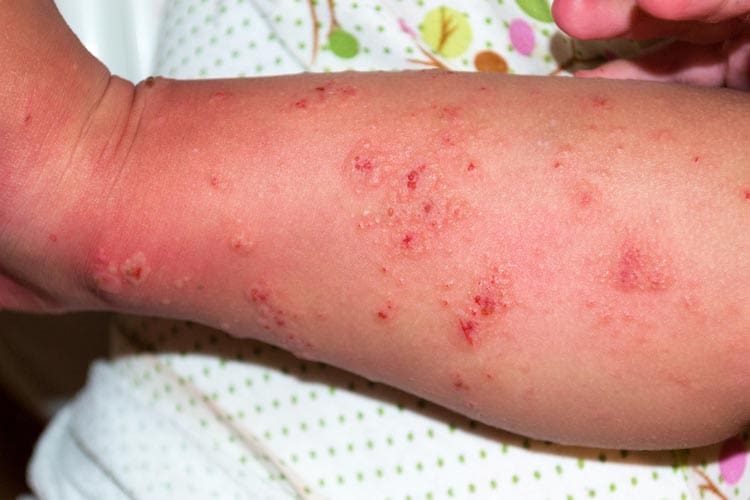
Scabies is an intensely itchy skin condition caused by tiny mites that can be passed from one person to another. The mites that cause scabies, called Sarcoptes scabiei var. hominis (human itch mites), only live on human skin – you cannot catch them from animals.
What are the symptoms of scabies?
The main symptom of scabies is an extremely itchy skin rash. The rash is usually bumpy and looks like pimples or tiny blisters. It can also be scaly. Sometimes you can see wavy lines on the skin where the mites have burrowed into the top layer of the skin.
The itch is often worse at night and is caused by an allergic reaction to the mites. It usually develops about 4-6 weeks after catching scabies, but people who have had scabies in the past tend to develop symptoms within a few days of being reinfested.
The areas of skin that are most commonly affected are the:
- hands, especially between the fingers;
- insides of the wrists;
- inner elbows;
- armpits;
- breasts;
- feet, especially between the toes;
- genitals, especially the penis; and
- groin.
Babies and young children often have scabies on their face, scalp, neck, palms of the hands and soles of the feet. These areas are usually not affected in adults and older children with scabies.
What are Norwegian scabies?
Norwegian scabies, now more commonly known as crusted scabies, is a more severe form of the condition. People with crusted scabies have thousands of mites on their skin, compared with about a dozen mites in regular scabies. Thick crusts of skin contain the mites and their eggs.
Crusted scabies is often not itchy. It is usually seen in older people, people living in nursing homes or care homes, mentally impaired people or in people with problems with their immune systems. People with crusted scabies are highly contagious and can easily pass scabies on to other people.
Who can get scabies?
Anyone can get scabies. Good personal hygiene does not prevent the spread of the scabies mite, and people from all walks of life can be affected.
In most parts of Australia, scabies tends to occur mainly in places where many people live close together, such as residential care homes. Child care centres and schools can also be affected.
There is a higher rate of scabies among people living in tropical areas of Australia, as mites can live longer away from a human host when the weather is warm and humid. Remote Indigenous communities and socioeconomically disadvantaged communities also have higher rates of scabies.
How does scabies spread?
The microscopic mites that cause scabies spread from person-to-person by close skin-to-skin contact. The mites burrow into the top layer of the skin where they live and lay their eggs. When the eggs hatch, the mite larvae make their way to the surface of the skin where they mature and can spread to other areas of the skin or be passed on to other people.
Contact usually needs to be prolonged for you to catch scabies. Brief contact such as a shaking hands does not usually spread scabies, but it is possible to get scabies from holding hands for several minutes. Mites can also spread through clothing or bedding, but this is rare unless the person has crusted scabies.
In general, the main people at risk of catching scabies are those who live in the same household as an affected person. You can also catch scabies from intimate or sexual contact with an infected person.
Can my pet give me scabies?
The scabies mites that affect dogs and cats are not the same species as the mite that affects humans, so your pet can’t give you scabies. Animal mites may cause temporary itching for a few days, but the mite will then die on the human skin.
Complications
People with scabies are at risk of developing bacterial skin infections such as impetigo due to scratching, which causes breaks in the skin where bacteria can enter. Bacterial skin infections need to be treated with antibiotics.
Can you see scabies mites?
Scabies mites are less than half a millimetre long, and because there are usually only a few present on the body at once, you are unlikely to see them.
Tests and diagnosis
Scabies can usually be diagnosed based on your symptoms and a skin examination. To confirm the diagnosis, your doctor will look for tiny, squiggly, raised lines in the skin made when the mite burrows.
