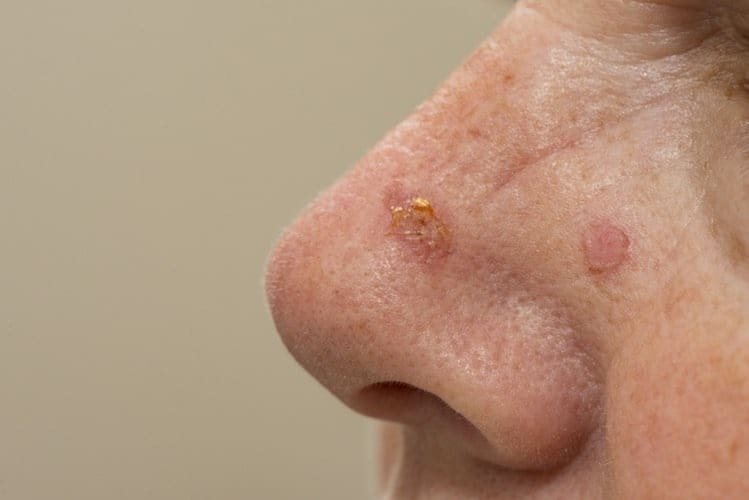
Discussion of skin cancer is usually divided into melanoma (by far the most dangerous form) and the non-melanoma skin cancers, which include basal cell cancers and squamous cell cancers.
The treatment of non-melanoma skin cancer has a high success rate, provided that the skin cancer is detected at an early stage.
Australians should regularly check their skin for new growths, sores that won’t heal, or any changes in the colour, shape or size of existing skin spots. Your doctor can also check for skin cancers.
If you have a history of this condition you should have regular medical checks of the previously treated areas and other areas that are susceptible to new cancers.
Diagnosis of skin cancer
Your doctor will look at the suspect skin lesion (or skin spot) and feel the nearby lymph nodes. If your doctor suspects that you may have a skin cancer, they will suggest a biopsy to confirm the diagnosis. This is a quick and relatively simple procedure carried out with a local anaesthetic. It may be a punch biopsy, where a small sample portion of the skin lesion is collected, or an excision biopsy, where the entire abnormal area is removed.
You may also need additional tests, such as a lymph node biopsy, to show if there has been any spread of the cancer.
Treatment
When planning the treatment, your doctor will take a number of factors into account, including:
- the type and size of the cancer;
- where it is situated; and
- whether it has spread to other parts of the body.
When your doctor knows to what stage the cancer has progressed, they can make a decision on the type of treatment required. The treatment often includes some type of surgical procedure or radiation therapy.
Types of treatment for non-melanoma skin cancer
Surgery
When obtaining a biopsy, often the whole skin cancer is removed, which may be the only treatment necessary. However, in some cases, if the skin cancer is large or spreading, a larger amount of skin may need to be removed and a skin graft may be needed to cover the area.
Mohs’ surgery
A specialised form of skin cancer surgery is called Mohs’ surgery. This method of micrographic surgery can be used to remove large, deep or recurring cancers. It is also used for cancers in areas that are difficult to treat surgically. The process involves methodically removing the visible skin cancer and a thin layer of tissue, staining and cutting the removed tissue into sections and marking on a diagram (Mohs’ map), and then preparing and examining the removed tissue under the microscope (which may take about an hour) to check that the deep ‘roots’ of the cancer have been removed. The process is repeated and continued until the entire cancer has been removed.
Cryotherapy
This technique uses extreme cold to treat pre-cancerous skin conditions and some small skin cancers. Liquid nitrogen is applied to the tumour to freeze and kill abnormal cells. Some pain and redness may occur after the area has thawed, and a blister may develop. A small white scar may remain over the treated area.
Curettage and cautery (also known as diathermy)
This is another form of surgery in which the doctor will numb the area with local anaesthetic and, using a small, sharp, spoon-shaped instrument called a curette, scoop out the diseased area. The doctor will often then use a diathermy instrument to run an electric current into the area to control bleeding and destroy any remaining cancer cells. This technique often leaves a flat, light-coloured scar.
Radiotherapy or radiation therapy
This technique is generally used for cancers that may be hard to treat with surgery (for example, on the eyelids or nose), or if the person is medically unfit for any type of surgery. The treatment uses high-energy X-rays to destroy cancer cells. Several treatments over several weeks are often needed to destroy the cells completely. This type of treatment can make the area red and sore, and can produce changes in skin colour and/or texture in the long term.
