Hyperparathyroidism is a condition where the parathyroid glands (found in your neck) make too much parathyroid hormone.
Parathyroid hormone helps regulate the amount of calcium in our bodies. Too much parathyroid hormone can cause raised levels of calcium in the body.
Hyperparathyroidism is 2 to 3 times more common in women than in men. Women between the ages of 50 and 60 years are most commonly affected.
Symptoms of hyperparathyroidism
There may be no symptoms at all in the initial stages. Hyperparathyroidism is often diagnosed on the basis of an abnormal calcium result from a routine blood test.
Symptoms, when they do occur, can be mild to start with, and include aches and pains or mild weakness and fatigue. Symptoms and signs are the result of the effect of calcium on the body.
- The kidneys are often affected, with the person passing large amounts of urine and feeling thirsty all the time. In about one-third of cases the high calcium levels will produce kidney stones, which can be very painful and can cause blood in the urine.
- High blood pressure can be present.
- Muscles are affected, aching legs and sore shins being common complaints. There may be generalised weakness and backache.
- Hyperparathyroidism can affect your bones, causing bone pain or weak bones that tend to fracture more easily — osteoporosis.
- If the digestive system is affected, abdominal pain, constipation, loss of appetite and nausea are the most common symptoms.
- Symptoms of mental health problems may also occur. There may be depression, confusion, personality changes, memory and concentration problems and, in severe cases, loss of consciousness.
Causes
The parathyroid glands are a group of 4 tiny glands situated in the neck, close to the much bigger thyroid gland. They produce parathyroid hormone, which is involved in regulating the levels of calcium, phosphorus and vitamin D in the body.
Hyperparathyroidism – too much parathyroid hormone in the body – can be either primary or secondary.
Primary hyperparathyroidism
In primary hyperparathyroidism, overproduction of parathyroid hormone can result from:
- a small, benign (non-cancerous) tumour, called an adenoma, on one of the parathyroid glands;
- enlargement of 2 or more of the parathyroid glands; or, very rarely,
- a malignant (cancerous) tumour of the parathyroid gland.
Secondary and tertiary hyperparathyroidism
Secondary hyperparathyroidism is when there is overproduction of parathyroid hormone in response to an underlying medical condition that is causing a low calcium level in your body. The parathyroid glands produce extra parathyroid hormone to stop your calcium level from getting too low. The most common cause of secondary hyperparathyroidism is chronic kidney failure. Vitamin D deficiency can also result in secondary hyperparathyroidism.
Over time, if left untreated, secondary hyperparathyroidism can cause ongoing overproduction of parathyroid hormone that results in elevated calcium levels – this is known as tertiary hyperparathyroidism. Tertiary hyperparathyroidism is not common.
Tests and diagnosis
Your doctor will ask about your symptoms and perform a physical examination.
Blood tests
A simple blood test can measure the level of calcium and phosphorus in your blood.
If high calcium and low phosphorus levels are detected, your doctor may recommend a blood test to check the level of parathyroid hormone in your blood. A raised parathyroid hormone level means you have hyperparathyroidism.
Imaging
Your doctor may recommend having an ultrasound scan of your parathyroid gland to determine the exact problem affecting the parathyroid gland(s).
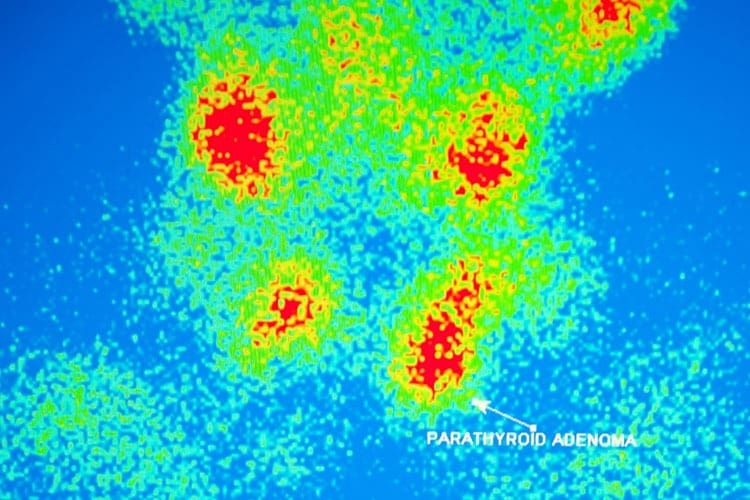
A special scan called a sestamibi parathyroid scan involves giving a small dose of a radioactive compound that is absorbed by the parathyroid gland so that the glands can be seen more clearly on a scan that detects radioactivity.
Other tests
If your doctor suspects you have secondary hyperparathyroidism, other tests may be needed to determine the underlying cause.
Other tests may also be needed to check whether high calcium levels have damaged your kidneys or caused osteoporosis.
Treatment of hyperparathyroidism
Most cases of primary hyperparathyroidism can be effectively treated with surgery to remove the affected parathyroid gland(s).
The treatment of secondary hyperparathyroidism depends on the cause.
Surgery
If there is a single adenoma in one gland, the gland containing the adenoma is removed. If there are enlarged, hyperactive parathyroid glands, the affected glands are removed.
Surgery can often be performed with very small incisions in the neck, allowing faster recovery.
Monitoring
In some cases of hyperparathyroidism, treatment is not needed but your condition will need to be monitored by your doctor. Suitable people are those who have no symptoms and are older than 50 years of age.
Regular blood tests to monitor your calcium level and kidney function, plus bone scans to check your bone density are usually recommended. Your doctor should advise you on a diet that’s not too high in calcium and on getting an adequate water intake (to reduce your risk of developing kidney stones).
Medicines
There is an oral medicine (tablet) available called cinacalcet (brand name Sensipar) that can be used in the treatment of hyperparathyroidism. It can be used to treat:
- secondary hyperparathyroidism associated with chronic kidney disease;
- primary hyperparathyroidism when surgery is not an option; and
- high calcium in people with parathyroid cancer.
Side effects of Sensipar may include nausea, vomiting, rash, diarrhoea and muscle pain.