Ulcerative colitis is one of 2 major types of inflammatory bowel disease — a condition which causes the bowel (colon) to become inflamed. The other type of inflammatory bowel disease is known as Crohn’s disease.
Inflammatory bowel disease is a totally different condition from irritable bowel syndrome (IBS). In IBS, the functioning of the bowel is affected but there is no inflammation.
Ulcerative colitis and Crohn’s disease are long-term, chronic (ongoing) conditions which can flare up, on and off, throughout life.
What are the symptoms?
Most commonly, the symptoms of ulcerative colitis include:
- abdominal pain, which is often crampy;
- a feeling of urgently needing to open the bowels;
- blood, mucus or pus in the stool;
- diarrhoea;
- fatigue and tiredness;
- weight loss; and
- loss of appetite.
People with ulcerative colitis may also develop other symptoms unrelated to the bowel. These can include:
- mouth ulcers;
- skin problems;
- joint pains;
- eye problems; and
- liver disease.
Sometimes, malabsorption of important nutrients can occur.
Many people with ulcerative colitis feel well most of the time and don’t have any symptoms. This means the disease is not ‘active’ at this time, or can be said to be in remission. When the disease flares up and causes symptoms, this is known as a relapse.
Most of the time a trigger for a relapse can’t be identified, although some people find that stress, infections, some medicines or certain foods can trigger symptoms. It should be remembered that none of these is the cause of the disease itself.
Depending on where the inflammation occurs in the large bowel, ulcerative colitis can also be called:
- proctitis (involving the rectum only);
- proctosigmoiditis, or distal colitis (involving the rectum and sigmoid colon); or
- universal or pan-colitis, which means the entire colon is affected.
Doctors don’t know why some people’s disease spreads to involve their entire colon yet in others the disease is confined to one area of it.
What is the difference between ulcerative colitis and Crohn’s disease?
It can sometimes be difficult to distinguish between ulcerative colitis and Crohn’s disease, particularly in the early stages, because the symptoms are very similar.
The major difference between the 2 include the following.
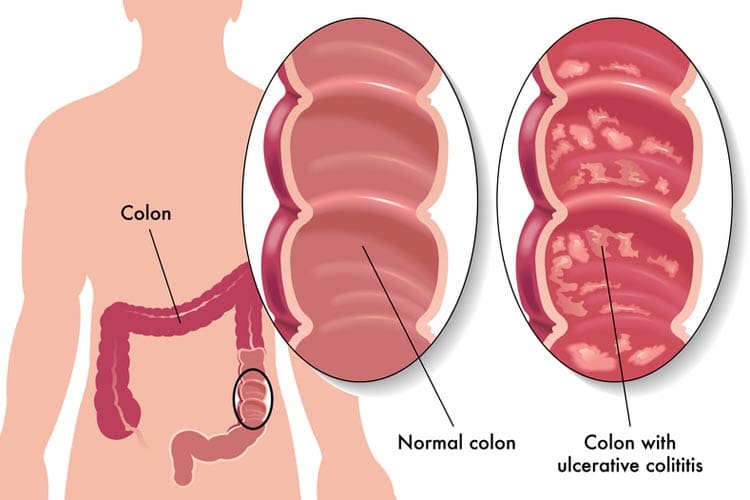
- In ulcerative colitis the inflammation affects only the inner lining of the bowel wall, whereas in Crohn’s disease the inflammation is of the full thickness of the bowel wall.
- The distribution of inflammation geographically within the gastrointestinal tract: ulcerative colitis affects only the large bowel (colon and rectum) and Crohn’s disease can affect any part of the gastrointestinal tract from the mouth to the anus.
- With Crohn’s disease there may be patches of healthy bowel next to patches of the diseased bowel. The inflammation of ulcerative colitis, on the other hand, is a continuous inflammation.
Who gets ulcerative colitis?
Ulcerative colitis affects people of all ages, but usually starts between the ages of 15 and 30 years. There is another (smaller) peak in the diagnosis of this disease between the ages of 50 and 70 years.
Although ulcerative colitis is uncommon in children, it can have more severe effects than in adults if it is not treated, such as delayed or stunted growth.
Having a close family member with ulcerative colitis puts you at increased risk of developing the condition.
What causes ulcerative colitis?
Unfortunately the cause is still unknown despite intensive research. Causative factors that have been suggested include:
- genetic predisposition;
- infectious agents (bacteria and viruses);
- defects in the immune system; and
- environmental factors.
Some doctors suggest a combination of some or all of these factors may be involved. Psychological stress and food allergies are not thought to play a role in the development of the disease.
Diagnosis
Ulcerative colitis is sometimes difficult to diagnose because its symptoms can be similar to other conditions such as bowel infections or irritable bowel syndrome. Most people with suspected ulcerative colitis will need a colonoscopy or sigmoidoscopy to confirm the diagnosis.
Colonoscopy and flexible sigmoidoscopy are endoscopic examinations, in which a thin, flexible tube with a light on it (an endoscope) is passed into the rectum to allow the doctor to view the lining of your bowel. You will be lightly sedated during the procedure. The doctor may take several small pieces of tissue from the lining of your bowel for examination under a microscope. This is called a biopsy.
Blood tests can reveal whether you have anaemia or any vitamin or mineral deficiencies. Blood tests can also confirm that there is inflammation in the body.
Testing of stool samples may also be recommended by your doctor to help make the diagnosis.
Ulcerative colitis treatment
Treatment of ulcerative colitis will depend on the severity of the disease and the effect the symptoms are having on your daily life. It will also depend upon whether you are in remission or are having a flare-up of your disease.