Chemotherapy (topical)
In this technique, a medicine is applied directly to a pre-cancerous lesion or sunspot in the form of a cream, for example, fluorouracil (brand name Efudix). The cream is applied twice every day for several weeks, with the area becoming red, followed by blistering, peeling or cracking. However, this reaction is only temporary, and the treated skin will flake away.
Immunomodifiers
Imiquimod is a cream that can be used as a treatment for some skin cancers (usually superficial basal cell carcinoma) and pre-cancerous lesions. It stimulates the immune system to recognise and destroy cancer cells.
Photodynamic laser therapy
Photodynamic laser therapy is the combined use of laser light and medicines to make the cancer cells sensitive to light so they can be destroyed by follow-up laser treatment. This treatment is suitable for pre-cancerous lesions and some superficial skin cancers.
Non-steroidal anti-inflammatory gel
Diclofenac 3% gel (brand name Solaraze 3% Gel) can be used to treat solar keratoses (also called actinic keratoses) — a type of pre-cancerous lesion — but is not a treatment for established skin cancer.
Outlook
Skin cancer treatment has a high success rate if started early. However, people who have been treated for skin cancer at any time have a higher-than-average risk of developing new skin cancers. As such, it is extremely important to continue to examine yourself and to visit your doctor regularly for follow-up checks.
Risk factors for skin cancer in Australia
Australia has the highest incidence of skin cancer in the world. Approximately 2 out of every 3 Australians will be diagnosed with skin cancer before the age of 70 years.
Who is most at risk?
The chance of developing skin cancer depends on a number of factors. A person may be more likely to develop skin cancer if they:
- are mature, as the risk of skin cancer increases with age;
- have fair skin, or skin that burns easily;
- have fair or reddish hair;
- have light-coloured eyes (green or blue);
- have lots of moles;
- have been severely sunburned in the past
- have a personal or family history of skin cancer;
- do not protect their skin from sun exposure;
- work outdoors or spend a lot of time outdoors, unprotected;
- have used solariums, sun lamps or have been sunburned; or
- already have ‘sun spots’ (actinic keratoses / solar keratoses) — flat scaly spots (red or skin-coloured). These are a warning that skin damage has occurred. Some may go on to develop into skin cancers.
Your sun exposure in the first 10 years of your life affects your background risk for getting skin cancer. Every additional decade of high sun exposure after that adds to your cumulative risk. Avoiding sun damage to skin throughout life is an important protection against developing skin cancer.
Solariums
Solariums, sunlamps and sun beds are not safe. Solariums emit ultraviolet (UV) radiation, which causes melanoma and other skin cancers, eye damage and premature ageing of the skin. Commercial solariums are illegal in Australia.
Medical treatments that increase risk of skin cancer
Some medical treatments which use UV radiation may increase the risk of skin cancer. In addition, a number of medicines, including some creams and lotions, and some antibiotics, can make a person more susceptible to skin damage from UV rays. Ask your doctor if any medicines you are prescribed are likely to increase your sensitivity to UV light.
Other risk factors
Some substances are photosensitisers, and exposure to them, for example through your occupation, can make you more sensitive to UV light, and put you at increased risk of skin cancer. Examples include:
- coal tar and derivatives such as creosote;
- dyes such as fluoroscein;
- chlorinated hydrocarbons such as chlorobenzols; and
- some plants such as fennel and some citrus species.
A number of rare hereditary conditions can also lead to an increased risk of skin cancer including xeroderma pigmentosa, a condition in which a person has reduced ability to repair DNA damage, such as that caused by UV radiation.
Early detection
The earlier a skin cancer is detected, the better the chance of successful treatment. Basal cell carcinomas (BCCs), the least dangerous and most common of the skin cancers, are successfully treated in almost all cases. Squamous cell carcinomas (SCCs) — which are not as dangerous as melanoma but can spread to other parts of the body if not treated — are also successfully treated in almost 100 per cent of cases. Melanoma can be fatal, although more than 90 per cent of people who have a melanoma treated will still be alive after 5 years.
Skin cancers usually do not cause discomfort and are best picked up by regularly looking at the skin rather than just by feel. A regular skin self-examination aims to pick up any changes early.
Be on the lookout for:
- any new spot or unusual freckle, mole or sunspot;
- a non-healing or crusty sore;
- a small lump that is red, pale or pearly;
- a spot that looks different from other spots around it;
- a persisting itch in a mole; or
- a spot that has changed colour, size or shape over a few weeks or months.
Consult your doctor if you have any of these signs. Skin cancers that are detected at an early stage are the most easily treated.