It can be difficult to find mite burrows as most people only have about 5-15 mites over their entire body. Your doctor may use a dermatoscope (special instrument with a light and a magnifying lens) to help to find them. If burrows are found, a skin scraping of the area can be taken for examination under a microscope, looking for evidence of mites, mite faeces (droppings) or eggs.
In many cases, the diagnosis of scabies can be simply confirmed when treatment successfully relieves the symptoms.
How is scabies treated?
Treating scabies involves:
- killing the mites with treatments that you apply to the skin and/or medicines that you take by mouth;
- disinfecting clothes, bedding and towels; and
- treating the itch, which can continue even after the mites have been killed.
If you have scabies, everyone you live with should also be treated at the same time. All members of the household should be treated, even if they don’t have any symptoms. That’s because symptoms often take weeks to develop, so family members or others people you live with could be affected without knowing it. Treating the entire household helps prevent re-infestation.
Skin treatments for scabies
Scabies mites can be killed with medicines called scabicides that you apply to the skin. These topical scabies treatments can be purchased from pharmacies in Australia without a prescription.
The first-choice treatment is permethrin 5 per cent cream (e.g. Lyclear Cream). You apply the cream to clean, dry skin. It should be applied over the entire body from the neck down. A nail brush is used to apply the cream under the fingernails and toenails. After applying the treatment, put on clean clothes or pyjamas and make sure you have fresh bed linen. The cream should be left on for at least 8 hours (usually overnight), and then washed off. Make sure you re-apply the cream to your hands if you wash them during the treatment period. Possible side effects include mild stinging or burning when the cream is first applied. The treatment may need to be repeated in 7 days in some cases when symptoms persist.
Benzyl benzoate 25 per cent lotion (e.g. Benzemul, Ascabiol) can also be used to treat scabies, but it is more likely to cause skin irritation than permethrin. It is applied to the skin from the neck down, and left on for 24 hours. It should be diluted with water for use in children. Treatment should be repeated in 7-14 days.
Always read the instructions when using these products and check the directions of use with your pharmacist. Children aged 6 months to 2 years should only be treated with permethrin under medical supervision.
Scabies can affect the skin on the head in some people, including young children, older people and people living in central and northern Australia. In these people, scabies treatment should be applied to the neck, face and scalp, taking care to avoid the areas around the eyes, nose and mouth. Check with your doctor about whether this is necessary. Young children will need to have their hands covered so that they cannot suck them and ingest the medicine.
Oral medicines for scabies
Ivermectin (brand name Stromectol) tablets may be prescribed for people who continue to have scabies after applying topical (skin) treatments, or for people who cannot use topical treatments.
Possible side effects of ivermectin include itching, dizziness, nausea, diarrhoea and tiredness. These side effects are usually mild and short-lived.
Treatments for itching
After treating scabies, the itch often gets worse for a few days. Itching can persist for several weeks, but usually gets better within a month. In the meantime, you can relieve the itching of scabies by using a skin moisturiser or over-the-counter antihistamine medicine taken by mouth. You can also try having cool baths or putting a cool, wet washcloth on itchy areas. Your doctor may prescribe a corticosteroid cream or ointment if you have severe or persistent itching.
Disinfecting clothes and bedding
To kill the scabies mites, bedding, towels and clothes should be washed in hot water and/or dried using a hot setting on a clothes dryer. If clothes cannot be washed or dried on a hot setting, they can be dry-cleaned or ironed with a hot iron.
Alternatively, clothes, sheets and towels can be washed and dried normally and then placed in a plastic bag out of the way for a week, as mites cannot survive longer than 36-72 hours when not in contact with human skin.
Treating crusted scabies
If you have crusted scabies, your doctor may refer you to a dermatologist (skin specialist) or specialist in infectious diseases. Crusted scabies may need to be treated in hospital.
Several doses of ivermectin (Stromectol tablets) are usually needed to treat crusted scabies, as well as repeated topical treatments with permethrin or benzyl benzoate. Additional treatments may also be recommended to treat the skin crusting, or thickening.
You will need to disinfect all clothes, bedding and towels (as described above), but with crusted scabies you should also thoroughly vacuum and clean all furniture, floors and carpets to prevent the spread of scabies and possible reinfestation.
Preventing scabies: how to protect yourself and others
If you have been in contact with someone who has scabies, especially if they have crusted scabies, see your doctor for advice on whether or not you need treatment.
If you live with someone who has been diagnosed with scabies or have had intimate contact with someone with scabies, you should be treated. You should limit contact with other people until you have received treatment.
Children with scabies should be kept home from school or child care, usually until at least a day after treatment has been started. Check with your doctor and your child’s school or child care centre before sending them back.