new patches forming. However, treatment for vitiligo tends to take a long time, and there is no definitive cure.
The most common forms of treatment include:
- corticosteroid creams or ointments;
- tacrolimus – a medicine known as an immunomodulator that can be made into an ointment by pharmacists – may be used to treat facial vitiligo when extended treatment with corticosteroids is unsuitable;
- exposure to a specific wavelength of UVB radiation (narrowband UVB phototherapy);
- treatment with a combination of either topical or oral psoralen and UVA light (photochemotherapy);
- depigmentation (fading the rest of the skin to match the already white areas); and
- surgical procedures including transferring skin from unaffected areas of your body to the areas affected by vitiligo (autologous skin grafts).
In addition, your doctor or dermatologist (skin specialist) may also recommend:
- camouflage measures such as makeup, topical dyes, self-tanning lotions or micropigmentation (tattooing); and
- in some cases, avoiding things that cause excessive friction on the skin, such as jewellery and wrist bands.
In all cases, strict sun protection is important with appropriate SPF 30+ sunscreens, protective clothing, hats and sun avoidance at peak times.
Many people with vitiligo suffer emotional and psychological problems because of the appearance of their skin. It is important to seek out support from your doctor or dermatologist if this is the case as a referral to a psychologist or psychiatrist can be helpful. In addition, there are support groups which can offer help and put you in touch with others who suffer from vitiligo.