Medications
There are several medicines that can be prescribed in Australia for the treatment of ulcerative colitis.
Aminosalicylates
This kind of anti-inflammatory medication includes:
- sulfasalazine (brand names Salazopyrin, Pyralin);
- mesalazine (brand names Mesasal, Salofalk, Pentasa, Mezavant);
- olsalazine (Dipentum); and
- balsalazide (Colazide).
These medicines are available to take orally (as tablets, capsules or granules) and/or rectally (as an enema, foam or suppositories).
Aminosalicylates have a similar structure to aspirin and are often used to prevent relapse. This is called maintenance treatment and it has been shown that people on maintenance therapy with aminosalicylates often have fewer relapses (flare-ups) than other people.
These medicines can also help to control symptoms during a flare-up. Often your doctor will suggest you increase the dose during a flare-up, and possibly take a rectal preparation in addition to your oral medicine.
Common side effects associated with aminosalicylates include:
- headaches;
- nausea;
- diarrhoea; and
- abdominal pain.
Corticosteroids
For flare-ups or relapses, corticosteroids can be used to reduce inflammation. Steroids may be given as tablets to be taken by mouth or as enemas, foams or suppositories to be put directly into the rectum.
Mild attacks or attacks where only the rectum is involved are often treated with steroid enemas or rectal foam. If the inflammation is more severe or the colitis involves parts of the bowel which can’t be reached with enemas or suppositories, then steroid tablets can be prescribed.
Corticosteroids are not usually given for long periods, but as a short-term treatment for disease flare-ups. Long-term corticosteroid treatment is not recommended because it does not prevent flare-ups and is associated with side effects including:
- rounding of the face (moon face);
- weight gain;
- mood changes;
- thinning of the bones (osteoporosis);
- cataracts; and
- diabetes.
If you have a severe attack of ulcerative colitis, you may need treatment in hospital with intravenous corticosteroids.
Immunosuppressants
Immunosuppressants are medications that suppress the activity of the body’s immune system. They may be prescribed as maintenance therapy in people who have ulcerative colitis that is difficult to control.
Immunosuppressant medicines used to treat ulcerative colitis include:
- azathioprine (for example, Imuran, Thioprine);
- mercaptopurine (Puri-Nethol); and
- methotrexate.
Infliximab (brand name Remicade), adalimumab (Humira), golimumab (Simponi) or vedolizumab (Entyvio) are medicines that may be used if other medicines are poorly tolerated or ineffective.
Side effects can include:
- liver problems;
- tiredness;
- infections;
- nausea;
- increased risk of developing certain cancers; and
- low white blood cell count.
When taking some of these medicines, frequent blood tests are needed to check on your blood cell counts and liver function.
Other medications
Medicines for diarrhoea and pain are also often prescribed.
Surgery
If maintenance medicines don’t help and you are still having flare-ups and the disease is seriously affecting your quality of life, or if your colon shows evidence of changes which your doctor believes could lead to cancer, then surgery may be recommended. However, only a minority of people with ulcerative colitis require surgery.
Surgery usually involves removal of both your colon and rectum (proctocolectomy), followed by one of the options below.
Proctocolectomy with ileostomy
If both your colon and rectum are removed the surgeon may perform an ileostomy where the ileum (the part of the intestine before the colon and rectum) will be made to discharge its contents out of the body through a hole in the abdomen. A bag will need to be worn outside the body to enable the drainage of waste.
Proctocolectomy with continent ileostomy
This is a variation of the operation above. The colon and rectum are still removed, but the surgeon uses the ileum to construct a pouch inside the abdominal wall. There is a small opening in the person’s side and periodically the person must insert a tube to empty the pouch.
Proctocolectomy with ileoanal anastomosis
Alternatively, you may be able to have a different kind of operation that eliminates the need to use a bag altogether. A pouch is constructed from the end of the ileum and then attached directly to the anus, allowing you to expel your waste normally. However, this type of operation, which may be carried out in one or 2 stages, can result in frequent bowel movements in the long term.
Although the decision to have surgery will have to be carefully considered by you and your doctors, it does mean your condition should no longer be a problem.
Self-help
You may notice that some foods (particularly spicy or fatty foods or those which contain lots of fibre, such as fruits) make your symptoms worse when you are having a flare-up. If so, you should avoid these. However, you should not restrict your intake of dietary fibre as a matter of course.
Some people with ulcerative colitis lose weight and find it hard to maintain a healthy weight. Your doctor will advise you if you need to take nutritional supplements. Eating a healthy diet is very important if you have ulcerative colitis.
Blood loss in ulcerative colitis can lead to anaemia. If you become anaemic your doctor will probably recommend that you take iron tablets.
Although the disease can be disabling during flare-ups, people with ulcerative colitis are able to lead normal lives relatively free of symptoms during the times the disease is in remission. Medical treatment can greatly improve the quality of life for people with the condition, and research into new treatments is continuing all the time. For those few whose disease is disabling, surgery does represent a cure, although it often involves an ileostomy.
Can ulcerative colitis lead to cancer?
If you have widespread ulcerative colitis, your risk of developing colon cancer is higher than people who do not have ulcerative colitis. This is particularly true if you have had colitis for many years.
Your doctor will probably advise you to have regular examination by colonoscopy. Biopsies (small tissue samples) will probably be taken at the colonoscopy for microscopic examination to detect any changes in bowel tissue that might lead to cancer. Your doctor will advise you on how often you should have these examinations depending on how long you have had ulcerative colitis.
