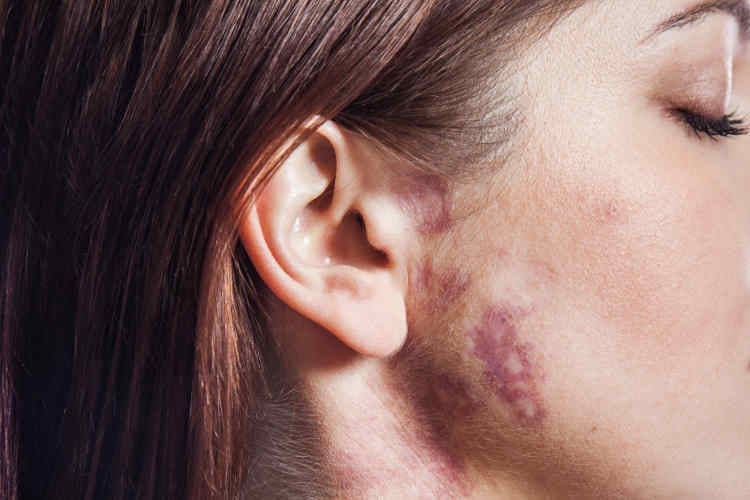
Port wine stains, or capillary vascular malformations, are birthmarks made up of tiny blood vessels. They are relatively common, occurring in 3 out of every 1000 babies. At birth, port wine stains appear pale pink to deep red or purple in colour. They can occur anywhere on the body.
Over the years, these lesions may become raised and thickened, and may bleed easily. They do not grow in size but they do grow proportionally as your child grows. They are not contagious nor can they be inherited.
Port wine stains don’t go away by themselves or decrease in size over time. Because of their appearance, there can be associated emotional, social or psychological problems.
In the majority of cases, port wine stains are not associated with any other abnormality. However, if the birthmark occurs on the face there is a slightly increased possibility of an associated eye or brain abnormality, such as glaucoma or epilepsy. The severity of these abnormalities is not related to the size of the port wine stain.
Regular checks
All children with a facial port wine stain — especially when it involves the eyelid — should be checked regularly by an eye specialist and a paediatrician is also usually involved in the child’s care.
If a child is going to develop epilepsy associated with their port wine stain, the onset will usually occur in the first 2 years of life. These birthmarks are not generally associated with developmental delay in the absence of any other abnormality.
Treatment of port wine stains
The appearance of port wine stains can usually be improved by treatment with a pulsed dye laser. This particular type of laser targets the blood vessels without damaging the overlying skin. About 60 per cent of facial port wine stains have a fairly good response to this treatment. Repeated treatments over many years are often required.
Side effects of laser treatment include temporary bruising, swelling and discomfort. Rarely, laser treatment can result in ulceration and scarring.